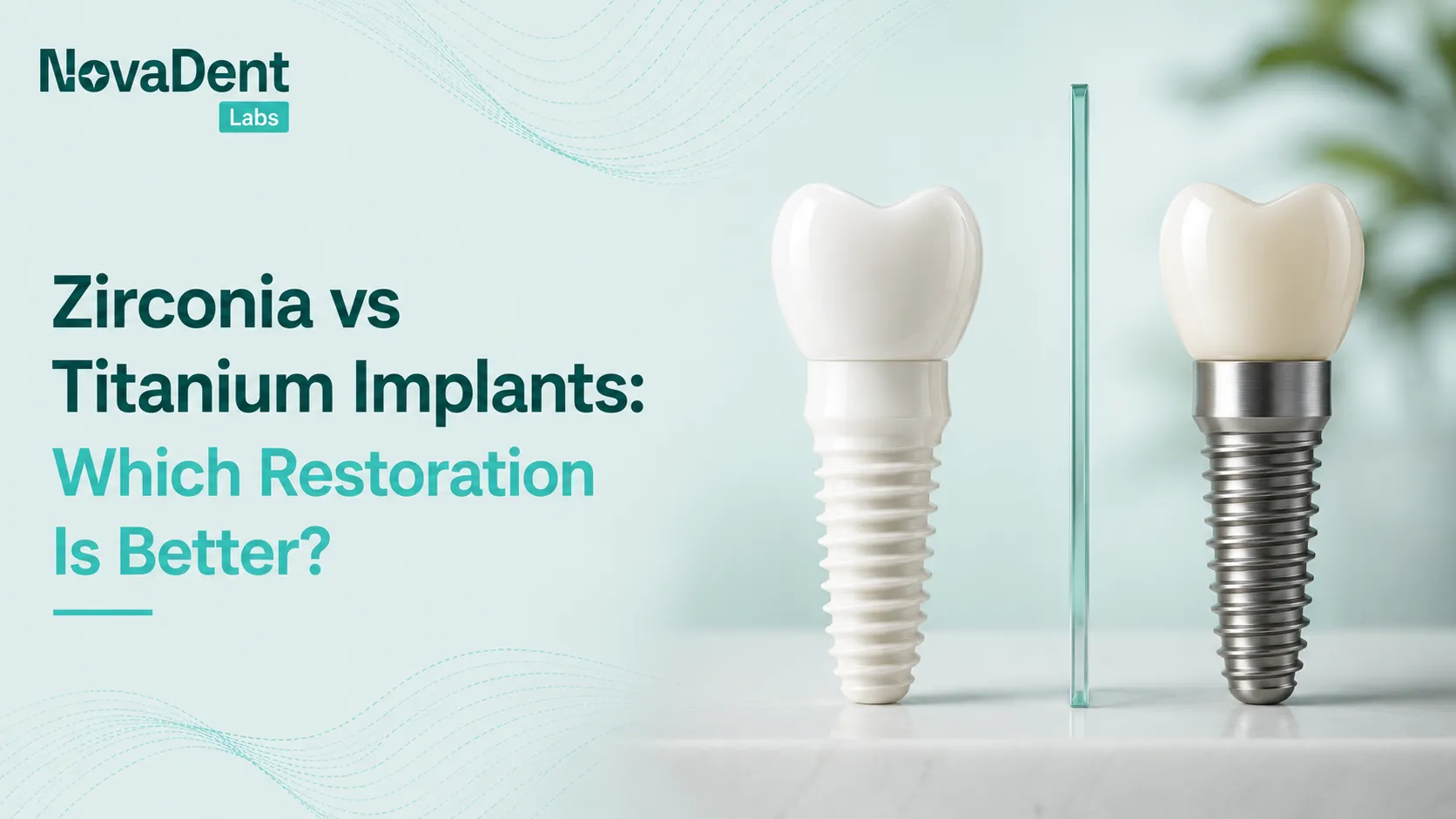
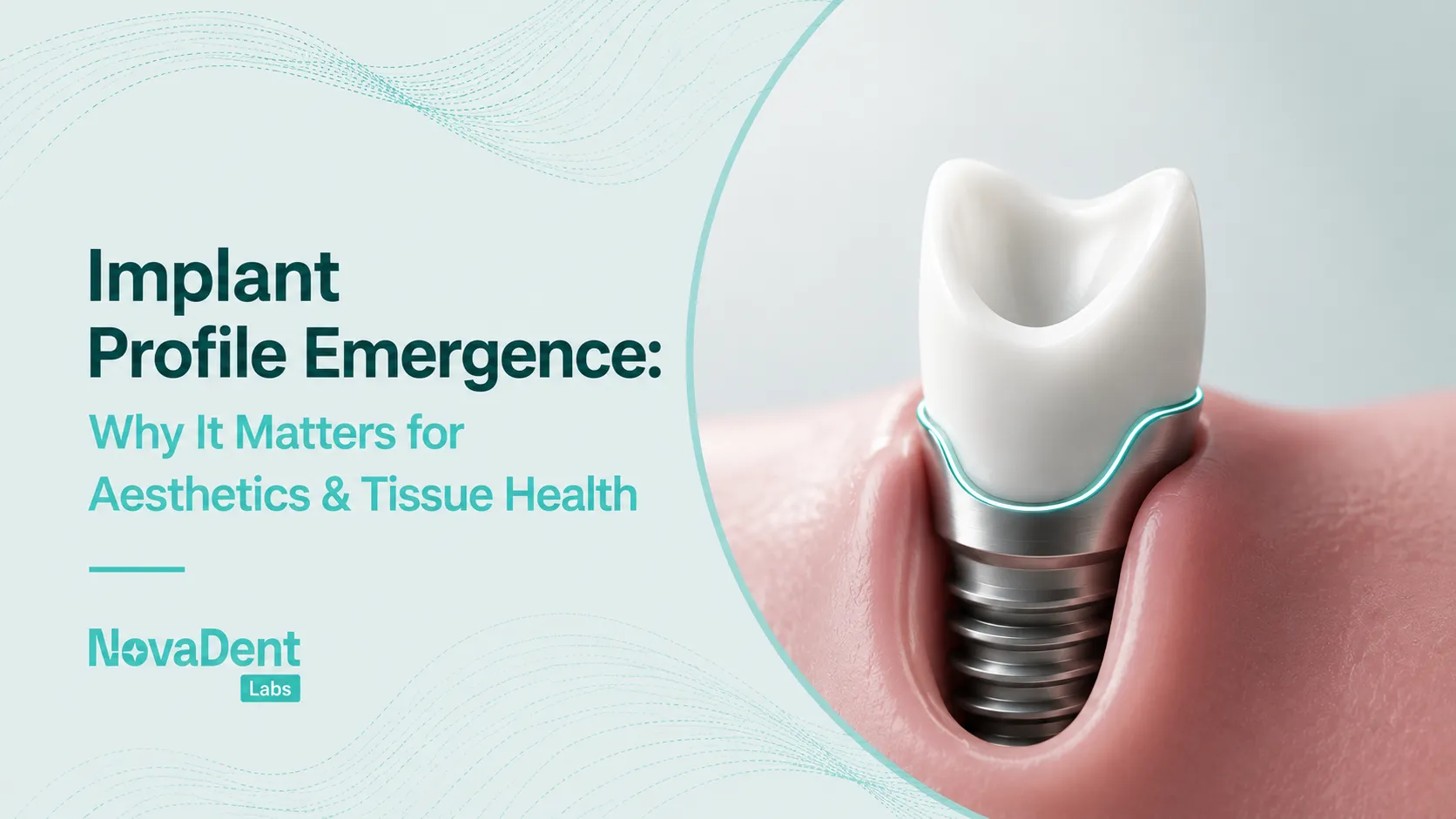
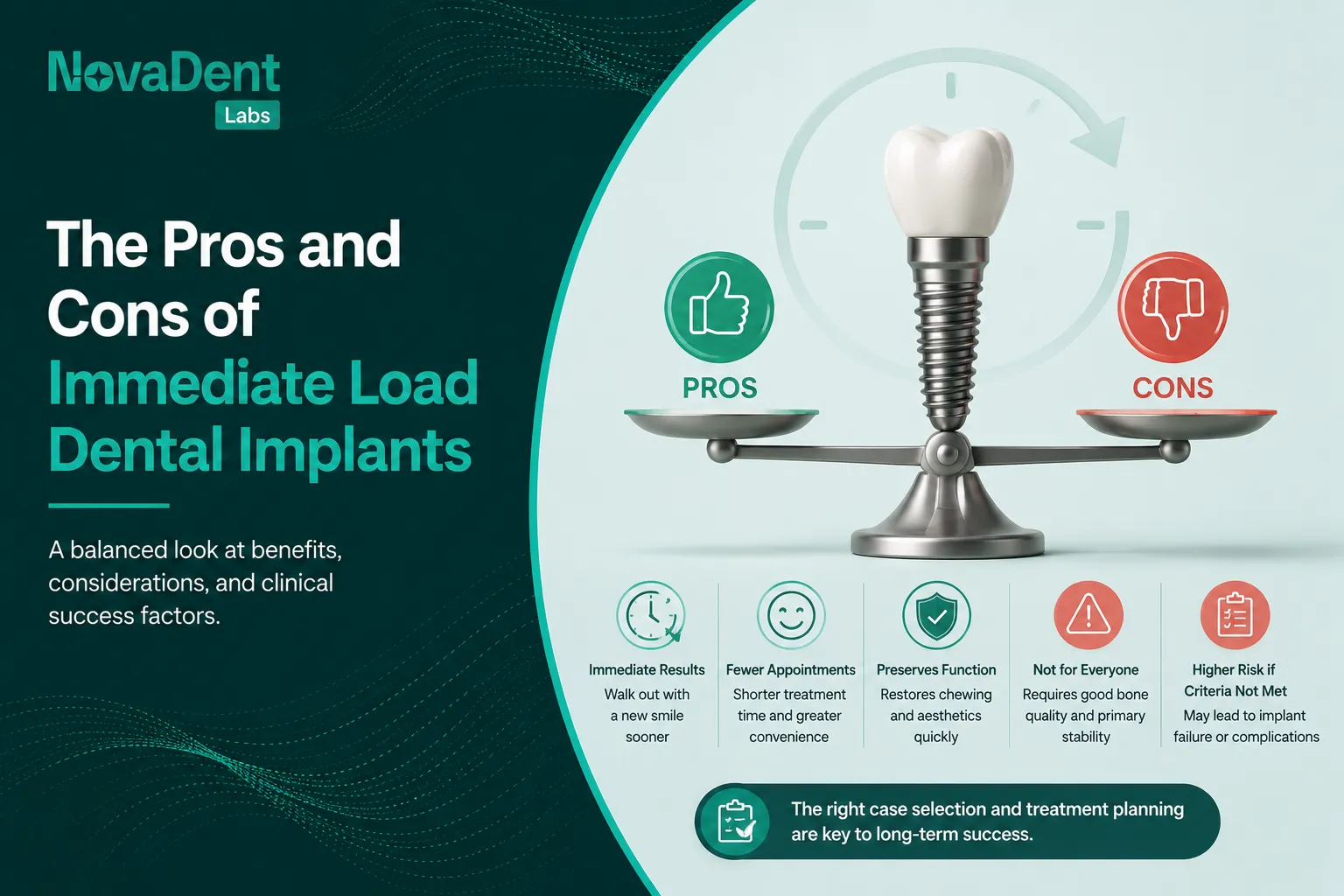
When patients ask, “what are dental implants made of,” they’re really asking two things: what’s going into my body, and how reliable is it long term and as clinicians we also need to understand how implant materials and components influence biomechanics, soft tissue health, aesthetics, and our restorative options chairside.
This guide for general dentists and specialists summarises the core materials used in modern implant systems and the main hardware pieces you work with every day.
