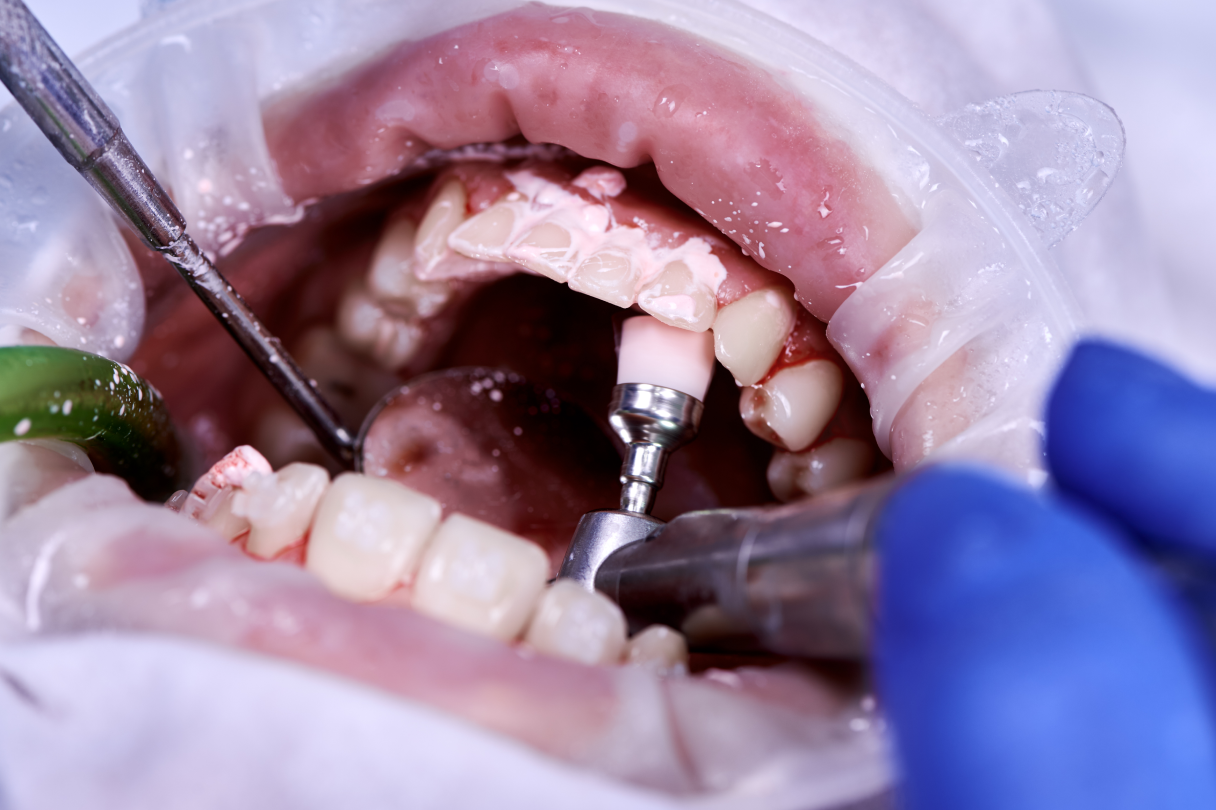
You seat a new lower denture, the occlusion looks reasonable, phonetics are acceptable, the patient smiles in the chair and thanks you. The next morning, the receptionist gets the call: “Doctor, I can’t chew on this at all.” Every dentist has lived that story.
Edentulous patients test every part of our skill set: diagnosis, anatomy, occlusion, communication and expectation management. When the case is a severely resorbed ridge, limited vertical space, or a mix of lost and remaining teeth, the stakes rise quickly.
At NovaDent Labs, we see these challenging full and partial edentulous cases every week. The basics still matter border molding, jaw relations, tissue management but digital workflows now give you a level of control and repeatability that simply wasn’t possible a decade ago.
In this guide, you’ll see exactly how to use digital workflows to make complex edentulous cases more predictable, with fewer remakes and far fewer “Doctor, I can’t chew on this at all” phone calls.
TL;DR
- Define what is edentulous clearly for each case (fully vs partially edentulous arch, edentulous space around key teeth).
