TL;DR
- Think of full arch implants cases as prosthetic cases first: work backwards from the ideal prosthesis and involve your lab early.
- Consistent records (CBCT, photos, digital scans, jaw relation) give you fewer surprises and fewer fit appointments.
- Design choices around material, framework, access for hygiene and phonetics matter as much as implant number and brand.
- Full arch dental implants cost is shaped by surgical complexity, prosthetic design, temporisation strategy and lab workflow not just your lab fee.
- A digital, CAD/CAM based lab partner can help you standardise your protocol and make full arch cases feel repeatable rather than “one off” projects.
For many Australian dentists, full arch implants are both exciting and slightly daunting. You know how transformative a stable, fixed prosthesis can be for an edentulous patient, yet every case comes with a stack of decisions: implant number and position, immediate load or delay, prosthetic design, materials, and of course, fees that patients can realistically manage.
At the same time, your lab partner needs clean digital records, clear instructions and a shared plan so you are not troubleshooting fractures or phonetics at the fit appointment. This article sets out a practical framework you can use to plan, present and deliver predictable full arch restorations while keeping your chair time and patients’ expectations under control.
What are full arch implants?
In simple terms, full arch dental implants support a fixed prosthesis that replaces all teeth in a maxillary or mandibular arch. Rather than one implant per tooth, a smaller number of implants (often four to six) support a screw retained bridge that restores function, aesthetics and confidence for completely edentulous or soon to be edentulous patients.
Clinically, you might be thinking in “All on 4 style” protocols, tilted posterior implants, or more traditional parallel placement with six fixtures. Prosthetically, however, the key question is: What kind of full arch bridge will this patient clean and live with every day? That is where close collaboration with your implant laboratory matters.
If you routinely provide implant restorations through NovaDent Labs, full arch cases build on the same principles: stable occlusion, repeatable jaw position, and a design that respects soft tissue and bone. For patient friendly education material on implants generally, you may also want to point patients to resources from bodies such as the Australian Dental Association.
When is a full arch implant restoration indicated?
Typical candidates include patients with terminal dentition from advanced periodontitis, repeated restorative failure, or severe wear, as well as long term denture wearers who cannot tolerate further loss of retention or soft tissue soreness.
Red flags should feel familiar: poorly controlled systemic disease, heavy smoking, parafunction that cannot be managed, limited mouth opening, or patients whose expectations are well beyond what any prosthesis can deliver. These are moments where slowing down, gathering more data and planning with your lab pays off.
A structured case selection checklist, shared between the surgery and lab, keeps you consistent. Many clinicians set up a simple internal pathway: initial diagnosis and photos, followed by a dedicated consult where they review CBCT findings and a basic full arch plan with their preferred lab. If you do not yet have a template, our team can help you develop one through our case planning support.
Clinical and lab workflow for full arch dental implants
Every clinician has a slightly different style, but predictable cases tend to share the same backbone. From the lab side, these are the stages that make or break the outcome.
Treatment planning and records
High quality records are the foundation. At minimum, your lab will work best with:
- CBCT of the relevant arch (with opposing dentition visible where possible)
- Intraoral scans or well bordered conventional impressions of both arches
- Full face and intraoral photographs in repose, smile and profile
- A stable jaw relation record and agreed vertical dimension

When these arrive together, your technician can build a digital wax up, propose implant positions and advise on whether a fixed hybrid, monolithic zirconia or other design is realistic. A standardised checklist, such as the ones we use in our digital workflows, helps your team collect the same set of data every time.
Surgical phase working with your lab
Some clinicians still place freehand; others prefer fully guided systems. Either way, aligning implant positions with the planned prosthesis is what keeps you out of trouble with screw access, lip support and cleansability.
Many of our referring dentists ask for:
- A diagnostic wax up and printed try in
- Surgical guides based on that set up
- A clear plan for multi unit abutment selection on the day
A quick call or video case conference with the lab before surgery can flag issues like limited prosthetic space or compromised bone that might otherwise only become obvious at the impression stage.
Provisionalisation and immediate load
Where primary stability and patient factors permit, immediate loading with a screw retained provisional can be life changing for patients. The key is to keep the temporary prosthesis forgiving: generous cleansable contours, lighter occlusal contacts and simple repair options.
Digital design and milled PMMA provisionals give you strength with easy adjustability. Your lab can often deliver a same day or next day provisional if the workflow is planned ahead. For more traditional protocols, a well fitting complete denture converted to an implant retained provisional on the day still works reliably when the lab has prepared the components in advance.
