For many of your patients, scattered failures and a collapsed bite sneak up over decades. The turning point is often when patchwork dentistry no longer holds together and you start thinking about full mouth rehabilitation. At that point, the quality of your lab partnership shapes everything: how confident you feel presenting the plan, how restorations seat, and how many “fifth appointments” you end up booking.
This article looks at lab side decisions that matter most in complex reconstruction: records, occlusion, materials, digital workflows, and how to reduce surprises in full-arch and implant cases before you go to final.

TL;DR
- The lab can only design to the level of detail you send. Complete records and clear intent beat “fix it at the try in” every time.
- Material choice, occlusal scheme and vertical dimension are easiest to tune in staged provisionals, not once zirconia or metal ceramic is on the articulator.
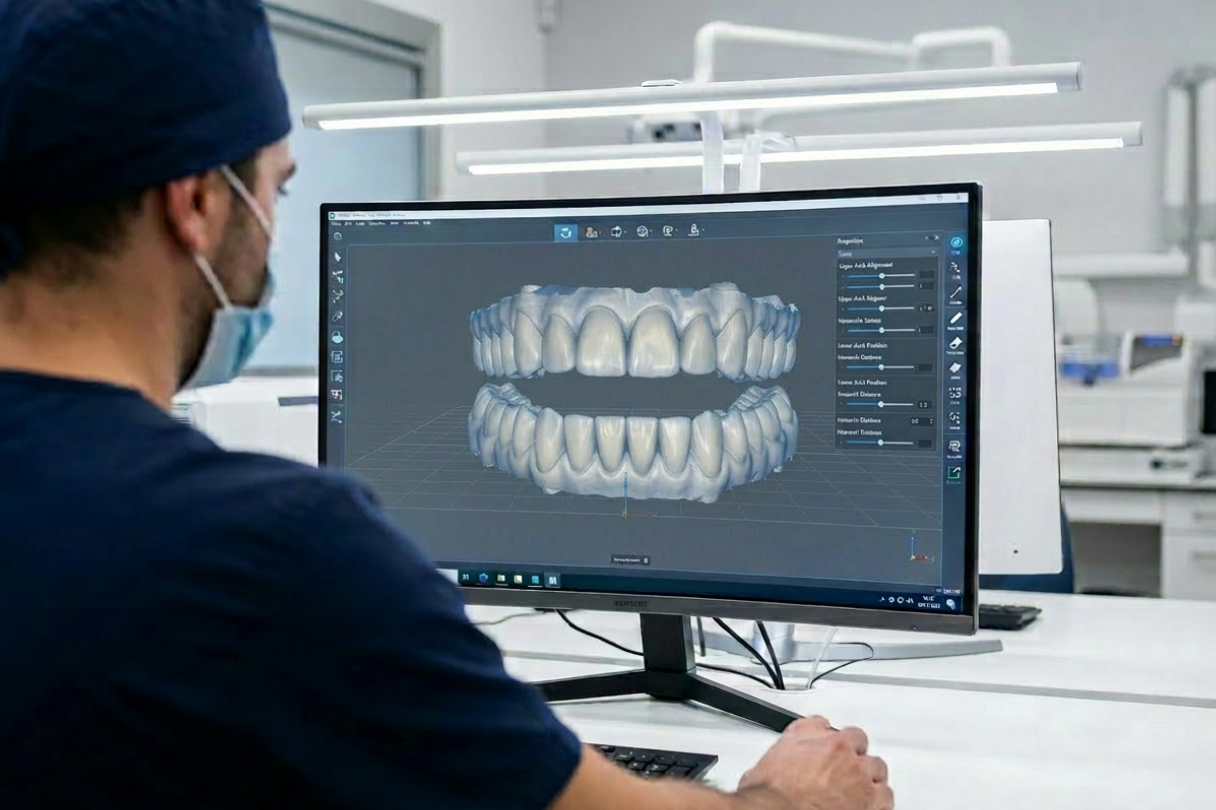
- Shared digital workflows with a trusted lab help you manage risk in full arch and hybrid implant cases while keeping chairside adjustments manageable.