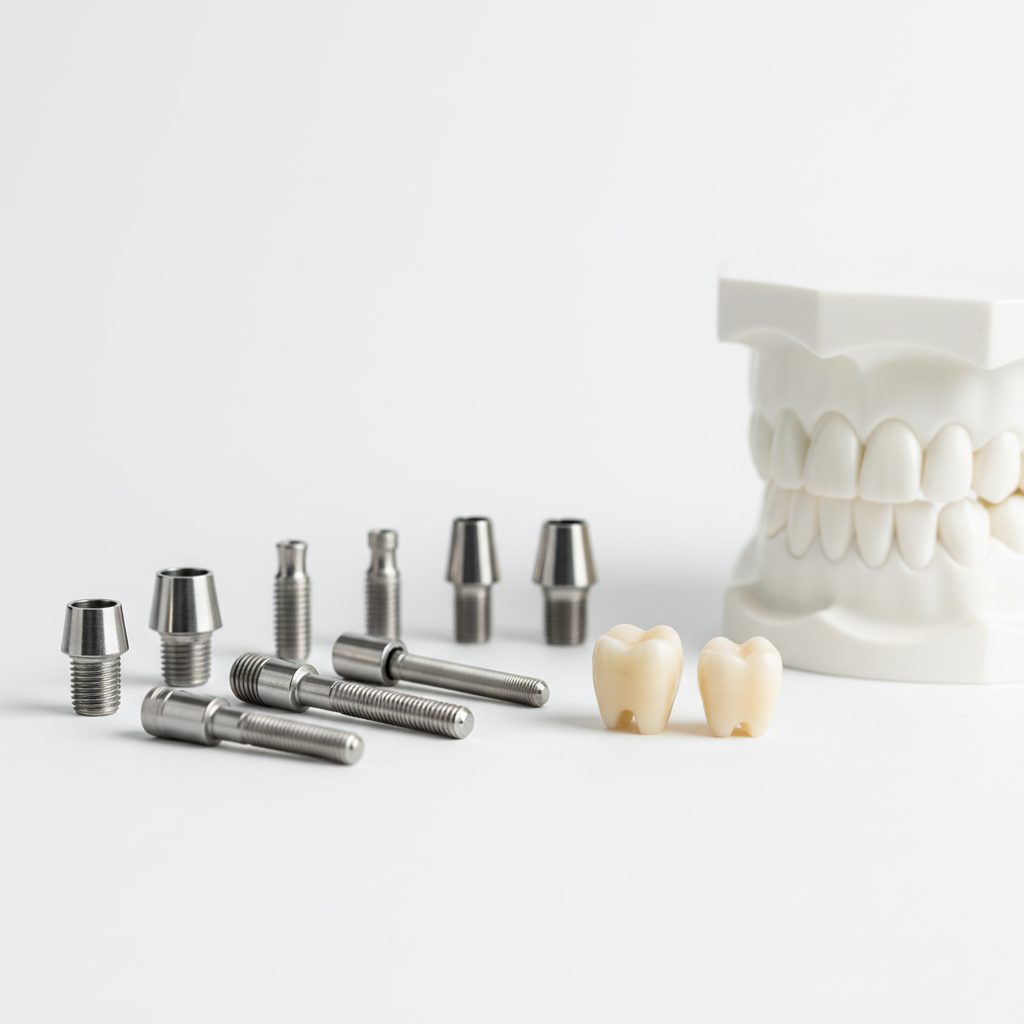
Core dental implant components: fixtures, abutments, and crowns in a clean clinical setup.
TL;DR:
- Fixtures: Most implant bodies are titanium or titanium alloy; zirconia is a metal free alternative for selected indications.
- Abutments: Stock or custom, in titanium or zirconia, connecting the fixture to the prosthesis.
- Prosthetics: Single crowns, bridges, or full arch solutions, often CAD/CAM milled from zirconia, lithium disilicate, or metal ceramic (see our implant restorations).
- Small parts: Prosthetic screws, healing abutments, scan bodies, and overdenture attachments complete the system.
For patients: Dental implants are usually made from titanium or tooth coloured zirconia. A small screw (fixture) goes in the bone, a connector (abutment) sits on top, and a crown, bridge, or denture is attached above the gum line. These materials are chosen because they are strong, biocompatible, and long lasting.
1. Overview: how an implant system fits together
An endosseous implant system has three layers:
- Implant body / fixture – the screw shaped part in the bone, replacing the root.
- Abutment – the connector emerging through the soft tissue.
- Prosthesis – crown, bridge, or full arch restoration that takes the load.
