As a practicing restorative dentist, the hardest part of an implant case often isn’t surgery day, it's the call months or years later when the patient reports tenderness, the crown feels “off”, and everyone wants to know what went wrong. Patients tend to label these situations as “bad dental implants”, but clinically you’re dealing with an implant that has failed or is trending toward failure.
This article focuses on the most common patterns behind problem implants and on what you can influence: assessment, surgery, prosthetic design, maintenance, and how you work with your lab. The emphasis is practical small upstream decisions that prevent stress later on.
TL;DR
- Most “bad” cases are either early failures (no osseointegration) or late failures driven by peri implantitis and/or mechanical overload, as summarised in an implant failure review.
- Key risk factors: history of periodontitis, poor plaque control, smoking, systemic disease, and lack of maintenance.
- Technical drivers: inadequate primary stability, poor positioning, excess cement, difficult cleansability, and occlusal overload on the implant prosthesis.
- Prevention hinges on better case selection, thoughtful surgical and prosthetic planning, and close collaboration with a digitally focused implant lab.
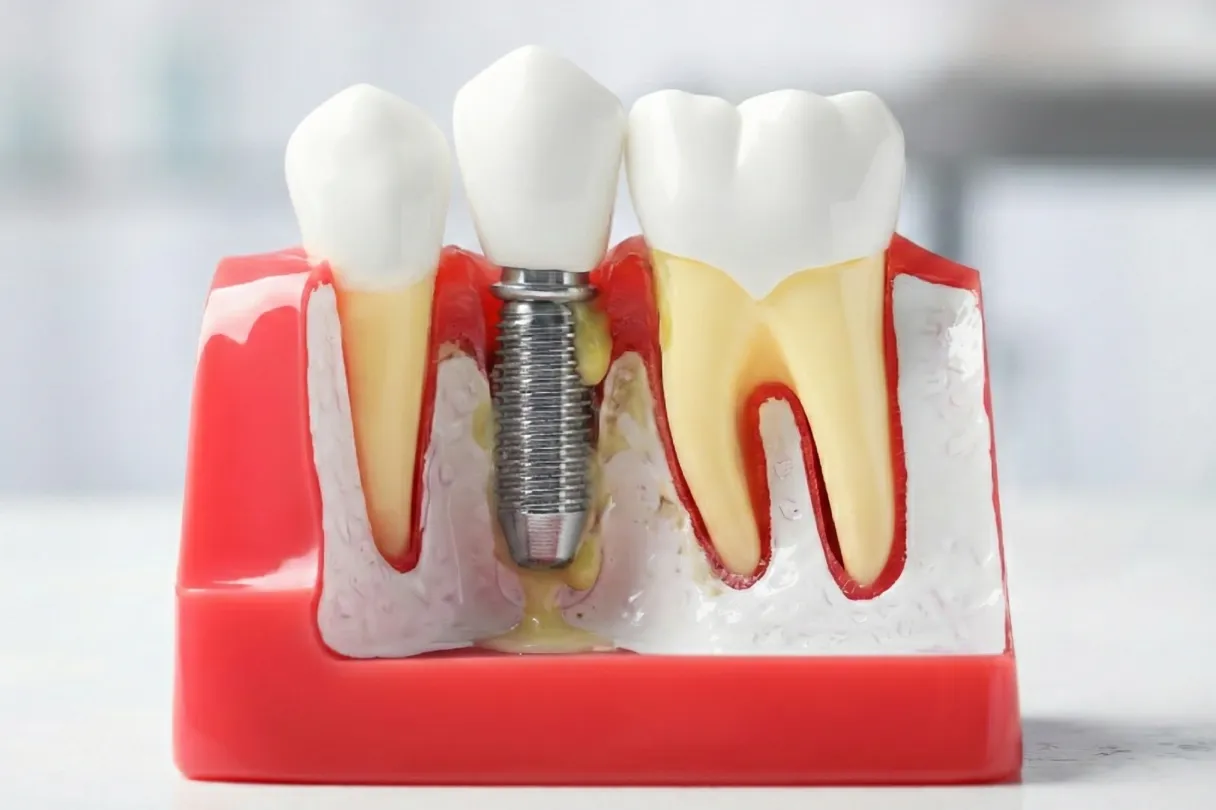
What do patients really mean by “bad dental implants”?