When should you consider full mouth rehabilitation & reconstruction?
Every clinician has met the patient whose dentition looks like a history lesson in past dentistry: multiple materials, drifting contacts, posterior collapse and TMD complaints. The question becomes, “Can I keep repairing, or do I reset the system?”
Typical indications for comprehensive rehabilitation include:
- Generalised severe tooth wear or erosion with loss of vertical support
- Combination of failing endodontic work, fractures and hopeless prognoses across arches
- Full arch edentulism or near edentulism, especially in implant candidates
- Longstanding functional issues (muscle pain, broken provisionals, chipping restorations) despite localised repairs
For these patients, you are rebuilding occlusion, aesthetics and function as a system, so the lab becomes a planning partner rather than a passive manufacturer.
Why the lab partnership shapes complex outcomes
On paper, two labs may both offer crowns and bridges, dentures and implants. In complex cases, the difference is usually in how they think with you. Do they question the VDO you have chosen, query the occlusal scheme, and suggest alternatives when restorative space looks tight? Or do they simply accept impressions and “make it fit”?
A collaborative lab should help you:
- Translate clinical findings into a diagnostic wax up or digital set up that respects occlusal principles
- Plan implant number and distribution in line with consensus guidance (for example, a minimum of four well distributed implants for a one piece full arch fixed prosthesis, as recommended in the ITI implant number consensus).
- Choose materials that suit parafunction, aesthetics, opposing dentition and available restorative space
- Stage the case with interim appliances and long term provisionals, not leap straight to definitive prostheses
At NovaDent, this is where digital tools (CAD/CAM, AI-assisted design and virtual articulation) sit alongside human judgement, rather than replacing it.
