
Choosing between Emax and zirconia crowns often starts with a clear chairside discussion of risks, aesthetics and longevity.
As a restorative dentist, you probably make more crown material decisions than you can count. Most days it feels simple: molars get something strong, anterior get something pretty. Then a bruxing patient asks for a flawless smile and the old patterns no longer feel so safe. The discussion about emax vs zirconia stops being theoretical and turns into remakes, fractures and extra appointments.
This guide speaks to that moment in the surgery when you pause mid prep and ask, “Which material will give this patient the best long term result?” We will walk through indications, prep design, bonding and real‑world trade offs so you can choose with more confidence, especially when you are working with a digital lab partner such as NovaDent Labs.
At a glance: zirconia vs emax
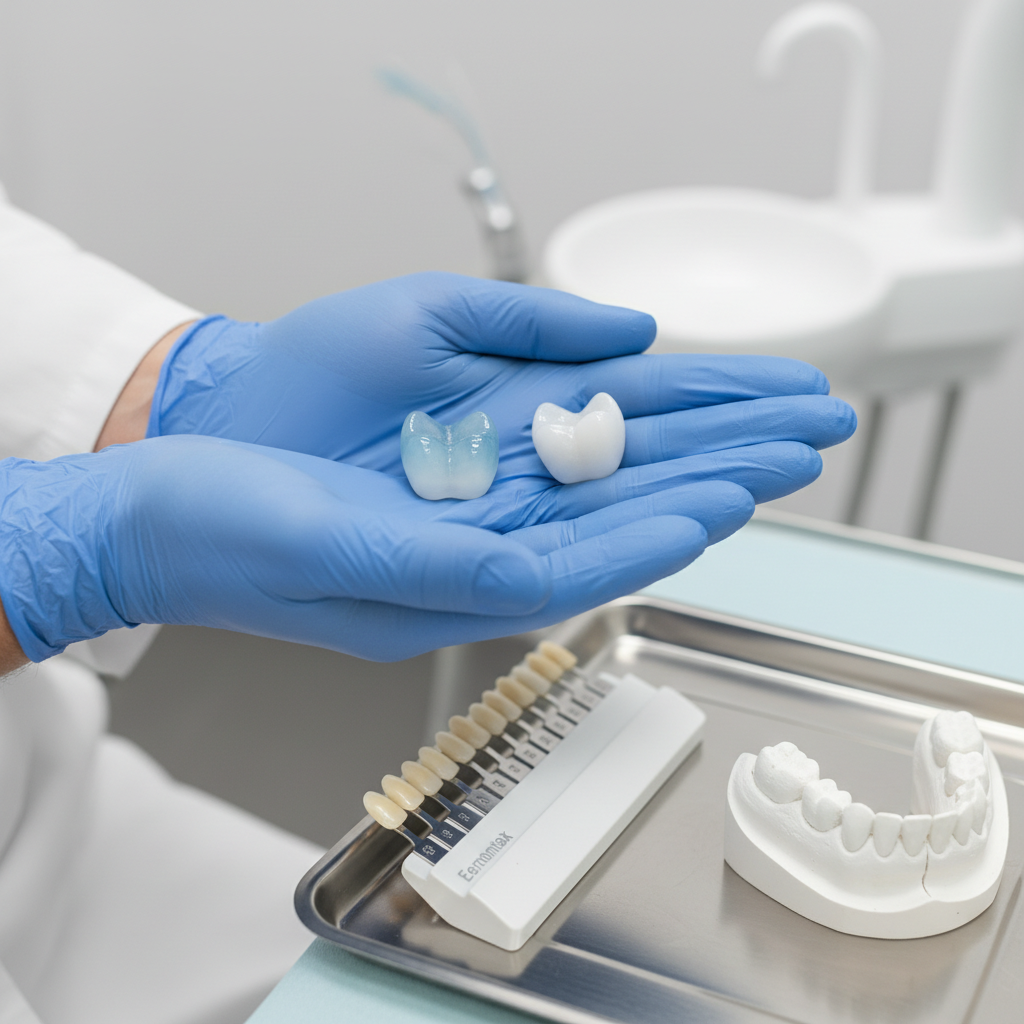
A quick visual comparison of ceramic crowns helps frame the differences between zirconia and Emax in everyday restorative practice.
TL;DR
- Zirconia is a high strength ceramic (yttria stabilised zirconia) ideal for high load posterior zones, bruxers and thin occlusal clearance.
