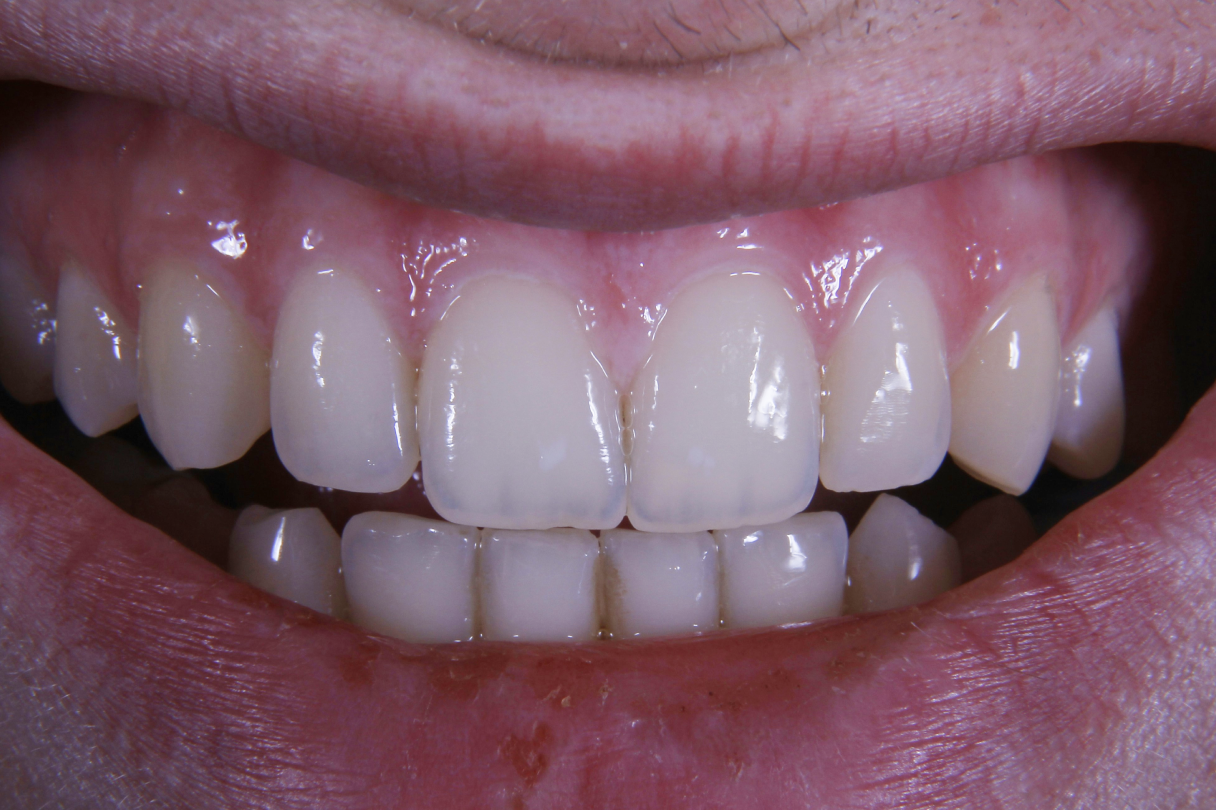
Patients rarely ask for “a B1 shade” they ask for “as white as possible… but I don’t want to wreck my teeth.” So the real question behind how often can you whiten your teeth is: how do we balance bright shade goals with long term enamel health?
As a Sydney based dental lab working with dentists across Australia, we also see the other side of over whitening: dehydrated looking enamel, mismatched crowns, and patients pushing for yet another round of bleach because their social feeds tell them “white equals healthy.” This guide pulls together current evidence and everyday chairside experience to give clinicians a clear way to talk about whitening schedules, especially when gels and trays enter the picture.

Many patients want a brighter smile but worry about how often they can whiten their teeth without harming enamel.
TL;DR
- In chair professional whitening: Usually no more than once every 12–18 months for a full course, with clinical judgement for high stain patients.
- Take home dentist trays (carbamide/hydrogen peroxide):
- Typical course: daily or nightly wear for 7–14 days..
- Repeat full course: commonly every 6–12 months.
- Maintenance: 1–2 nights every 1–3 months, depending on staining habits and sensitivity.