- Use CBCT, intraoral scanners, and digital jaw relation tools to record anatomy and function, not just “a bite.”
- Plan tooth position, VDO and implant positions digitally with your lab before you pick up a bur.
- Send full records (photos, scans, old dentures, bite blocks) so your lab can design for stability and phonetics, not just aesthetics.
- For your toughest edentulous teeth cases, co-plan with a prosthodontist and a digital lab from day one.
1. What is edentulous?
In simple terms, an edentulous area is a part of the mouth where teeth are missing. That might be:
- a completely edentulous maxilla or mandible,
- a single edentulous space in a quadrant, or
- a long-span area with only a few remaining abutment teeth.
Patients will often ask, “So what is edentulous exactly does it mean I have no teeth at all?” You and I know that edentulous teeth is a slightly clumsy phrase; what we really mean is a site with absent teeth that needs a prosthetic solution: complete dentures, partials, or implant restorations.
From a lab perspective, what matters most is how that edentulous space relates to:
- available bone and soft tissue,
- opposing occlusion, and
- the patient’s desired function and aesthetics.
If those three elements are clear and well recorded, even a difficult case becomes far more predictable.
2. Why complex edentulous cases feel so hard
2.1 Clinical challenges
Long-term edentulism often means:
- advanced residual ridge resorption (especially in the mandible),
- knife-edge ridges or undercuts,
- mobile mucosa or flabby tissue in the anterior maxilla, and
- loss of vertical dimension and altered facial support.
Add in a few remaining teeth with poor prognosis, and you’re planning around what to keep, what to extract, and how to transition to a fixed or removable solution. Every decision you make here has knock-on effects for the lab.
2.2 Human factors
Many edentulous patients have a long history of “bad dentures” and repeat adjustments. They come in tired, frustrated, and worried about cost. They’ve Googled full-mouth implants and seen perfect smiles on Instagram.
This is where a clear digital plan helps. When you can show a virtual tooth setup or a 3D-printed try-in from your digital workflow, the conversation shifts from vague promises to concrete options and trade-offs.
For background on how common edentulism really is and why expectations keep rising have a look at the edentulism overview on StatPearls (NCBI). Recent World Health Organization estimates suggest that roughly 23% of people aged 60 years and older are completely edentulous worldwide, and this degree of tooth loss is linked with reduced chewing function and quality of life (World Health Organization oral health fact sheet).
3. Digital tools that change edentulous treatment planning
3.1 Intraoral scanners and CBCT
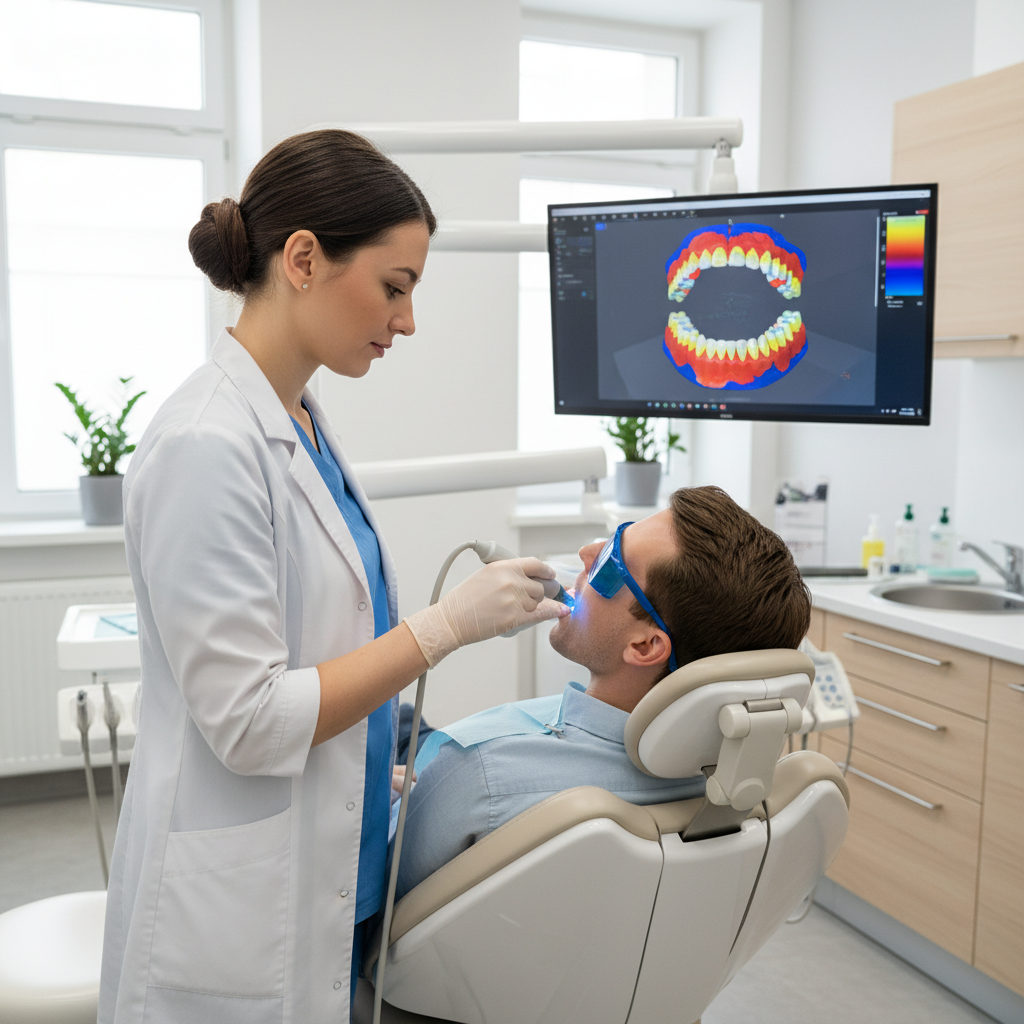