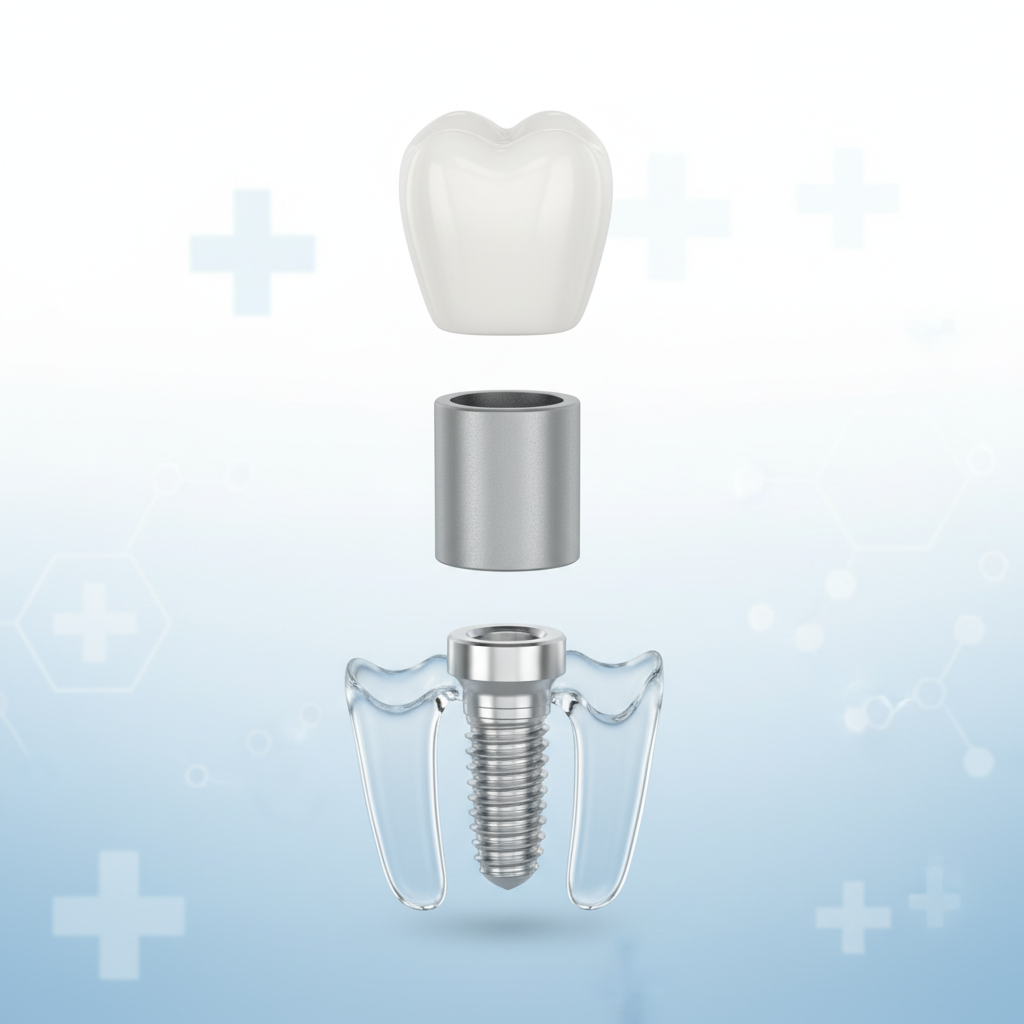
The three main layers of a dental implant system: fixture, abutment, and prosthetic crown.
Around that trio sit healing abutments, cover screws, multi-unit abutments for full arch work, impression or scan bodies, and overdenture attachments; knowing which components and materials are in play makes lab communication smoother and reduces last-minute compromises during implant planning.
Typical materials by implant component
2. Core materials used in dental implants
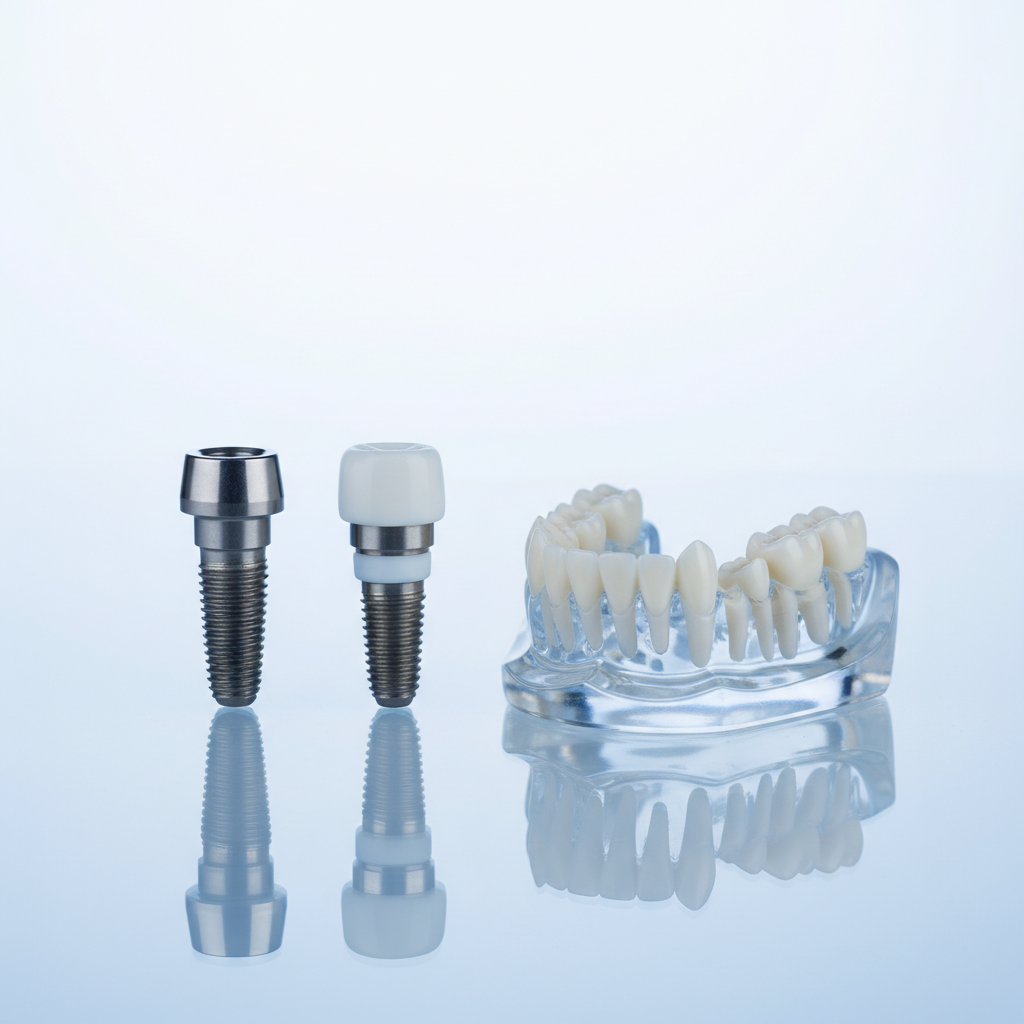
Titanium and zirconia fixtures represent the main material families used in dental implants.
2.1 Titanium and titanium alloys
Titanium remains the workhorse material for implant fixtures and screws because it combines high strength, corrosion resistance, and reliable osseointegration, and still outperforms zirconia and other ceramics for tensile and fatigue strength hence its dominance in high load posterior segments and full arch frameworks, including All on X restorations. Newer titanium zirconium alloys further improve strength while maintaining biocompatibility.
In day to day practice, this gives reliable integration even in compromised bone and broad compatibility with the major systems your lab already supports.
2.2 Zirconia and ceramic implants
Zirconia (typically yttria stabilised zirconia) offers a tooth coloured, metal free alternative. One piece and two piece ceramic implants show excellent biocompatibility, low plaque affinity, and favourable soft tissue response in the anterior zone, with promising mid term aesthetics.
Mechanical testing suggests zirconia is very hard and stiff but generally has lower fatigue resistance than titanium, and the long term clinical data set is still smaller, so many clinicians reserve zirconia fixtures for carefully selected cases while routinely using zirconia at the abutment or prosthetic level (for example, zirconia crowns and bridges) to combine strength with superior aesthetics.