Clinically, you think in terms of early vs late failure, biological vs mechanical complications, and osseointegration vs peri implantitis, mirroring the framework used in an implant failure review. Patients don’t. For them, a “bad” implant is any case where:
- the implant had to be removed,
- the crown never felt right, or
- They keep needing repairs or hygiene visits just for that site.
Aligning those patient perceptions with your clinical framework helps when you audit your own cases. Ask: is this mainly a surgical issue, a prosthetic/lab issue, a maintenance gap, or a mix of all three?
Common causes of bad dental implants
From a clinical point of view, most “bad” implants cluster into a few repeatable patterns. The table below summarises them before we look at each in more detail.

Careful digital planning helps reduce early and late implant failures linked to positioning and site selection.
Risk factors → peri implant mucositis → peri implantitis → biological or mechanical failure
1. Patient and site risk factors
Consensus statements highlight a familiar cluster of risks for peri implant disease and failure: history of chronic periodontitis, poor plaque control, smoking, systemic disease (especially uncontrolled diabetes), bruxism, and lack of supportive maintenance.
- History of periodontitis
- Poor oral hygiene / plaque control
- Smoking
- Systemic disease (e.g. uncontrolled diabetes, immunosuppression)
- Bruxism and heavy occlusal load
Despite these risks, long term data remain reassuring for well selected, well maintained patients: systematic reviews with at least 10 years of follow up report implant level survival around 94 to 96%, while peri implantitis still affects roughly one in five patients and about 11 to 13% of implants over time; smokers appear to have substantially higher failure rates than non smokers.
Most “bad dental implants” aren’t about the implant brand they’re about the system around it: risk factors, positioning, design, and maintenance.
2. Surgical and planning errors (early failures)
Early failures usually occur when osseointegration never establishes properly. Reviews point to preventable factors such as thermal trauma to bone, poor primary stability, contamination, and placement in compromised sites.
- Over prepared or overheated osteotomy sites.
- Implant angulation that leaves a thin buccal plate or dehiscence.
- Immediate placement without adequate infection control or bone quality.
- Functional loading before the bone implant interface is ready.
From the patient’s perspective, these early losses feel no different from a late “bad implant” that fails years after restoration.
3. Prosthetic and lab related factors
Once osseointegration is stable, long-term success is driven largely by the prosthesis and occlusion. Common contributors to biological or mechanical problems include:
- Occlusal overload from poor fit or misaligned contacts.
- Residual subgingival cement around cement retained crowns.
- Bulky, non cleansable contours that trap plaque.
- Materials poorly matched to load in parafunctional patients.
These factors are repeatedly linked with increased peri implant bone loss, technical complications, and need for retreatment in narrative reviews and consensus reports.
A lab partner with consistent CAD/CAM workflows, accurate digital articulation, and implant experience can take much of this risk off the table. NovaDent’s workflows for custom abutments and implant crowns are built around tight fits, cleansable emergence profiles, and predictable occlusal schemes across major implant systems.
4. Maintenance and communication gaps
Even technically excellent work will suffer if the patient disappears after insert. Lack of structured recalls, no written implant specific hygiene instructions, or unclear responsibility between GP, periodontist, and surgeon are all associated with higher peri implantitis rates in consensus reviews.
How to reduce the risk of a failed dental implant
A simple way to think about prevention is the “4 Chain Implant Success Model”: patient biology, surgery, prosthetics, and maintenance. The stronger each link, the lower your risk of a “bad implant” case.

Close collaboration between the clinician and implant laboratory strengthens each link in the implant success chain.