What the lab needs for predictable full mouth rehabilitation implant cases
Whether you are planning tooth borne rehabilitation or a full mouth rehabilitation implant case, the lab can only design what it can see and verify. Thin instructions on the sheet usually turn into thick adjustment appointments.
Core records for all comprehensive cases
- High quality upper and lower intraoral scans (or well poured stone models) with accurate centric relation records
- Facebow or virtual facebow-equivalent information when possible, especially in restorative dentistry that alters VDO
- Full face and intraoral photographs (rest, smile, retracted, occlusal views) with shade tabs for reference
- Clear notes on desired occlusal scheme (mutually protected, group function, lingualised for dentures, etc.)
- Diagnostic wax up or digital design approved by you and, ideally, tested with provisionals
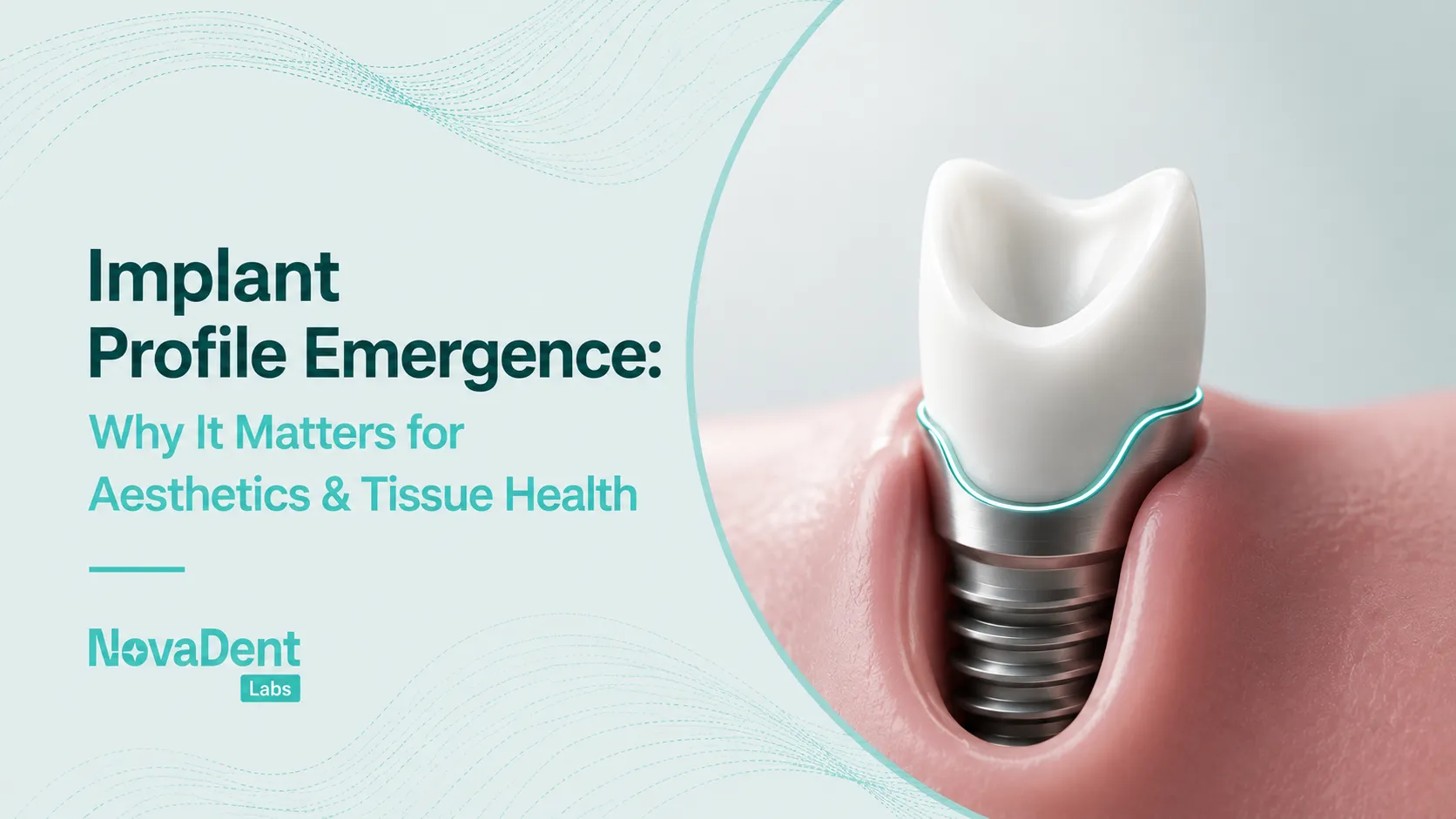
Additional records for implant supported or hybrid cases
- CBCT data (DICOM) with restorative driven implant planning, not just “bone driven” placement
- Information on multi unit abutments, tissue depth and any angulation corrections
- Photographs showing smile line, lip support and any gingival display concerns
- Requested prosthesis type (fixed, fixed removable, bar overdenture, All on 4 style) and any cantilever limits you want respected
When these records are complete, a lab like NovaDent can help you co-plan the case and suggest whether to stage with immediate load PMMA, removable prostheses or segmented approaches.
For more detail on how we receive digital files, see our intraoral scanner connection guide.
Material selection for full arch and mixed cases
Material decisions in comprehensive work are rarely one size fits all. You are often balancing aesthetics, parafunction, opposing materials, restorative space and retrievability. The lab’s job is to surface those trade offs before you are locked in.