Ten years ago, full edentulous arches meant alginate or elastomer and a lot of hope. Today, high-quality intraoral scanners can capture arches and occlusion with surprising detail, especially when combined with border-molded custom trays and scan bodies.
When you pair that with a CBCT, your lab can:
- visualise bone volume under the edentulous space,
- plan implant positions relative to the planned tooth setup, and
- design surgical guides and provisional prostheses in a single workflow.
At NovaDent, we routinely merge implant restorative designs with CBCT data to help clinicians time extractions, immediate placement, and loading protocols more safely.
3.2 Digital jaw relation and VDO
Getting vertical dimension and centric relation right has always been the art of denture work. You still need clinical judgment, but digital tools let you record and verify:
- facebow or virtual facebow records,
- reference photos with ruler or lip support markers, and
- phonetic checks at try-in that can be adjusted in software.
Instead of sending a wax rim and a few scribbled notes, you can send photos, scan files and a short chairside video. Your lab can then adjust the virtual setup before printing a new try-in, instead of you starting again from scratch.
3.3 Virtual tooth setup for every edentulous space
Whether it’s a single edentulous space in the anterior or a full-arch restoration, virtual tooth setup lets you:
- test different tooth positions and occlusal schemes,
- check lip support and smile line with patient photos, and
- spot areas where you’ll have acrylic bulk issues or limited restorative space.
This is especially useful in cases mixing overdentures, fixed bridges and remaining natural teeth. The digital model forces you to think in 3D about how those pieces will meet in function.
4. A practical digital workflow: from edentulous space to stable prosthesis
Here’s a straightforward three-step framework we use with dentists for both fully and partially edentulous cases: Assess → Design → Deliver.
4.1 Assess: records that set you up for success
For a complex edentulous case, we recommend sending:
- full-arch scans or quality impressions (plus bite registration),
- CBCT data where implants are planned,
- photos (frontal at rest, full smile, 45° views, retracted occlusal),
- any old dentures that “almost worked,” and
- a short written summary of the patient’s main complaints and goals.
A short note such as “hates palatal coverage but accepts bulk in posterior, prioritises chewing over appearance” can shape the entire design; we see this daily in our denture and overdenture work.
4.2 Design: co-planning with your lab
Once the records land, your lab can:
- create a virtual wax-up or try-in for the edentulous teeth area,
- mock up implant positions and multi-unit abutments where relevant, and
- check for collisions, cantilevers and areas of thin acrylic or zirconia.
Many clinicians now prefer a digital “design review” call screen-share the case, agree on tooth position and occlusal scheme, then green-light the printable try-in. This 20-minute step often saves you two appointments.