1. Front load the case with honest risk assessment
A simple checklist at treatment planning stage goes a long way:
- Current or past periodontitis status and residual pocketing.
- Smoking status and willingness to reduce or quit.
- HbA1c or medical clearance for relevant systemic conditions.
- Bruxism, wear facets, existing splints, and parafunctional habits.
- Patient expectations and commitment to maintenance visits.
Documenting these factors not only protects you medico legally; it also makes it easier to discuss the small but real chance of failure even when everyone does their part.
2. Plan position, soft tissue, and occlusion digitally where possible
Many late “problem” implants started life slightly off in three dimensions. Cross mounting CBCT, intraoral scans, and a driven plan can minimize that. From a lab point of view, receiving clean, well labelled scans and a clear occlusal scheme lets the team design restorations that share load intelligently rather than punishing one fixture.
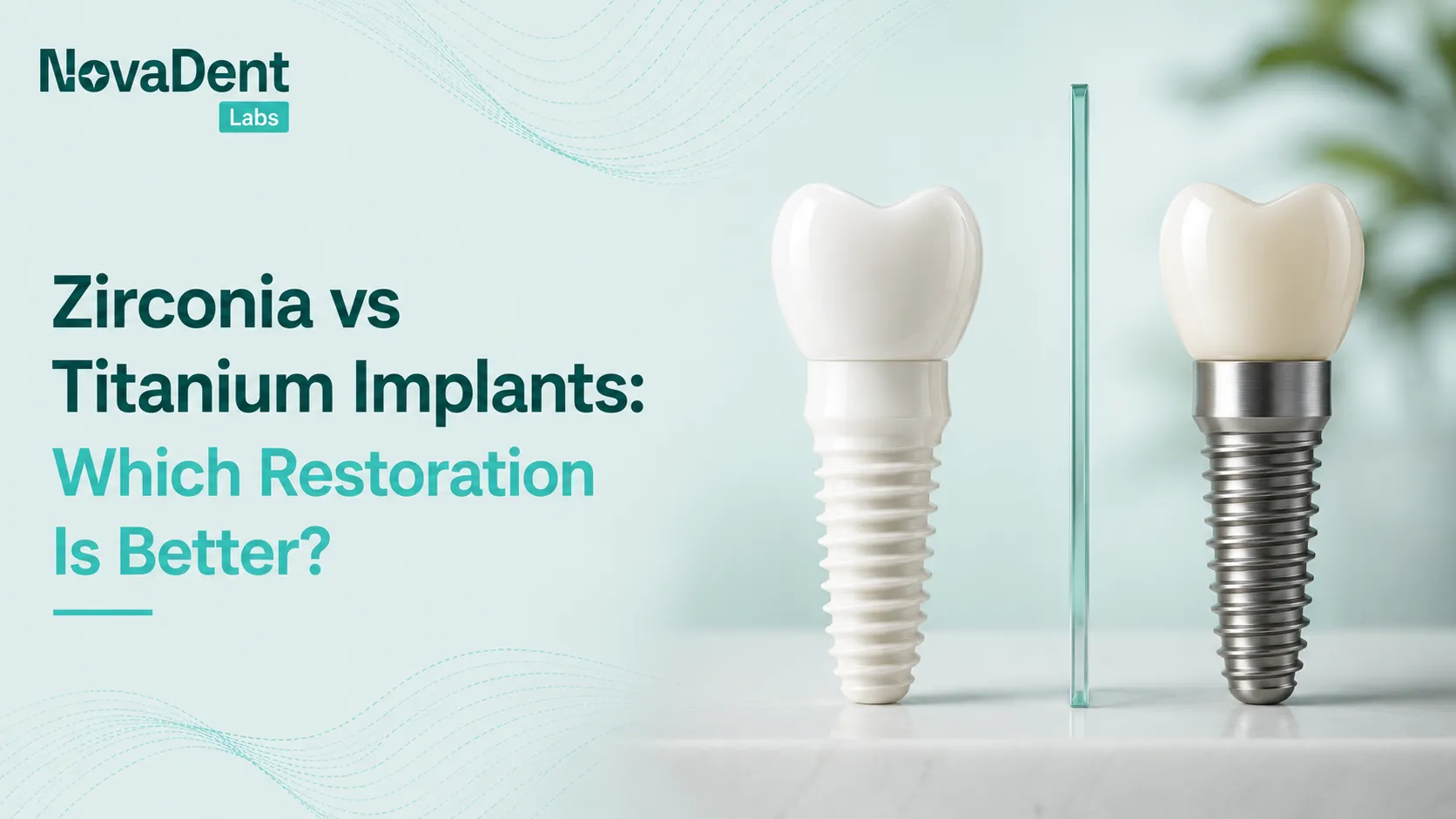
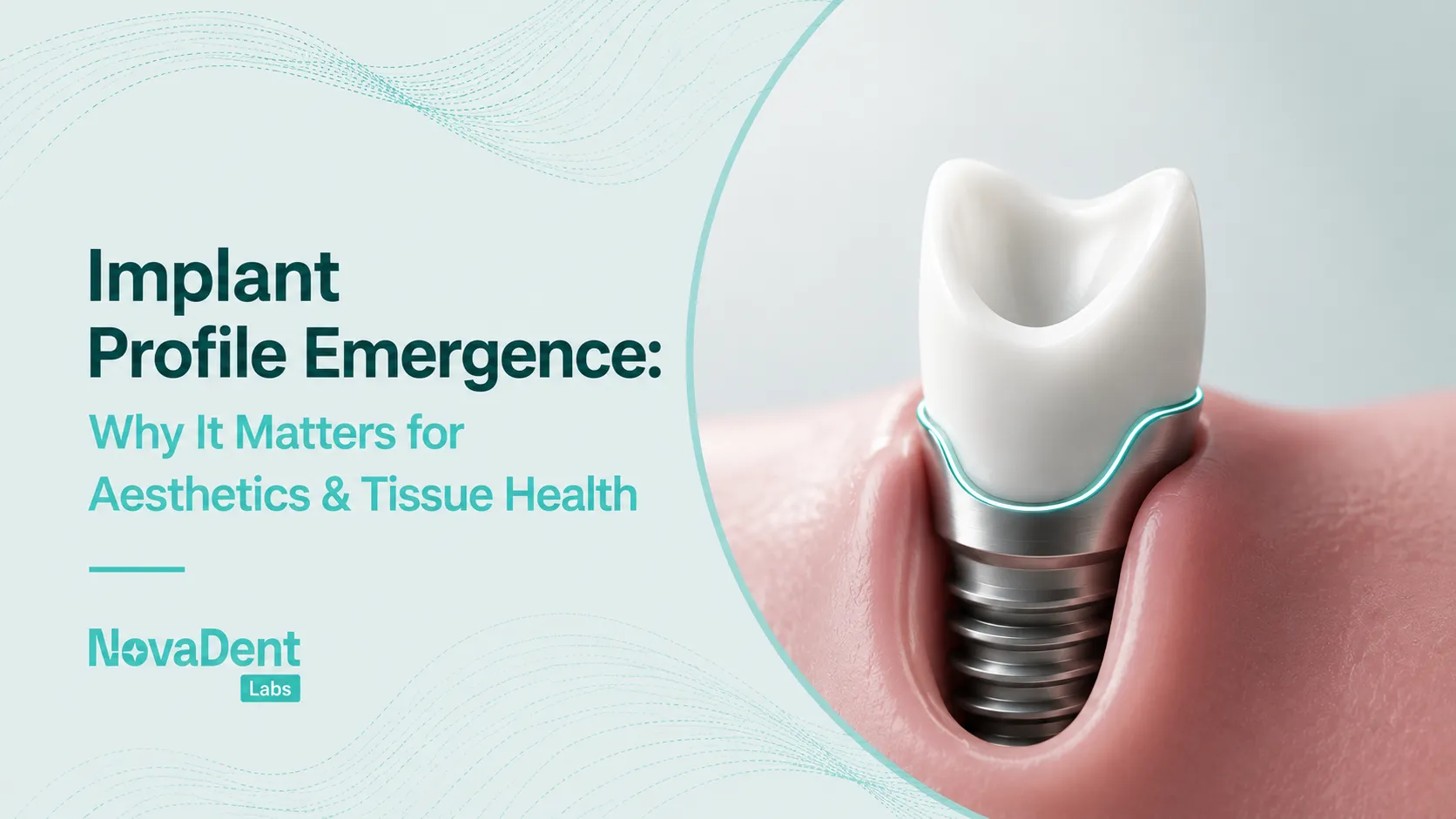
For example, NovaDent’s customised abutments are milled to create soft-tissue friendly emergence profiles and consistent margins, which supports cleansability and stable soft tissues. Similarly, their zirconia implant crowns offer strength and wear resistance for high load posterior cases.