Tooth borne full arches
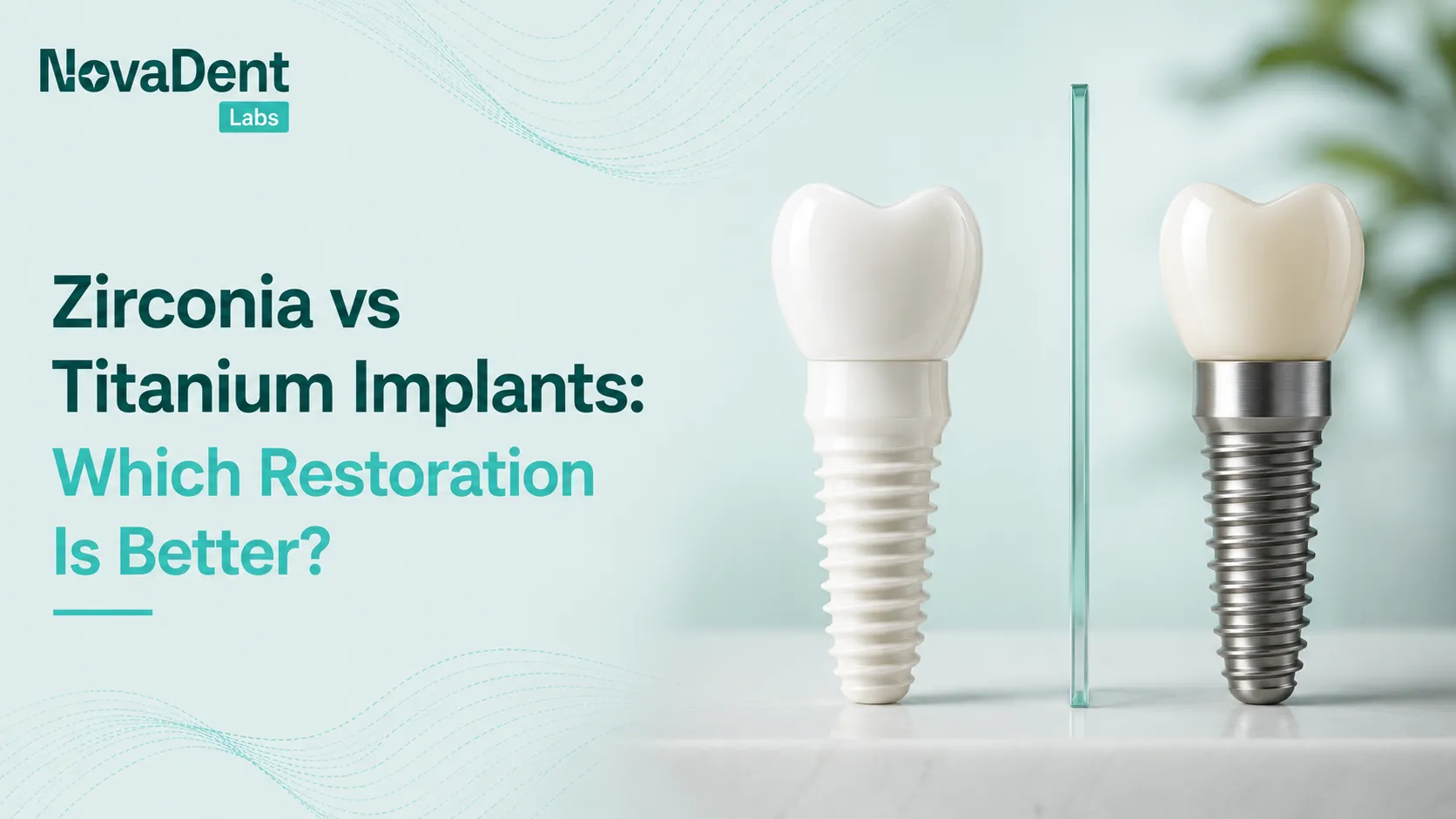
- Layered zirconia or lithium disilicate veneers/onlays: useful in younger wear patients with high aesthetic expectations and reasonable enamel support.
- Zirconia crowns/bridges: high strength, good for bruxers when designed with protective occlusion, studies show solid long term survival but note substantial veneering ceramic chipping when heavy layering is used. In an 8 year pilot of mandibular full arch zirconia FDPs, all prostheses survived, but approximately 40% of veneered units showed porcelain fracture.
- Metal ceramic: still a workhorse where space is limited or in posterior segments that will not be highly visible.
Full arch implant supported prostheses
- Monolithic zirconia on multi unit abutments: favoured for strength and aesthetics, requires adequate prosthetic space and thoughtful design of connectors and occlusion.
