This guide is for general information only and does not replace a dentist’s clinical judgement or a medical emergency assessment.
Throbbing toothache that keeps you awake, sudden swelling in the jaw, a bad taste that won’t go away are the sorts of problems that make people call a dentist first thing in the morning. Often, the underlying cause is a tooth abscess, an infection around a tooth that can spread quickly if it isn’t treated.
For patients, it feels frightening and disruptive. For clinicians, it can mean a long day of emergency appointments, difficult conversations, and urgent decisions about saving or extracting teeth. This article explains what’s happening inside the tooth, the stages of infection, the red flag symptoms, and how prompt treatment and thoughtful restorative planning protect long-term oral health.
TL;DR
- A tooth abscess is a pocket of pus caused by a bacterial infection in or around a tooth.
- Typical tooth abscess symptoms include severe toothache, swelling, tenderness on biting, and sometimes fever or feeling unwell.
- Stages move from deep decay and pulpitis through to localised abscess, then potentially to spreading infection that can affect the face, neck and airway.
- Tooth abscess treatment usually involves drainage of infection plus either root canal treatment or extraction, followed by definitive restoration.
- Patients should seek urgent dental care; clinicians can then work with a lab such as NovaDent Labs to restore function and aesthetics once infection is controlled.
What is a tooth abscess?
A dental or tooth abscess is a collection of pus caused by bacteria, usually triggered by untreated decay, a cracked tooth, or advanced periodontal disease. The infection can occur:
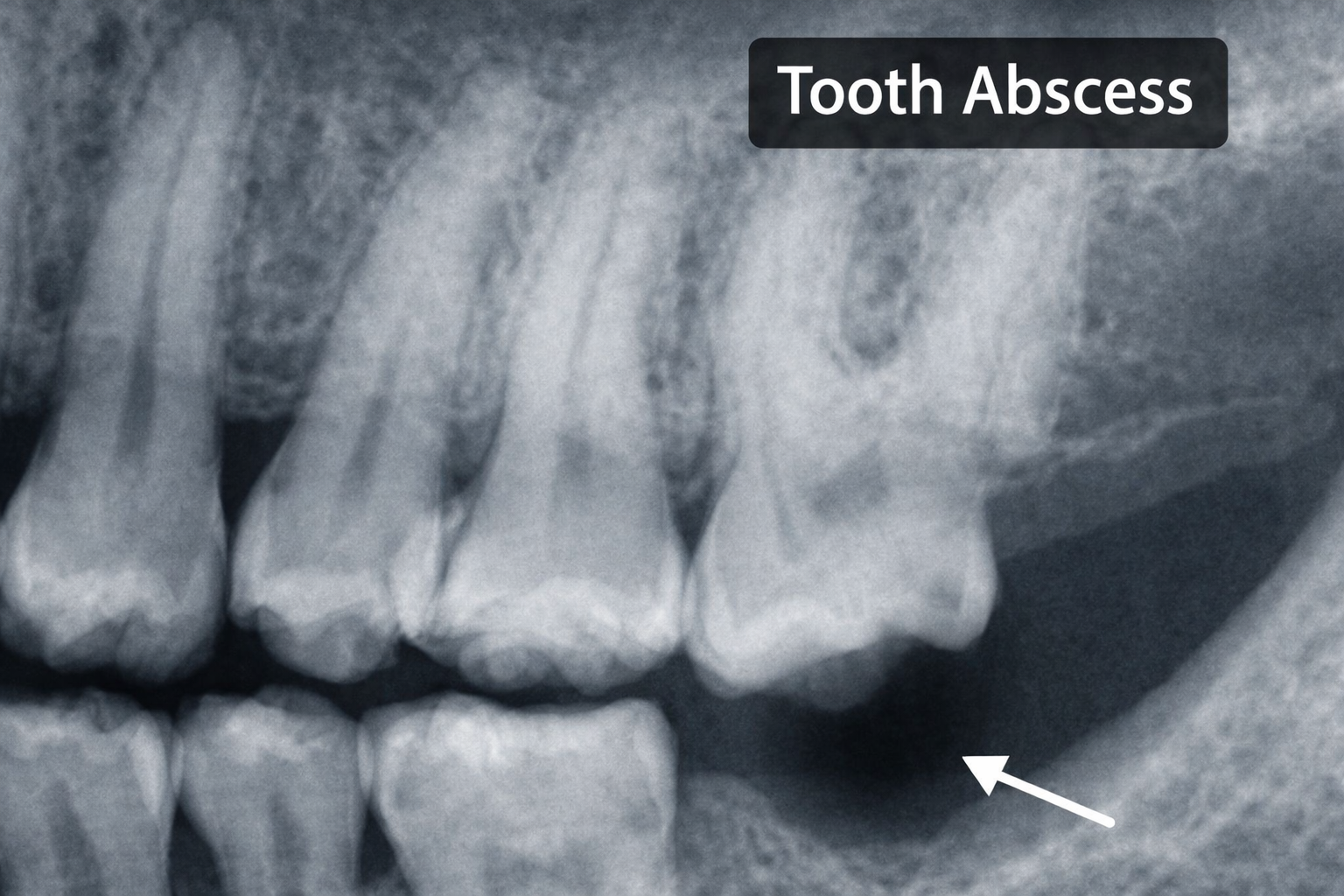
- Periapically – at the tip of the root after the pulp has become necrotic.