- Over the counter strips and gels: Shorter, lower strength courses; encourage patients to stick strictly to the packet and seek review if they want to repeat.
- Whitening toothpaste: Ongoing use is usually fine when abrasivity is reasonable, but colour shift is modest.
Golden rule: any increase in sensitivity, translucency, or gingival irritation is a signal to pause and reassess, not to push on.
For take home instructions or handouts, you can adapt this summary or point patients towards your practice resources and the NovaDent whitening blogs between visits.
What whitening really does to enamel
Peroxide based whiteners (hydrogen peroxide or carbamide peroxide) don’t “strip away” enamel. Instead, they diffuse through interprismatic spaces, oxidising organic stain molecules in the enamel and superficial dentine.
Explaining how peroxide gels move through enamel and affect stain molecules can reassure patients about whitening safety and limits.
Short term changes in surface hardness, porosity and mineral content have been reported in vitro, especially with higher concentrations and extended contact times. However, saliva and fluoride exposure tend to remineralise the surface once treatment stops, which matches what clinicians see: a transient spike in sensitivity that calms with rest and desensitising care.
Where problems arise is not a single, well managed course. Trouble comes from:
- Stacking multiple full courses close together.
- Doubling wear time “for extra effect.”
- Using high strength products on already compromised enamel or exposed roots.
For that reason, most guidance worldwide stresses dentist assessment first, prescription strength products within professional protocols, and a rest period between whitening cycles.
As a lab partner, we see the downstream effect: patients who push whitening too hard often later require zirconia crowns and bridges to mask intrinsic colour and structural wear that bleaching alone can’t fix.
How often to repeat professional whitening
In chair whitening
In chair systems typically use 25–40% hydrogen peroxide with soft tissue protection, applied in several short cycles within one appointment. The colour change is fast; the question is how often that session should be repeated.
A practical pattern many clinicians follow:
- Full in chair course: once, then review shade stability over 12 months.
- Touch up session: every 12–18 months if relapse and lifestyle warrant it, using the same or slightly gentler protocol.
Heavy tea/coffee/red-wine drinkers and smokers may relapse sooner, but repeating high concentration bleaching several times a year rapidly increases sensitivity risk and patient discomfort, without a proportional shade gain on subsequent rounds.
Combined in chair + take home trays
Many practices now use a “boost plus trays” model: a single in chair session followed by 1–2 weeks of home trays with 10–16% carbamide peroxide or similar. Research on combined whitening protocols
In this scenario, the combined course is still counted as one whitening cycle. Patients can then:
- Use leftover gel for 1 night every 1–3 months as colour maintenance, and
- Return for a full reassessment and possible repeat course roughly every year if indicated.
Whenever a new ceramic restoration is planned, coordinate whitening first, then match crowns, veneers or bridges to the post whitening baseline. Our team at NovaDent routinely uses standard shade systems (e.g. Vita guides) and digital photos to lock in that baseline before implant supported crowns or anterior veneers go into fabrication.
Internal whitening of endodontically treated teeth
Internal bleaching after root canal therapy is a different case: gel is placed in the pulp chamber and refreshed over several visits. Frequency here is dictated by clinical response rather than a fixed calendar, but repeated cycles over many years on the same tooth raise concerns about cervical resorption and structural fatigue. Keeping detailed notes on the number of internal whitening episodes per tooth pays off long term.
How often should you whiten your teeth with gel trays at home?
This is usually where things run off track, because trays feel “gentle” and patients assume more nights equal better whitening.
Typical home gel course

Clear communication about how often to use whitening gel trays at home helps patients avoid overusing “gentle” feeling products.
Most dentist prescribed tray systems use:
- 10–22% carbamide peroxide worn overnight, or
- 6–10% hydrogen peroxide worn for 30–90 minutes daily.
Common protocol for a healthy adult:
- Wear trays once daily (or nightly) for 7–14 consecutive days.
- Stop once the agreed target shade is reached, even if there is gel left over.
- Use a potassium nitrate or stannous fluoride toothpaste for two weeks before and during treatment to calm sensitivity.
How often to repeat a gel course
For most adults with sound enamel and good hygiene:
- Repeat a full 1–2 week course every 6–12 months, not every few weeks.