Definitive full arch prosthesis design
Once tissues stabilize and you are happy with the occlusal scheme, records for the definitive prosthesis should be as precise as you can comfortably obtain: open tray impressions or accurate scans, validated jaw relation, and a provisional that has been “road tested” by the patient.
At this stage, the lab will guide you on framework design, material selection and whether to preserve or reduce pink aesthetics. A short, structured lab prescription that documents what did and did not work in the provisional helps convert a good temporary into a great final bridge.
Design choices that matter to patients
From a patient’s perspective, “teeth that don’t come out” sounds simple. In practice, design details determine whether that promise feels true six months later.
Screw retained vs cement retained
Most full arch prostheses are screw retained for retrievability and maintenance. Where implant angulation demands, angled screw channel components give you aesthetic access without compromising serviceability.
Cement retained options may still have a place in segmental restorations, but for full arches the risk of residual cement and the difficulty of retrieval mean screw retained designs are usually preferred. Discuss this early with your technician so they can optimize framework design and soft tissue contours around the access channels.
Material options for full arch frameworks
Common combinations include:
- Titanium or cobalt chrome framework with acrylic or composite teeth
- Monolithic or layered zirconia full arch bridges
- Hybrid designs with a milled bar and individually bonded crowns
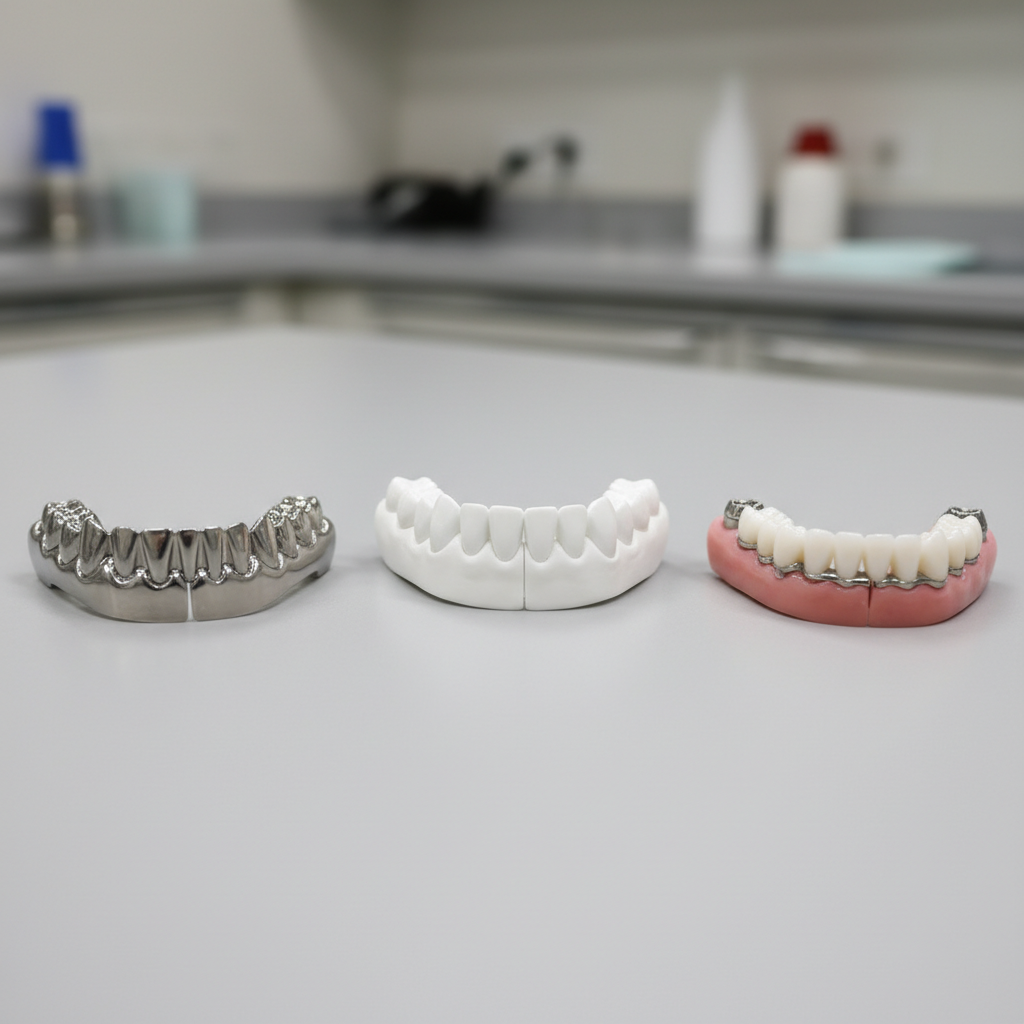
Different full arch implant materials and framework designs carry distinct trade offs in strength, aesthetics and maintenance.