- Emax (lithium disilicate glass ceramic) offers superior translucency and bonding for anterior, premolars and adhesive partial coverage work.
- The more functional risk (parafunction, minimal ferrule, short clinical crown), the more zirconia usually makes sense.
- The more the patient focuses on shade, translucency and blending with natural enamel, the more Emax earns its place.
- Preparation design and cement choice can matter as much as the material itself.
Clinical scenarios that favour zirconia vs emax
Think about the last mandibular molar crown you placed on a heavy grinder. In that setting, every extra megapascal of strength helps. Zirconia’s transformation toughened structure and high fracture resistance give you a wider safety margin when load is the main concern.
High‑load posterior units
Full contour monolithic zirconia crowns are well suited to:
- First and second molars in patients with strong masticatory forces
- Short span posterior fixed partial dentures
- Cases with limited ferrule or compromised tooth structure where retention is already challenged
Bruxism and parafunction
For bruxers, a zirconia crown gives a strong core with less chipping than older porcelain fused to metal designs. With careful occlusal adjustment and polishing, modern zirconia shows acceptable antagonist wear. Many clinicians now pair occlusal guards with zirconia posteriors for bruxers as a practical, long term combination.
Limited occlusal clearance
When vertical space is tight, a zirconia crown can often function at reduced occlusal thickness compared with lithium disilicate. That can spare you from aggressive additional reduction or elective endo on already stressed teeth. Always confirm specific minimal thickness recommendations with manufacturer guidelines and your lab.
For example, a 48 year old bruxing patient presented with a fractured PFM crown on a mandibular first molar and very limited occlusal clearance. After discussing the occlusal scheme and parafunction with the lab, the case was redesigned as a monolithic zirconia crown at a conservative occlusal thickness and protected with a night guard; at two year review the restoration and opposing dentition remained intact with no reported sensitivity.
When an Emax crown is the better choice
If you have ever placed a beautiful anterior crown only to have the patient say, “It still looks a bit dull,” you know how unforgiving the aesthetic zone can be. This is where Emax tends to shine.
Single anterior crowns and short spans
Lithium disilicate’s glass‑ceramic microstructure gives it a translucency that mimics natural enamel. That makes Emax a strong candidate for:
- Single unit central and lateral incisors where shade matching is demanding
- Upper canines that sit right in the smile line
- Short span anterior bridges where indication and occlusion permit
Veneers, onlays and partial coverage restorations
Because Emax is etchable, it bonds reliably to enamel and dentine when used with hydrofluoric acid etching, silane and resin cement. That combination supports minimal prep veneers, overlays and onlays where enamel preservation and adhesion matter. In many of these cases, zirconia would bring more strength than you need but less optical integration than you want.
Material properties: strength, translucency and bonding
From a materials science perspective, you can think of zirconia and Emax as very different ceramics. Zirconia is a polycrystalline material (yttria stabilised tetragonal zirconia polycrystal, or Y‑TZP). Emax is a lithium disilicate glass ceramic with an etchable glass phase.
That difference explains the clinical behaviour you see every day:
- Strength: Monolithic zirconia often reaches flexural strength values in the high hundreds of MPa, while lithium disilicate sits in the mid hundreds.
- Translucency: Emax lets light pass in a way that mimics enamel. Newer multilayer translucent zirconias narrow the gap but still tend to look slightly more opaque at similar thicknesses.
- Bonding: Emax can be etched and bonded like other glass ceramics. Zirconia relies on micromechanical retention and chemical bonding via MDP containing primers or resin cements, or on conventional luting with adequate macro retention.
For detailed scientific background, many clinicians refer to materials guidance from bodies such as the Australian Dental Association and manufacturer manuals for IPS e.max and dental zirconia systems.
Preparation, cementation and occlusal adjustment
Two dentists can use the same material and see very different outcomes simply because their prep and cementation protocols differ. Material choice and tooth preparation belong in the same conversation.
Careful planning of crown thickness, margins and cementation protocol is just as important as whether you choose zirconia or Emax.
Typical preparation guidelines
- Zirconia crowns: Often permit slightly less occlusal and axial reduction (for example, around 1.0 mm occlusal, 0.8 to 1.0 mm axial in low risk zones), with rounded internal line angles and a chamfer or shoulder.