- Use short “top up” nights (1–2 nights) every 1–3 months only if relapse and lifestyle justify it.
In practice, most healthy adults do best with one whitening cycle every 6–12 months, plus occasional single night top ups, rather than continuous or back to back bleaching.
Any of these should trigger a pause and review before repeating:
- Sensitivity lingering more than 48 hours after a whitening night.
- Sharp zingers on chewing or with cold air.
- Patchy, chalky areas or increased incisal translucency.
- Red, puffy or tender gingiva along tray margins.
Coaching patients on non prescription gels
Patients will use online kits regardless of what we say. Rather than a flat “no,” give simple rules of thumb:
- Stick exactly to the product’s stated number of days.
- Space out repeat courses by at least several months.
- Book an exam before starting again if they have any sensitivity history, restorations on anterior teeth, or past trauma.
Healthdirect Australia and other public health sites echo the same message: whitening should run under dental supervision, with practitioner supplied products preferred over unregulated kits.
If your practice offers customised take home kits through a partner lab, you can link this advice directly to a structured protocol and shade documentation, rather than leaving patients to self experiment.
Signs whitening is happening too often
A handy way to frame things chairside is, “Your teeth will usually tell us when they’ve had enough.” Red flags include:
- Sensitivity trending upward across a course instead of stabilising.
- Grey or glassy edges on incisors as enamel thins and dehydration effects linger.
- Gingival blanching or ulceration at tray margins.
- Uneven, patchy shade suggesting irregular demineralisation, not simple stain removal.
Certain patients need especially gentle scheduling or alternative strategies:
- Young adults and adolescents with larger pulps and thinner enamel.
- Teeth with cervical abrasion, erosion or recession.
- Heavily restored anterior teeth, craze lines, or existing white spot lesions.
- History of significant post whitening hypersensitivity.
For these cases, discussing restorative or orthodontic options early from microabrasion and resin infiltration to veneers or aligners often leads to happier, safer outcomes than chasing repeated bleach cycles. When you reach that point, a close relationship with your prosthetic and orthodontic lab partners makes planning much smoother.
Whitening, restorations and what labs see
From the lab bench, one pattern stands out: patients often whiten after they have anterior crowns, composite veneers or implant crowns in place. As you know, those restorations do not change colour with bleach.

Reviewing tooth shades together before crowns, veneers or implant restorations ensures whitening cycles and prosthetics stay aligned.
The result is a patchwork smile: natural teeth step up several shades, while older prosthetics stay put. Repeated whitening at that point only widens the mismatch and may increase sensitivity, without ever solving the aesthetic complaint.
A more predictable sequence is:
- Full exam, photographs and shade documentation.
- Whitening (in chair, trays, or both) with a planned end shade.
- Shade re-check two weeks after whitening stops, once rebound settles.
- Only then, finalise shade selection for crowns, veneers or implant prosthetics.
At NovaDent, we encourage our partner clinics to send post whitening photos and shade references with their lab prescriptions via our secure case submission form. That single step cuts down remakes and patient dissatisfaction when whitening and restorative work intersect.
Chairside scripts for talking about whitening frequency
When patients push for “just one more round,” having simple language helps. A few examples you can adapt:
- On spacing treatments:
“Your enamel needs rest between whitening courses, a bit like skin between peels. Let’s review in a year rather than stacking another full round now.” - On gel tray overuse:
“More nights won’t give a Hollywood jump in shade, but they will raise your chance of sensitivity. Let’s keep this course for two weeks, then reassess.” - On expectations with existing crowns:
“Whitening only changes natural teeth. If we push the bleach again, your crowns will still stay the same colour. To get everything matching, we may need to plan new ceramics instead.” - On DIY kits:
“If you’d like to brighten safely at home, I’d rather prescribe a gel where we know the exact strength and timing, and we’ll check on your enamel and gums as we go.”
Having a printed or digital handout that echoes this advice can reduce post-op calls and gives patients something to share with family members asking the same questions. Many practices place these guides alongside clinical content about implants, dentures and crowns so patients understand whitening as one part of a bigger treatment picture.
Plan whitening and restorative cases together
For Sydney and Australian dentists planning whitening-led cosmetic or implant cases, you can work with NovaDent Labs as your digital lab partner or submit a case online so whitening, shade selection and final restorations stay aligned.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website