3. Design for cleansability and maintenance
Peri implant mucositis is to peri implantitis what gingivitis is to periodontitis an early, largely reversible stage while inflammation is confined to soft tissue. MSD peri implant diseases Contour, access, and patient instruction therefore matter just as much as torque values.
- Favour screw retained solutions where access and system compatibility permit fewer cement issues and easier retrievability, consistent with consensus trends.
- Use emergence profiles that allow floss, brushes, or interdental aids to actually reach the critical areas.
- Set a clear maintenance interval and assign who owns reviews GP, periodontist, or shared care, echoing EFP guidance on prevention.
- For bruxers, prescribe and deliver a night guard once restorative work is completed; your lab can fabricate this alongside the final prosthesis. A digital appliances partner such as NovaDent’s occlusal splint service makes this easy to build into your workflow.
The worst part of dental implant complications
For many clinicians, the hardest part of implant problems is not the re-entry surgery, it is explaining complex biological and prosthetic issues to someone who mainly remembers a big investment of time and money.
Clear documentation of risk factors, shared responsibilities (surgery, prosthetics, maintenance, home care), and a trusted lab that supports you with remakes goes a long way toward preserving trust when things go wrong.
Key red flags and practical next steps
Whether you placed the implant or inherited it, some signs should prompt closer review:
Regular, structured reviews make it easier to catch early warning signs around dental implants.
- Bleeding or suppuration on probing around the implant, even in an otherwise asymptomatic patient.
- Increasing probing depths compared with baseline records.
- Crestal bone loss on serial radiographs beyond expected initial remodelling.
- Patients reported pain on biting, mobility, or a sense that “the tooth feels high”.
- Fractured screws, chipped ceramics, or repeated loosening episodes.
Early conservative steps typically include debridement, removal of excess cement, occlusal adjustment, and reinforcement of maintenance protocols, with more advanced cases requiring surgical management or explantation.
Patients facing resources such as the American Academy of Implant Dentistry’s information portal can also help align expectations and reinforce your explanations during these discussions.
FAQs
What typically causes a failed dental implant?
Most failed dental implant cases reflect a combination of host factors (periodontitis history, poor plaque control, smoking, systemic disease) and technical issues (surgical trauma, unfavourable positioning, excess cement, and occlusal overload) on a background of weak maintenance.
How long should a dental implant last?
With good case selection, execution, and maintenance, many implants function well for a decade or longer, but they should never be presented as a guaranteed “lifetime” solution. Longevity depends heavily on risk factors, surgical and prosthetic quality, and ongoing maintenance.
Can a “bad” implant be saved?
peri implant mucositis is often reversible with biofilm control and professional therapy; peri implantitis has a more guarded outlook and may require surgical intervention or removal. The earlier you intervene, the better your options.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website