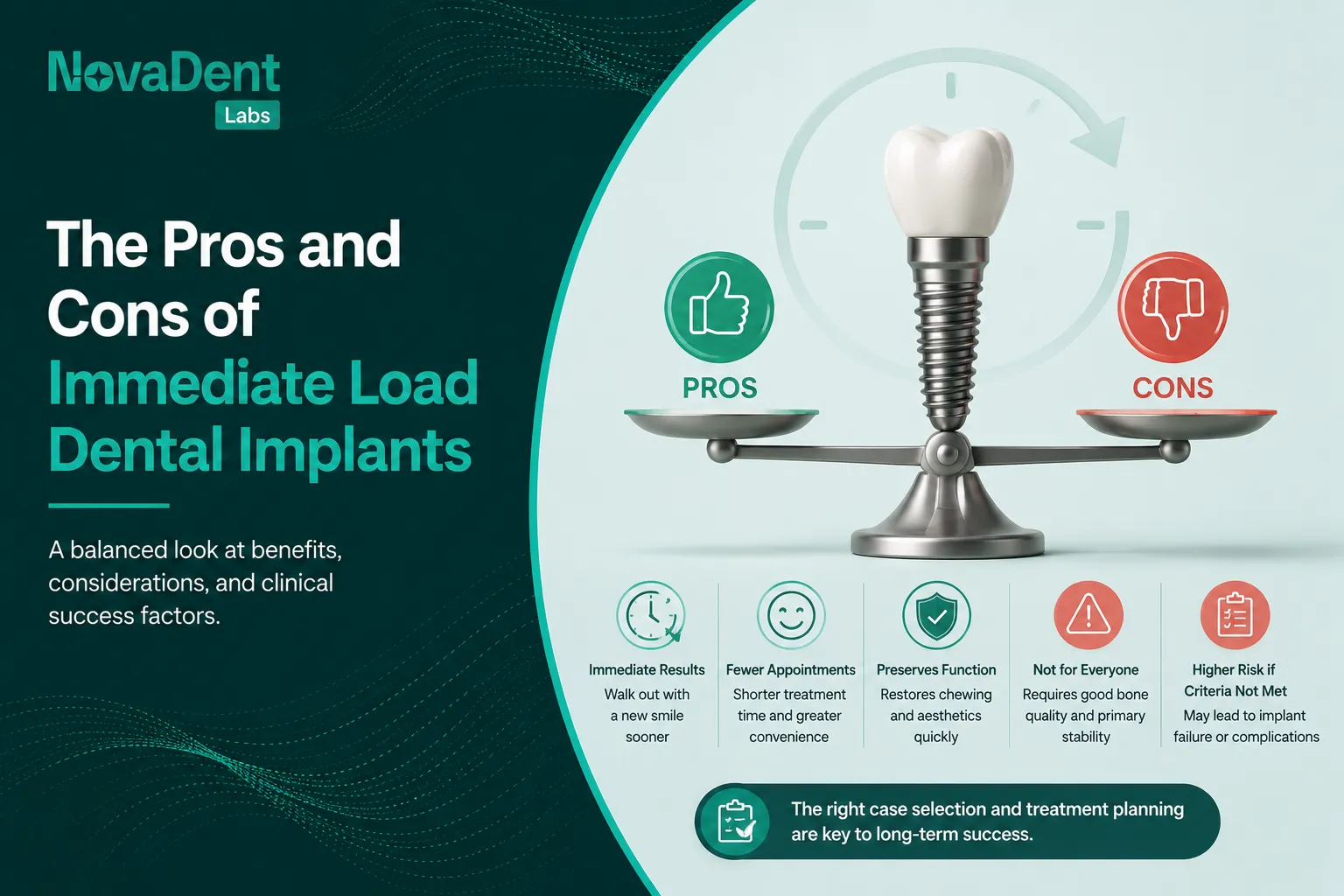
- High impact PMMA or composite hybrids: useful as long term provisionals to prove aesthetics, phonetics and VDO, expect more wear and occasional fractures, which can be helpful feedback before you move to definitive work.
- Bar supported overdentures: a flexible option in patients with hygiene challenges or when you want easier future maintenance.
