Many patients mention waking with a sore jaw, headaches, or a partner complaining about noise at night. As clinicians, you know there is often more going on than “just stress”. Teeth grinding (bruxism) sits at the intersection of occlusion, sleep, psychology and lifestyle and it can quietly damage teeth and restorations you’ve worked hard to place.
This guide walks through the current thinking on causes and symptoms, with a practical lens for chairside assessment and appliance prescription. By the end, you’ll have a clearer structure for deciding when to reassure, when to monitor, and when to prescribe a protective appliance or involve your lab and other providers.
TL;DR
- Bruxism can be sleep-related, awake, or mixed, and is often linked to stress, sleep disorders and some medications.
- Early clinical signs include tooth wear, fractured restorations, linea alba, tongue scalloping and muscle tenderness.
- A mouth guard for teeth grinding can protect teeth and work well as part of a broader plan that may include stress management or sleep assessment.
- Clear lab prescriptions and good records lead to better fitting occlusal splints, fewer adjustments, and happier patients.
What is bruxism?
Bruxism describes repetitive jaw muscle activity that involves clenching, grinding or bracing of the teeth. It is usually split into:
- Sleep bruxism – rhythmic or sustained activity during sleep, often reported by a partner.
- Awake bruxism – clenching or bracing during waking hours, often linked to concentration, posture or stress.
For the dental team, the label matters less than the impact: enamel wear, fractured cusps, failed crowns and muscular symptoms. On the lab side, repeated remakes on the same patient can be an early clue. If your practice uses digital impressions, comparing scans over time can make progressive wear easier to track.
For patient facing explainers and broader overviews, you can direct patients to the NIDCR bruxism overview, ADA teeth grinding resources and materials from the Sleep Health Foundation during your discussions.
How common is grinding teeth in sleep?
Current estimates suggest that sleep bruxism affects roughly 8 to 10% of adults, with higher rates reported in children and adolescents and broader reviews indicating that bruxism of any type is relatively common in the general population, in day to day practice, only a subset of these patients develop clinically significant tooth wear or restorative complications.
Causes of bruxism: daytime and sleep
Bruxism is usually multifactorial. Key contributors include:
- Psychological and lifestyle factors – stress, anxiety, mood disturbance and hypervigilance, plus habits such as high caffeine, alcohol or tobacco use.
- Sleep and breathing disorders – sleep disordered breathing and other sleep related movement disorders.
- Medications and systemic conditions – some antidepressants and stimulants, neurological conditions and other systemic disease.
- Occlusion and vertical dimension – not usually a primary cause, but occlusal schemes can modify how bruxism expresses itself.
These factors typically act together, which is why mechanical protection with an occlusal splint generally sits alongside stress management, sleep assessment or medication review rather than replacing them.
Signs and symptoms patients may report
Patients often describe bruxism in their own words long before you see the full clinical picture. Common stories include:
- “My jaw feels tight when I wake up.”
- Morning headaches around the temples.
- Tooth sensitivity without obvious caries.
- A partner hearing grinding teeth in sleep or seeing clenching.
- Episodes of earache or “blocked ear” with no ENT findings.
These symptoms often sit against a background of work or family stress, so a short, empathetic conversation usually elicits context more effectively than a long checklist. This section also adapts well as a patient facing checklist on your own clinic site, supported by selected posts from the NovaDent clinical blog.
Clinical examination: what to look for chairside
A structured, repeatable exam helps you distinguish active bruxism from historical wear patterns or other causes.