4.3 Deliver: test, tweak, finalise
With a printed try-in or PMMA provisional, you can:
- test phonetics and aesthetics under real speech and expression,
- use pressure indicator paste to refine pressure areas, and
- mark any chairside adjustments directly on the provisional.
Those data go back to the lab, and the final prosthesis is milled or printed with those refinements baked in. Less grinding at insertion, fewer sore spots, and a lot fewer weekend phone calls.
5. Common clinical scenarios we see at the lab
5.1 Severely resorbed lower ridge with unstable dentures
The classic nightmare case. Here, even the best conventional denture will have limits. Digital planning lets you:
- evaluate if two to four interforaminal implants are feasible,
- design an implant-retained overdenture with proper bar or locator placement, and
- plan soft tissue support and flange extension before surgery.
We often use the same scan data to design both a surgical guide and a conversion prosthesis, keeping surprises to a minimum.
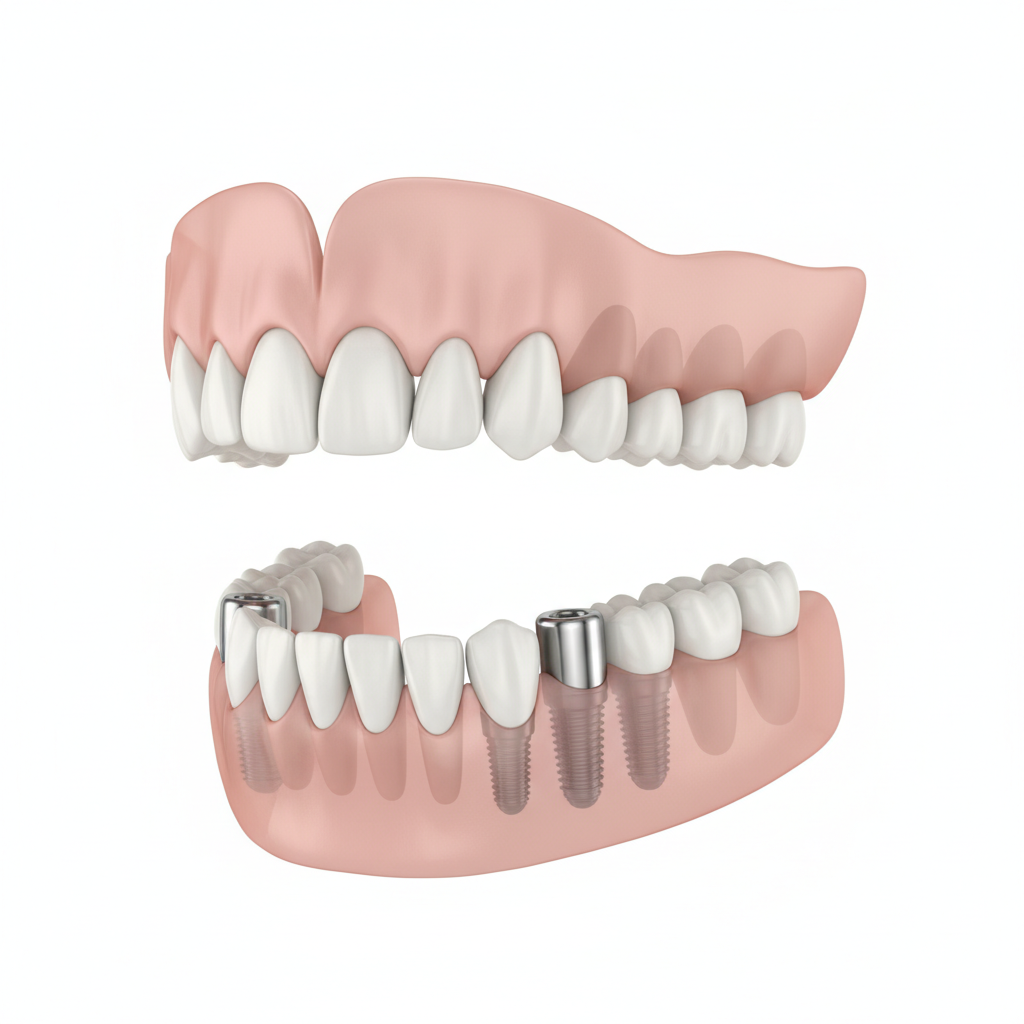
This approach is supported by long-term data: implant-retained mandibular overdentures typically show implant and prosthesis survival rates around 95% after 4–5 years, together with substantial improvements in patient satisfaction and oral health-related quality of life in clinical cohort studies (implant-retained overdenture outcomes study).