From a numbers perspective, a 2023 systematic review of full arch monolithic zirconia prostheses reported an average prosthesis survival of about 97% at a mean follow up of roughly four years, with survival across studies ranging from about 88% to 100%. Monolithic zirconia review. A retrospective series of 214 full arch frameworks found 5 -year prosthesis survival of 88.9% for zirconia and 84.7% for PMMA, but only 60.5% (zirconia) and 78.1% (PMMA) of prostheses remained free from any complications at five years, underscoring the importance of design and maintenance rather than material alone.
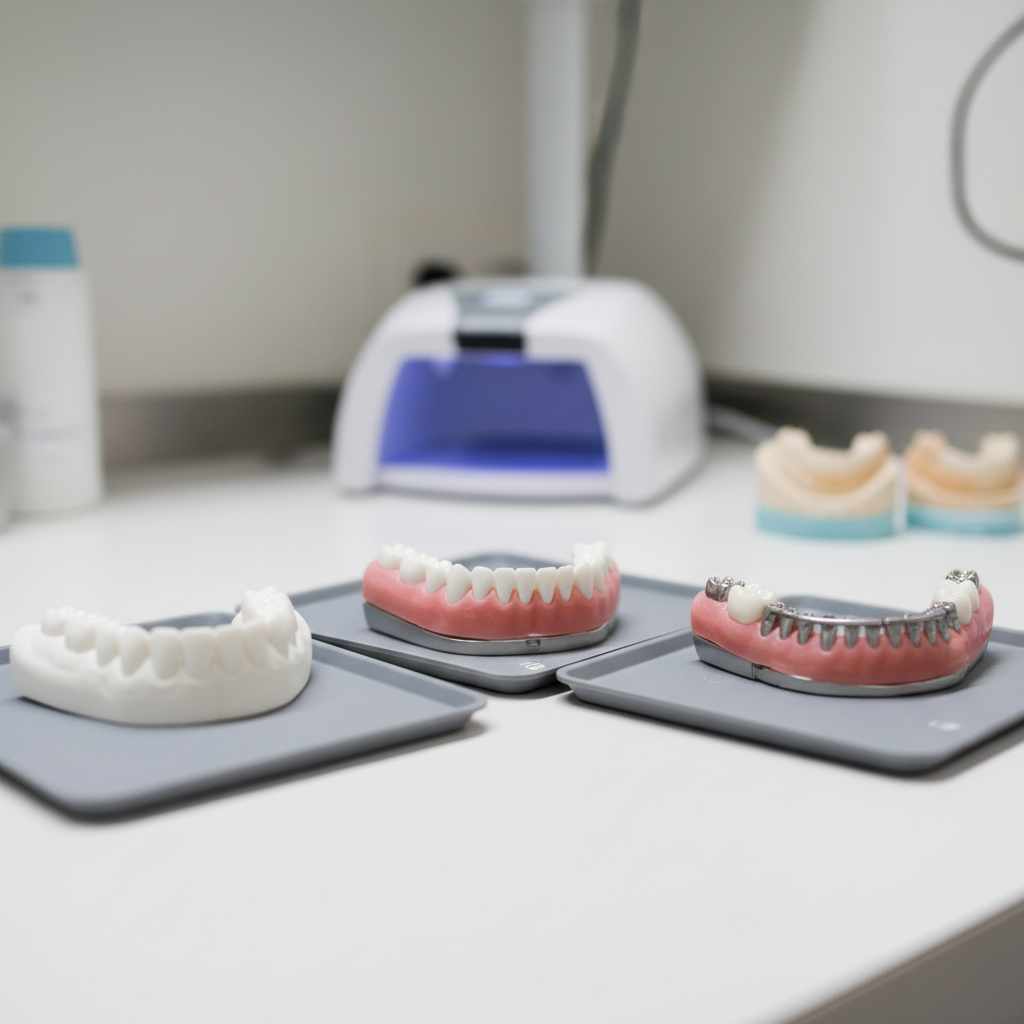
If you are unsure which way to go for a particular arch, you can share photos and scans with the NovaDent team for material suggestions that fit your case goals and your patient’s budget. Our Fixed Prosthetics service page outlines common combinations we support in daily work.