Each approach has trade offs in weight, wear behaviour, aesthetics, repairability and cost. Discussing options with your lab and showing patients clear photos or demos often shortens consent discussions. For clinicians wanting a deeper review of materials and wear, organisations such as the American Academy of Periodontology publish useful summaries and consensus reports.
Occlusion, phonetics and hygiene
These are the classic “everything looked fine on the model” issues. A small anterior cantilever, palatal bulk or phonetic edge can undo a beautiful case if it interferes with speech or cleaning.
Many dentists now schedule a dedicated phonetic and hygiene review with the provisional, then document feedback for the lab. Simple notes such as “slightly more tongue space palatally around 11 to 21” or “patient struggles with floss under 33 to 43 area” give the technician clear directions for refinement.
In full arch work, the lab is not a vendor at the end of the chain; it is a planning partner from day one.
Full arch dental implants cost: what actually drives the fee?
Patients quickly ask about numbers, but as you know, full arch dental implants cost in Australia is not one fixed figure. It reflects the surgical plan, materials, number of visits and how efficiently the team works together.
Surgical factors
- Number and brand of implants, and the need for bone grafting or sinus lifts
- Use of guides, immediate placement in extraction sockets, or staged approaches
- Anaesthesia arrangements and theatre or day surgery fees where relevant
Prosthetic and laboratory factors
- Type of definitive prosthesis (hybrid acrylic, zirconia, segmented bridges)
- Number of provisional stages and whether you are changing vertical dimension
- Framework design complexity and any special components or multi unit abutments
As a lab, we see that clinicians who present “good, better, best” options with clear explanations of trade offs tend to have smoother consent conversations. We can help you structure these with sample cases and photos from our implant resources library.
Digital vs traditional workflows
Digital workflows usually front load some planning costs but can reduce the total number of appointments, remakes and chairside adjustments. Over a year of cases, that can have a very real impact on how sustainable your full arch offering feels for the practice.
When you request our NovaDent Labs price list, we can outline how different material and workflow choices influence the lab component of your fee, so you can build transparent packages for your patients.
Digital workflows for predictable full arch cases
If your practice already uses an intraoral scanner, full arch cases are a natural extension of the digital work you do for crowns and bridges. The difference is in how thoroughly the data is combined and shared.
A typical digital pathway might include:
- CBCT and intraoral scan alignment for prosthetically driven implant planning
- Digital wax up and 3D printed try in for patient approval
- CAD/CAM milled provisional and final prostheses with documented design files
Digital scanning and CAD/CAM workflows help standardise full arch implants from planning through to final restoration.
This gives you an audit trail and makes remakes, repairs or future upgrades far less stressful. Our team has set up many clinicians with simple protocols to send scanner files, photos and prescriptions through secure channels, outlined in our guide to digital workflows. For broader reading on digital implant dentistry, the open access library at NCBI’s PMC hosts a number of useful review papers.
Working with NovaDent Labs on full arch cases
NovaDent Labs was built by clinicians and technicians who handle full arch work every week, not once a year. That shapes how we support you: from recommending suitable components for the major implant systems used in Australia, to reality checking whether a proposed design will be maintainable for a particular patient.
We typically help with:
- Case planning support and review of CBCT and diagnostic records
- Diagnostic set ups, guides and provisionals for All on 4 style protocols
- Framework design and material selection matched to your patient’s risk profile
- Clear communication about turnaround times and logistics Australia wide
If you are new to full arch work, starting with a small number of well planned cases and a lab that treats you as a partner makes a big difference. You can learn more about how we work with practices in our About NovaDent Labs section.
FAQs
How many implants do I need for a full arch?
Most patients need between four and six implants per arch, but the exact number depends on bone quality, anatomy, bite forces and the type of prosthesis planned. The final decision comes after a full clinical exam and CBCT based assessment.
How long do full arch implant bridges last?
With good home care, regular professional maintenance and well planned occlusion, many patients enjoy stable function for many years. Over time, however, wear, chipping or changes in soft tissue may mean repairs, relines or replacement of the prosthesis. You can frame this as ongoing maintenance, much like servicing a car, rather than a “once and done” solution.
Why do full arch options cost more than dentures?
Patients see the surgical phase and final smile, but much of the fee reflects planning, high precision components, lab work and multiple visits. Explaining that they are paying for stability, function and day to day comfort not just “more expensive teeth” often makes the discussion feel fairer.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website