- Emax crowns: Generally need more space for both strength and natural translucency (commonly 1.5 to 2.0 mm occlusal and 1.2 to 1.5 mm axial, depending on position and indication).
These numbers are broad guides only; always follow the specific instructions from your chosen system and discuss borderline cases with your lab. For lithium disilicate, that means checking the latest IPS e.max IFU before relying on minimum thicknesses.
Cementation considerations
- Zirconia: Works well with resin modified glass ionomer in many cases with strong mechanical retention. Where retention is compromised, MDP containing resin cements and primers support chemical bonding to the zirconia surface.
- Emax: Typically benefits from adhesive bonding after HF etch, silane and resin cement, particularly for partial coverage work and short clinical crowns.
A quick email to your lab with prep photos or intraoral scans can save a remake when you are deciding how far to reduce or which cement protocol will suit a specific case. At NovaDent’s fixed prosthetics service, for example, the team regularly reviews scans and suggests thickness and material combinations for tricky cases.
Longevity, fracture and wear: what the evidence shows
Both zirconia and Emax have strong clinical track records when used within their indications. Recent systematic reviews of tooth supported single crowns report 5 year survival rates in the high 90% range for both monolithic lithium disilicate and monolithic zirconia when cases are appropriately selected. systematic review data Zirconia’s performance is particularly strong in posterior regions and as frameworks for fixed partial dentures.
One point that often surprises patients is antagonist wear. Polished zirconia tends to be kinder to opposing enamel than rough, glazed zirconia. So if you place zirconia crowns routinely, giving each unit a careful polish after occlusal adjustment is almost as valuable as the material choice itself.
For clinicians who like to see the numbers, a quick literature search on PubMed for “lithium disilicate zirconia crown survival” brings up multiple cohort studies and reviews that you can skim between patients via PubMed.
Patient centred factors: aesthetics, cost and expectations
Technical arguments aside, the best material is the one that fits the patient sitting in your chair today. Two people with identical occlusions can still want very different things from a crown.
- Aesthetics: Highly demanding anterior patients, especially those focused on fine shade differences, often respond better to Emax. Zirconia in the anterior can look very good, especially multilayer systems, but tiny mismatch is more noticeable there.
- Budget: Your lab’s fee schedule, your own pricing and the patient’s circumstances all play a part. Some clinicians use zirconia for most posteriors and reserve Emax for cases where its optical advantages clearly change the outcome.
- Time and chairside adjustments: Well designed zirconia and Emax crowns from a digitally focused lab tend to seat with minimal trimming. If you find yourself re adjusting one material more often, that is a useful data point to discuss with your lab.
Setting expectations early helps. A quick explanation along the lines of “This option is stronger; this one blends a bit more with your natural tooth” goes a long way in shared decision making.
Working with your lab on material selection
Material selection is much easier when your lab team sees the same clinical picture you do. Digital impressions, photographs and a short note about parafunction or patient priorities help the lab make specific suggestions instead of generic ones.
As a digital first Sydney lab, NovaDent Labs receives intraoral scans from most major systems and uses CAD/CAM workflows for both zirconia and Emax crowns. That allows consistent thickness, controlled emergence profiles and predictable contacts, which in turn reduces your adjustment time regardless of material.
If you are reviewing your own crown menu or fee schedule, asking your lab for a simple “posterior zirconia vs emax” comparison by indication can be helpful. NovaDent can share turn around times, typical layer choices and a current fee guide when you request a price list, so your clinical preferences line up with the lab’s strengths.
Decision checklist: zirconia crown vs emax (6 Q Crown Checklist)
When you are chairside and time is short, running through a simple mental checklist keeps decisions consistent. We call this the 6 Q Crown Checklist:
A structured checklist helps turn the Emax vs zirconia decision into a repeatable process rather than a case by case guess.
- Zone: Is this a high load posterior or a highly visible anterior?
- Parafunction: Does the patient clench, grind or have a history of fractures?
- Tooth structure: Is there enough height and ferrule for mechanical retention?
- Space: How much occlusal and axial reduction is realistically possible?
- Aesthetic demand: How precise does the shade match need to be?
- Bonding: Will you bond adhesively or lute conventionally?
In many busy general practices, this translates roughly into: zirconia for high load posteriors and compromised retention; Emax for the aesthetic zone and adhesive partial coverage work. The question “zirconia crown vs emax” becomes less of a debate and more of a repeatable process.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website