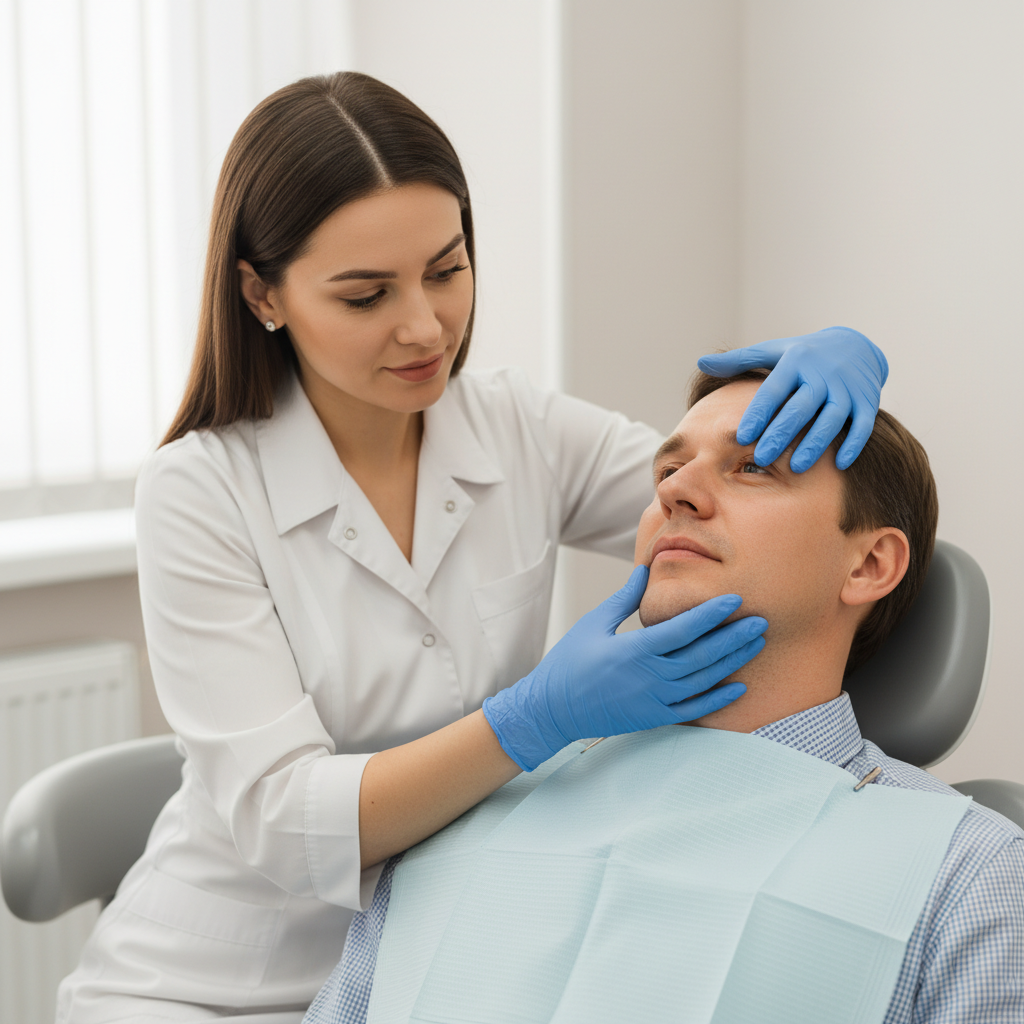
Extraoral and TMJ findings
- Hypertrophy or tenderness of masseter and temporalis muscles.
- Clicking, crepitus or deviation on opening.
- Limited opening or locking episodes.
Intraoral signs
- Attrition facets matching in ICP and excursive positions.
- Chipping at incisal edges and cusp tips.
- Fractured cusps, craze lines, or debonded restorations.
- Gingival recession and abfraction lesions that seem out of proportion to brushing habits.
- Linea alba on the buccal mucosa, tongue scalloping.
Simple functional checks
- Ask the patient to show “how your teeth sit when you’re concentrating”.
- Check for strong clenching when you lightly tap the canines or premolars.
- Note parafunctional habits like nail biting or pen chewing.
Photographing wear patterns and splint surfaces at reviews, especially when working with a digital first lab such as NovaDent Labs, helps you monitor change over time.
When a mouth guard for teeth grinding helps (and when it doesn’t)
Occlusal appliances are often the first mechanical line of defence. They do not “cure” bruxism, but they can:
- Protect enamel, restorations, and implants from further damage.
- Redistribute forces across the arch.
- Provide a smoother, more stable occlusal surface.
- Offer some reduction in muscle pain for selected patients.
The Reassure, Monitor, Protect triage
A simple way to triage bruxism chairside is to think in terms of “Reassure, Monitor, Protect”:
- Reassure – minimal wear, no symptoms, no high value restorative work at risk. Educate, address habits, and review at routine recalls.
- Monitor – early wear, occasional symptoms, or planned restorative or implant work. Document photographs or scans, record occlusion and review in 6 to 12 months.