Occlusion, VDO and long term provisionals
Many comprehensive cases fail not because the material fractured, but because the occlusal design never matched the patient’s neuromuscular comfort. That is tough to fix once zirconia is milled.
Staged provisionals let you test:
- The proposed vertical dimension of occlusion over weeks, not minutes
- Centric contacts, excursive guidance and freedom in centric
- Speech sounds (especially “s,” “f,” “v”) and anterior tooth position
- Lip support and smile line in function rather than static photos
For full arch implant cases, cross sectional data show that patients can keep high satisfaction scores even when they do not attend structured maintenance, but prosthetic complications accumulate over time. In one Columbus Bridge Protocol study of 56 patients who did not receive regular peri-implant care, implant survival was 100%, yet the prevalence of prosthetic complications rose from 5.3% at 1 to 2 years to 33.3% after more than six years, while Oral Health Impact Profile scores remained high.
In our lab, we often recommend a period with long term PMMA or printed composite prototypes before converting to monolithic zirconia on the same framework. This “test drive” of the occlusion gives both you and the patient confidence before committing.
Digital workflows that keep adjustments low
When clinician and lab share a consistent digital workflow, complex cases start to feel more routine. For example, a retrospective series of 37 full arch monolithic zirconia restorations fabricated entirely in a digital workflow, with zirconia suprastructures luted to titanium bars, reported 100% prosthesis survival and no serviceable biological or technical complications over 12 to 20 months of follow up.

Practical digital steps that work well in full arch cases include:
- Standardised scan paths and scan body protocols for all your implant systems
- Digital articulation with jaw tracking data where available, or consistent CR records when not
- 3D printed mock ups and try ins derived directly from the approved digital design
- Cloud based case notes and photo sharing so the lab can flag issues early
NovaDent accepts files from all major intraoral scanners and uses CAD/CAM plus AI assisted design for crowns, bridges, dentures and implant restorations, which helps keep remakes and chairside grinding down for our partner practices.
Common pitfalls and how to reduce risk
Most full arch headaches fall into a few predictable themes. Being explicit with your lab from the start keeps them from sneaking into your case.
- Incomplete records: No centric relation, no face photos, unclear smile line. Result: guesswork on incisal edge position and occlusion.
- Unclear endpoint: “Make it look nice” without a defined VDO, occlusal scheme or prosthesis type.
- Insufficient restorative space: Implants placed without a restorative plan, leaving no room for framework and ceramic; leads to bulky or weak designs.
- No provisional phase: Straight from wax up to final prosthesis, leaving no time to test phonetics or comfort.
- Hygiene blind spots: Pontic and tissue designs that are impossible for patients to clean, with predictable peri-implant inflammation later.
Short, honest notes on the lab sheet such as “willing to adjust VDO by ±1 mm based on aesthetics/phonetics” or “prioritise cleansability over pink aesthetics” give the technician permission to make thoughtful suggestions.
Local standards and references such as the ADA dental guidelines can also guide your risk thresholds and maintenance schedules.
For more on how we manage design tolerances and quality control, you can review our services overview.
Working with NovaDent Labs on complex cases
NovaDent Labs was built by a clinician technician team, so our starting point is always the patient in your chair, not just the STL on our screen. From our Sydney lab we support general dentists and specialists across Australia with crowns, bridges, dentures, full arch implant work and specialised appliances, using ISO 13485 and TGA aligned processes.
In complex full arch and full mouth rehabilitation implant cases, we typically:
- Review your records and, where needed, suggest supplementary photos, scans or jaw relation records
- Provide a staged plan (diagnostic wax up or digital set up, provisionals, then definitive work)
- Discuss material combinations that balance strength, aesthetics and cost for that specific patient
- Provide technical case support if you run into questions mid treatment, so you can troubleshoot records, materials or design decisions with the lab team.
If you would like a structured fee guide for these cases, you can use the Request Price List form on our services overview page, or contact us directly through the site. We are happy to review upcoming cases, including severe wear, full arch implant candidates and other complex implant cases, before you present options to your patient.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website