- Periodontally – along the side of the root, linked to deep periodontal pockets.
Either way, bacteria enter spaces they should never reach. The body responds with inflammation, fluid and pus, which build up pressure inside bone and soft tissue. That pressure is what creates the intense, throbbing pain many patients describe.
Reliable clinical overviews are available from organisations such as the NHS and Cleveland Clinic, which both explain symptoms, treatment and potential complications of an untreated dental abscess.
Tooth abscess symptoms: what patients notice
In practice, patients rarely present saying “I think I have a periapical abscess.” They describe experiences such as:
- Severe, throbbing toothache that may radiate to jaw, ear or neck.
- Pain that worsens when lying down, chewing, or tapping the tooth.
- Swelling of the gum, face or jaw near the affected tooth.
- Red, tender gum or a “pimple” on the gum that may discharge pus.
- Bad taste or odour in the mouth.
- Sensitivity to hot or cold is sometimes followed by loss of sensation as the pulp dies.
- Fever, malaise or enlarged lymph nodes in more advanced cases.
Clinicians will of course confirm the diagnosis with history, clinical exam, and radiographs. For patient education material in your practice, many dentists link to resources from the Australian Dental Association.
The 4 Stage Tooth Abscess Progression
The phrase tooth abscess stages usually refers to how far the infection has progressed. While every case is slightly different, you can think about this 4 stage tooth abscess progression in four broad stages.
Stage 1 – Deep decay and inflamed pulp
Decay progresses through enamel into dentine, allowing bacteria and toxins to approach the pulp. The pulp becomes inflamed (reversible or irreversible pulpitis), often causing sensitivity and sharp pain, especially to hot or cold.
Stage 2 – Pulp death and early spread
Left untreated, the pulp tissue breaks down and dies. Bacteria now occupy the root canal system. Pressure builds within the tooth, then moves through the apical foramen into the surrounding bone, leading to apical periodontitis.
Stage 3 – Localised tooth abscess
A true abscess forms as pus collects in bone or soft tissue. Pain is usually constant and severe. Swelling may be visible intraorally or extraorally. A sinus tract may develop, giving temporary relief when it drains.
Stage 4 – Spreading infection and systemic involvement
In advanced cases, infection extends into fascial spaces of the face and neck. Patients can develop trismus, difficulty swallowing, or breathing compromise. Systemic signs like high fever, tachycardia and general illness may be present.
At this stage, hospital management, IV antibiotics and surgical drainage may be required. Communication between the treating dentist, medical team and, eventually, the restorative dentist and lab becomes essential as long-term treatment planning begins.