- Protect – ongoing fractures, moderate severe wear, existing crowns or implants at risk, or TMJ symptoms. Prescribe an appropriate splint and consider broader medical or psychological contributors.
“Not every grinder needs a splint immediately, use Reassure, Monitor, Protect and escalate when risk changes.”
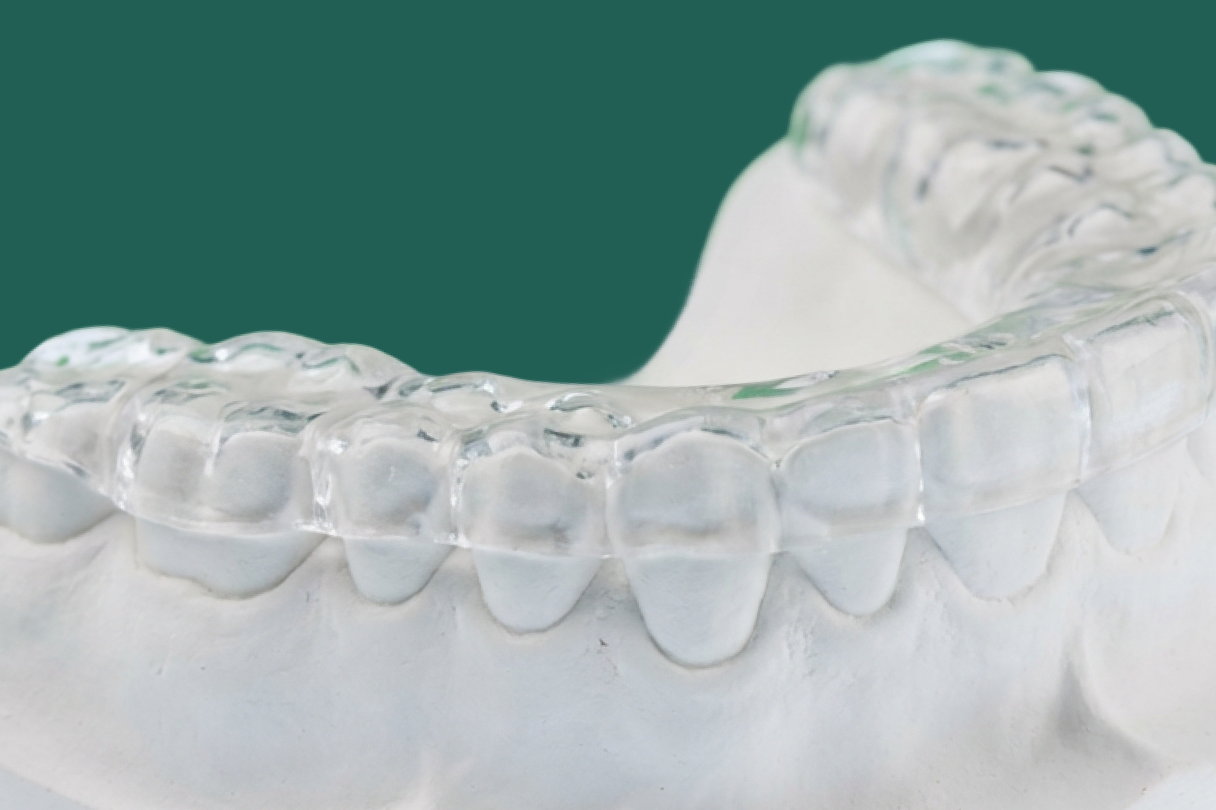
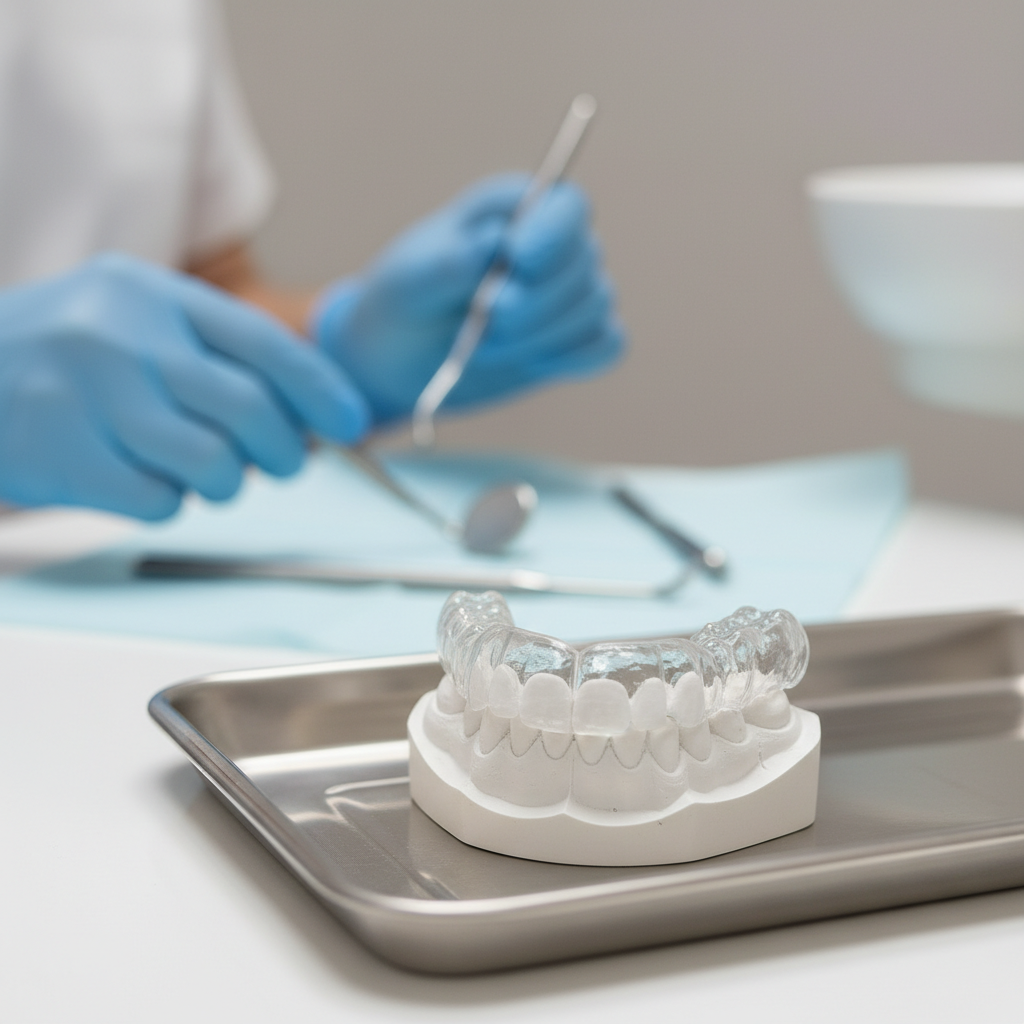
Comparing common splint and guard designs
Once a patient is in the “Protect” category, design decisions matter. Full coverage, hard acrylic maxillary splints remain a mainstay, but you may also prescribe mandibular splints, soft guards or combination designs depending on occlusion, aesthetics and patient preference.
Hard acrylic maxillary flat plane splint
- Typically offers the most predictable, adjustable occlusal scheme for moderate high bruxism risk.
- Easy to fine tune contacts and guidance chairside and to add or remove acrylic as restorative plans evolve.
- Often preferred where you are protecting multiple crowns, bridges or implants in the opposing arch.
Hard/soft (dual laminate) night guard
- Soft inner layers can improve initial comfort and acceptance for anxious or gag prone patients.
- A hard outer layer provides better wear resistance than a purely soft guard, but is usually less adjustable than a full hard acrylic splint.
- Night guard is useful for low moderate risk cases where comfort and compliance are your main concerns.
Mandibular splint
- Helpful where maxillary aesthetics are a concern, or where upper arch anatomy or restorations limit bulk and retention.
- It can be easier for some patients to tolerate socially if they remove it just before getting out of bed.
- Needs the same attention to occlusal design and excursions as a maxillary splint, do not treat it as a “less serious” option.
Over the counter vs custom devices
- Boil and bite or preformed guards may offer short term protection in very mild cases or while a patient saves for custom work.
- They are bulkier, less retentive and less durable, and can create uneven contacts or soft tissue irritation.
- For patients with moderate severe bruxism, existing restorative work, or TMJ symptoms, a custom, lab made splint is almost always the safer option.