2.3 Other metals, alloys, and surface treatments
Beyond pure titanium and zirconia, you’ll encounter titanium alloys, cobalt chromium in superstructures or small parts, and surface treatments that increase area and encourage bone contact.
For long span or full arch work, frameworks are either rigid cobalt chromium or more aesthetic zirconia when dimensions allow.
Surface topography matters: roughened surfaces support faster integration, smoother collars can help soft tissue stability and cleansability, and your priority is to know the surface you’re working with and align loading and maintenance protocols accordingly.
3. Main dental implant components
3.1 Implant body / fixture
The fixture is the threaded body placed into bone. It’s usually titanium or a titanium alloy, with macro design features (taper, thread profile, neck design) chosen to match bone quality and surgical protocol.
From a restorative perspective, what matters most is:
- Platform size and connection type (internal hex, conical, Morse taper, etc.).
- Platform switching and how far subcrestal the fixture sits.
- System compatibility with the digital workflow and scan bodies you’re using.
3.2 Abutments: stock, custom, and multi‑unit
The abutment connects the fixture to the restoration, passes through the soft tissue, and comes in titanium, zirconia, or hybrid designs that may be:
- Stock abutments – pre-fabricated shapes, adjusted chairside.
- Custom CAD/CAM abutments – designed from digital scans for optimal emergence profile.
- Multi unit abutments (MUAs) – used for screw retained bridges and full arch prostheses.