Tooth abscess treatment options
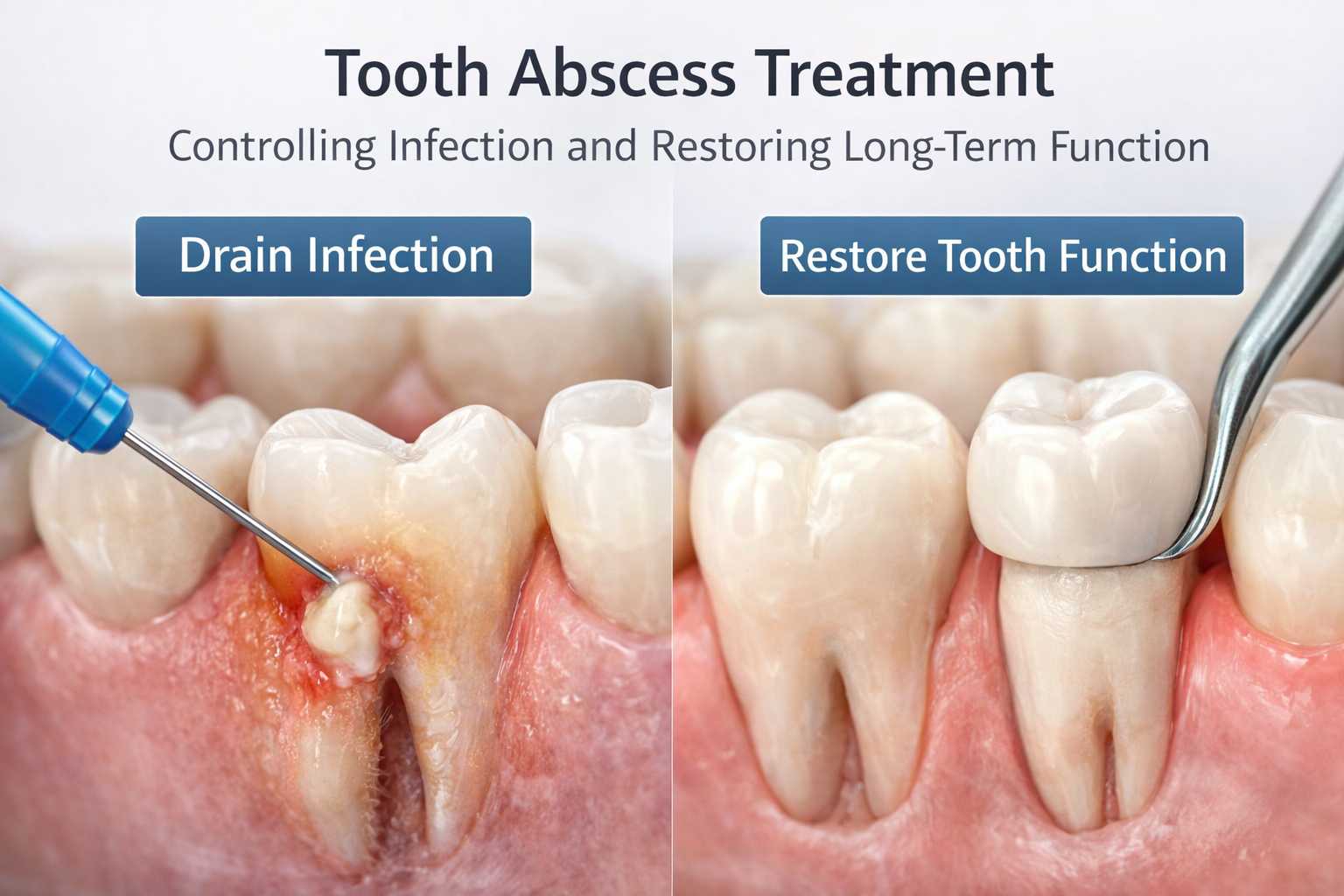
Once an abscess is confirmed, treatment goals are consistent: control infection, relieve pain, remove the source of infection, and restore function and aesthetics.
For patients: what usually happens at the dentist
Patients often ask, “What will you do today?” While each case is individual, the dentist will generally:
- Assess symptoms, medical history and vital signs to check for signs of spreading infection.
- Take appropriate radiographs to locate the source and extent of the problem.
- Provide local anaesthesia and, if needed, initial drainage either via the tooth (access cavity) or soft tissue incision.
- Prescribe antibiotics when indicated for example, if there is cellulitis, systemic involvement, or difficulty achieving drainage at that visit.
- Explain options: root canal treatment, extraction, or, in rare cases, a period of monitoring when the diagnosis is uncertain.
Only a dental professional who has examined the tooth can decide on the right course of action. Over the counter pain relief may help symptoms for a short time, but it does not resolve the underlying infection.
Guidelines from the American Dental Association highlight that, for most otherwise healthy adults with localised acute apical abscess and no systemic signs, priority should be given to procedures such as drainage or root canal treatment rather than relying on antibiotics alone.