5.2 Long-span partially edentulous space with drifting teeth
In these cases, remaining teeth may have migrated, tipping into the edentulous space and compromising restorative room. A virtual setup lets you:
- decide whether limited orthodontics is worthwhile,
- see if a short-span bridge plus a small RPD will be more stable, and
- test whether implants will give you better long-term function.
A detailed discussion with your lab and, if needed, an orthodontist can turn a messy quadrant into a well-planned restorative area.
5.3 Full-arch fixed prosthesis on edentulous teeth sites
Full-arch fixed cases bring their own challenges: limited restorative space, phonetics, hygiene access and fracture risk. A digital workflow makes it easier to:
- choose between zirconia, PMMA over titanium, or hybrid designs,
- plan screw access channels away from aesthetic zones, and
- verify that the design respects lip support and cleansability.
For more global guidance on full-arch planning, the online consensus statements from organisations such as the ITI are worth keeping bookmarked.
6. Working with a digital lab for predictable outcomes
6.1 What to send your lab
For any challenging edentulous case, we suggest treating your lab submission like a mini case presentation. Alongside scans or impressions, include:
- a simple written diagnosis and treatment goal,
- photos and, where possible, CBCT data,
- notes on previous dentures or provisional restorations, and
- your timeline and budget constraints.
A consistent case submission checklist in your practice aligned with NovaDent’s online case submission form can standardise this so your team does most of the preparation.
6.2 Simple habits that reduce remakes
“The single best way to cut remakes is not new material, it's better records and clearer instructions.”
In our experience, these three habits save the most headaches:
- Over-communicate early. One extra photo or note is cheaper than one extra appointment.
- Standardise materials. Use a small set of impression and bite registration approaches so you and your lab speak the same language.
- Review the design. A quick design review call or annotated PDF catches issues before milling.
Over time, this turns your lab relationship into an extension of your clinical team rather than a black box that “just makes teeth.”
7. When to bring in a specialist or co-plan
Some edentulous cases are better handled in a team. Good candidates for prosthodontic or surgical input include:
- severe skeletal discrepancies where orthognathic options are on the table,
- patients with medical issues affecting healing or bone quality,
- redo full-arch cases with failed implants, and
- patients with very high aesthetic demands and limited restorative space.
A digital plan shared between you, the specialist and the lab keeps everyone aligned. Your lab can provide digital wax-ups, guide designs and even mock-ups for patient communication.
If you’re considering more advanced airway-focused appliances alongside dentures for example, for a patient with sleep-disordered breathing you may also want to look at options such as NovaDent’s SOMA appliance in the broader treatment plan.
8. Getting started with NovaDent Labs
Complex edentulous cases don’t have to mean endless adjustments and awkward follow-up calls. With the right records and a digital-first lab partner, you can offer:
- more accurate try-ins and fewer remakes,
- clearer treatment options for full and partial edentulous teeth cases, and
- a smoother journey from first consult to final prosthesis.
If you’d like to see how our Sydney-based team supports clinicians across Australia with digital dentures & implants, reach out for a chat or case review.
You can Request Price List to understand fees, turnaround times and available materials, or contact us directly with a de-identified case and we’ll suggest a practical digital workflow.
The next time you face a tough edentulous space, you don’t have to guess alone bring your lab into the planning from day one and share the load.
Key takeaways
- Use clear definitions of edentulous areas (full arch vs local edentulous space) to frame treatment choices.
- Combine scans, CBCT and digital jaw relation tools for detailed planning and fewer surprises.
- Involve your lab early with photos, notes and design reviews to reduce remakes.
- Call in specialist support when skeletal, medical or aesthetic factors raise the stakes.
- Partnering with a digital-focused lab like NovaDent Labs makes challenging edentulous cases more predictable for you and more comfortable for your patients..

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website