Case vignette: when “Monitor” becomes “Protect”
A 46 year old attends recall with jaw tightness, mild wear and a fractured restoration; with upper crowns planned, you document findings and classify him as “Monitor”. Six months later a cracked crown and night‑time grinding reported by his partner prompt you to shift to “Protect” with a hard maxillary splint and a sleep study; symptoms settle and there are no further fractures.
Be cautious in patients with suspected moderate severe sleep apnoea, a guard that simply holds the jaw in a retruded position can aggravate snoring and airway issues. In these cases, co-management with a sleep physician and consideration of mandibular advancement devices for example in collaboration with a lab experienced in sleep appliances often makes more sense than a simple night guard, given the overlap between sleep apnoea and bruxism. Patient friendly overviews of diagnosis and management, such as the Mayo Clinic treatment page, can support these discussions.
“In suspected sleep apnoea, a simple night guard can worsen airway issues co‑manage with a sleep physician.”
Working with your lab on splints and guards
Bruxism cases live or die in detail. A short extra step in your prescription can save you a chairside adjustment appointment later.

Key details to include on your lab sheet
- Preferred arch (maxillary or mandibular) and material.
- Desired occlusal scheme: flat plane, canine guidance, anterior guidance, or customised design.
- Centric relation vs ICP instructions, and whether you supplied a separate bite record.
- Any recent major restorative work, implants or ortho that needs special protection.
NovaDent Labs works with general dentists and specialists across Australia on bruxism appliances, night guards and sleep devices. Digital impressions and CAD/CAM workflows support predictable fit and occlusion. To standardise these cases with one lab partner, you can request our current price list for your team and share our occlusal splint workflow with associates.
When to co-manage or refer
Many mild cases can be handled entirely within general practice, but some merit a broader team:
- Suspected sleep apnoea – loud snoring, witnessed apnoeas, daytime sleepiness: refer to a sleep physician for assessment.
- Severe psychological distress – consider GP and psychology input alongside dental care.
- Persistent or worsening TMJ dysfunction – involve an orofacial pain specialist or oral medicine specialist.
- Extensive restorative plans – work with a prosthodontist and your lab on sequence and splint design.
Positioning your practice as a central coordinator rather than the sole solution builds trust and tends to improve long term outcomes for patients and their restorations. Professional bodies such as the Australian Dental Association list local specialists and provide concise summaries of complications such as fractured teeth, jaw joint pain and damaged dental work.
Talking with patients about bruxism without alarming them
No one likes to be told they are “destroying their teeth”. Calm, practical language tends to work better:
- Frame bruxism as a habit the body has picked up, not a personal failing.
- Explain that you are protecting teeth and joints while other contributors such as stress or sleep issues are addressed, and set clear expectations about how often to wear the appliance and how it should feel.
- Use simple visuals: photos of wear facets or cracked fillings, or coloured markings on the splint at review.
A printed or emailed handout that summarises this conversation perhaps hosted on your clinic website and supported by the NovaDent clinical blog helps reinforce the message at home.
FAQs
What causes grinding teeth in sleep?
Most patients have a mix of predisposing factors: genetics, sleep disordered breathing, and psychological load such as stress or anxiety. Triggers such as stimulants, alcohol and poor sleep routines can flare episodes, which tend to fluctuate over time. Regular reviews and updated records help you keep the bigger picture in view.
Does every patient need a mouth guard for teeth grinding?
Not every patient with bruxism needs an appliance straight away; some have minimal wear and no symptoms, so monitoring and simple habit counselling may be enough initially. Once you see ongoing wear, new fractures, or you are placing higher‑value restorations or implants, a protective splint becomes hard to argue against. Match splint design to risk level, occlusion and patient tolerance.
How long should patients wear a night guard each day?
For sleep bruxism, most clinicians recommend wearing the guard every night for the full sleep period. For awake bruxism, some patients benefit from a slim guard during high risk tasks such as intense desk work, with appliance condition and fit reviewed regularly.
Can teeth grinding damage dental implants or crowns?
Yes. Repeated clenching and grinding can chip porcelain, loosen screw retained components and contribute to fracture or loss of both crowns and implants, so many clinicians place these patients at least in the “Monitor” category and often “Protect” with a hard acrylic splint.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website