For dentists: from drainage to definitive restoration
For clinicians, successful tooth abscess treatment is more than pain relief. It sets the stage for durable restoration:
- Root canal treatment (RCT): Cleaning, shaping and obturation of the root canal, followed by a well sealed core and coronal coverage, often with a full crown. Many dentists work with their preferred lab for post and core and crown fabrication; for example, NovaDent’s fixed prosthetics (crowns and bridges) are designed to support predictable outcomes after endodontics.
- Extraction: When prognosis is poor, extraction may be the safest option. Provisional replacement (flipper, temporary partial denture) can be followed by a fixed bridge, implant supported crown, or removable prosthesis. Labs play a major role at this stage.
- Adjunctive care: Occlusal adjustment, treatment of contributing periodontal disease, and patient education about oral hygiene and diet complete the picture.
Working backwards from the desired restorative endpoint often makes decision making easier. If you know a heavily compromised molar is unlikely to support a long term crown, planning extraction plus implant or bridge with your lab early can streamline the whole pathway.
When is a tooth abscess an emergency?
Some situations call for same day or hospital-based care. Red flags include:
- Swelling that spreads rapidly or affects the eye, cheek, floor of mouth or neck.
- Difficulty swallowing, talking, or breathing.
- High fever, chills, confusion or feeling very unwell.
- Trismus or inability to open the mouth properly.
- Patients with compromised immunity (e.g. diabetes, cancer therapy) showing any signs of spreading infection.
Resources such as the NHS and Cleveland Clinic stress that dental abscesses causing rapid facial swelling, high fever or breathing and swallowing difficulty need urgent assessment, because infection can spread into deep spaces of the head and neck or, rarely, cause life threatening complications.
Case example (anonymised): A middle aged patient delayed seeing a dentist for a “gum boil” that stopped hurting once it started draining. Within 48 hours of new swelling under the tongue and in the neck, they required hospital admission for IV antibiotics and airway monitoring, a pathway that earlier dental treatment might have prevented.
In these cases, emergency services or a hospital emergency department may be the safest first stop. Having clear practice protocols, triage scripts for reception staff, and a checklist for when to escalate can reduce stress for both teams and patients.
How dental labs support long term outcomes
At first glance, tooth infections look like a purely clinical issue. Yet many abscess cases end with restorative work where the lab’s input shapes the final result.
Examples where a lab such as NovaDent is involved include:
- Post endodontic crowns: Well-designed full coverage after RCT reduces the risk of fracture and microleakage. Accurate occlusal schemes and contact points minimise postop symptoms.
- Bridges after extraction: When a tooth cannot be saved, a bridge may be planned. Quality frameworks and ceramics influence both longevity and patient satisfaction. See our overview of fixed prosthetics (crowns and bridges).
- Implant restorations: Once the site has healed and an implant is placed, a lab experienced in digital workflows and implant systems can help deliver a precise, aesthetic crown. Learn how we approach this on our implant restorations page.
- Removable options: For some patients, partial dentures remain the best solution. A digitally planned design from a lab that understands occlusion and clasping can make daily wear far more comfortable. More details are available under NovaDent removable prosthetics and dentures.
When dentists share clear notes, photos and scans related to the original abscess case, the lab can factor in history of infection, periodontal status and occlusal challenges while designing the restoration.
FAQs
Can a tooth abscess heal on its own?
The body may temporarily wall off infection or form a draining sinus, which can lessen pain. However, the source of infection often remains. Without professional treatment, flare ups and progression are very likely.
Can antibiotics alone treat a tooth abscess?
Antibiotics can help control spreading infection and systemic signs, but they do not remove necrotic pulp or deeply infected tissue. Definitive treatment root canal treatment or extraction is still needed in most cases.
How long can you leave a tooth abscess untreated?
There is no safe “time limit.” Some patients deteriorate quickly. Others have low grade symptoms for months, but the risk of sudden worsening remains. As a rule of thumb, any suspected abscess should be assessed by a dentist as soon as possible.
Does a tooth abscess always hurt?
Not always. Once the pulp is fully necrotic and a sinus tract forms, pain can lessen or even disappear. Radiographic changes and sinus tracts often reveal chronic abscesses during routine exams, which is another reason regular check ups matter.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website