In practice, you’ll balance soft tissue aesthetics, cleansability, screw channel access, and retrievability, and clear prescriptions to the lab (“custom zirconia abutment on titanium base, screw retained, anterior aesthetic zone”) prevent remakes.
3.3 Prosthetic components: crowns, bridges, and overdentures
Common implant prostheses include single crowns and short span bridges typically monolithic or layered zirconia, lithium disilicate, or metal‑ceramic and implant retained overdentures on ball attachments, locators, or bars, choose materials with your lab based on load, available restorative space, and aesthetic priorities.
3.4 Screws, healing abutments, and small parts
The “small stuff” is what often delays cases:
- Prosthetic screws – typically titanium or titanium alloy, engineered for specific torque values.
- Cover screws and healing abutments – shaping soft tissue and protecting the interface during healing.
- Scan bodies / impression copings – transferring the 3D position of the fixture to the lab accurately.
- Overdenture attachments – ball, locator, or bar components, with replaceable nylon or elastic inserts.
A clear component list in your lab sheet (system, platform, connection, and any existing prosthetic parts) dramatically reduces the risk of mismatched screws or reordering delays.
4. Key takeaways: matching materials to clinical scenarios
Once you understand the main components and materials, the practical question is which combination suits each case; the scenarios below offer a simple framework you can adapt chairside and in your lab prescriptions.
- High load posterior implant with limited restorative space – Use a titanium fixture with a titanium or titanium base abutment and a monolithic zirconia or metal ceramic crown or bridge, preferably screw retained; where access or space is very limited, a short cemented abutment or slim Co–Cr framework is a practical fallback.
- Single tooth in the anterior aesthetic zone – Use a titanium fixture with a custom zirconia abutment on a titanium base and a high translucency zirconia or lithium disilicate crown, prioritising soft tissue support and switching to cement‑retention only if the screw channel would emerge facially.
- Patient seeking a “metal free” solution or with metal sensitivity concerns – Favour titanium fixtures combined with zirconia abutments and zirconia or lithium disilicate restorations to minimise visible metal, reserving zirconia fixtures for carefully selected cases and documenting the discussion about evidence and limitations.
- Full arch or All on X case with bruxism or heavy occlusion – Plan titanium fixtures with multi unit abutments and a screw retained full arch prosthesis such as All on X restorations, choosing monolithic zirconia where space and forces allow and a rigid metal framework (titanium or Co–Cr with ceramic or composite layering) when vertical space is tight or occlusal loads are high.
In all of these scenarios, early lab input ideally with intraoral scans, photographs, and a brief note on occlusion helps you land on a material and component combination that is technically feasible and maintainable long term.
5. How NovaDent works with implant materials and components
NovaDent helps convert your treatment plan into a clear, compatible combination of fixtures, abutments, and prosthetic materials.

A digital lab workflow allows implant fixtures, abutments, and restorations to be planned cohesively.
- Support major titanium implant systems and multi unit platforms used across Australia.
- Design custom titanium and zirconia abutments and CAD/CAM frameworks for single units, bridges, and full arch All on X restorations.
- Work from intraoral scans or traditional impressions within streamlined digital workflows and published turnaround times.
If you’re unsure which combination of fixture, abutment, and prosthetic material makes the most sense, our team can review your scans and photographs and suggest options aligned with our implant price list.
FAQs
Are all dental implants made from titanium?
No. Most contemporary systems still use titanium or titanium alloys for the implant body because of their long term clinical performance. Zirconia and other ceramics are also used, particularly where a metal free approach or highly aesthetic anterior outcome is desired, with other alloys appearing mainly in prosthetic components rather than in the fixture itself.
What are the main dental implant components I need to specify on a lab sheet?
At a minimum, list the implant system and platform, connection type, abutment type and material (stock or custom; titanium or zirconia), retention method (screw or cement retained), prosthetic material, and for overdentures or bars the attachment system; combined with good digital scans, this lets your lab choose compatible components and design efficiently.
How do we know these materials are safe for patients long term?
Implant materials are tested against international standards (for example, ISO and ASTM) for biocompatibility, corrosion resistance, and mechanical behaviour before clinical use, and titanium systems in particular have strong long term data, with meta-analyses reporting around 96% implant-level survival at 10 years for modern endosseous implants. Zirconia has a growing, though still smaller, evidence base, so many clinicians reserve it for carefully selected indications.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website