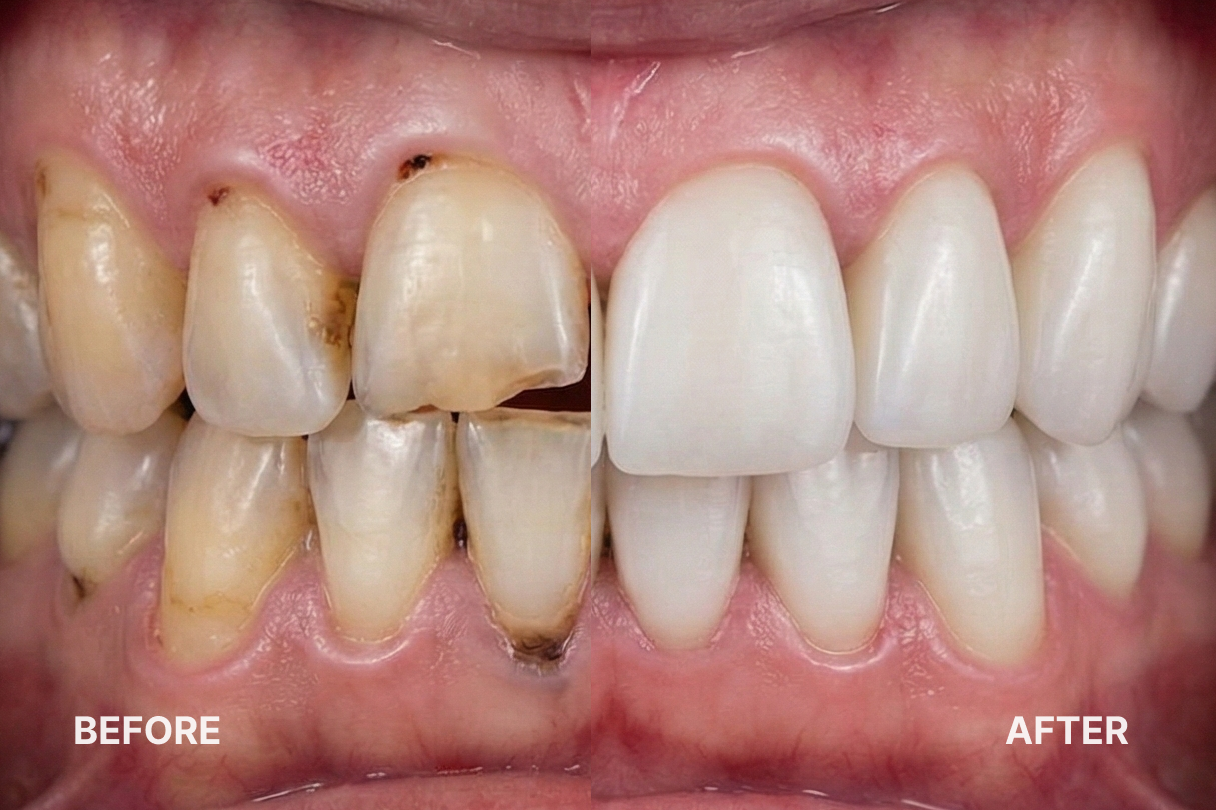
Most days in general practice start with a familiar scene: a patient in your chair with an old amalgam that has finally given up, or a cusp fractured off a premolar the night before. You’re not just filling a hole, you’re deciding how to rebuild a whole functional unit. That’s where teeth restoration comes in.
The question isn’t just what material to use. It’s: When is intervention really indicated? How much structure can you preserve? At what point should you move from a small adhesive increment to an indirect onlay, crown, or implant restoration? And how do you use your lab so the work on the model matches what happens chairside?
This article walks through the “when and why” of tooth restoration, how adhesive systems have reshaped decision making, and where a digital focused lab can quietly de-stress your restorative days.
A consultation where the restorative plan is discussed often sets the tone for the whole teeth restoration journey.
TL;DR
- Restore when lesions are cavitated, plaque-retentive, symptomatic, or structurally compromising; monitor early, non cavitated and shallow cervical lesions.
- Use direct restorations for small moderate defects; step up to indirect onlays or crowns when cusps, endodontically treated teeth, or vertical dimension need protection.
- Adhesive techniques let you replace only what’s missing instead of cutting full crowns purely for retention.
- Involve your lab early for cracked, endo, wear, implant, and full-arch cases so the restoration design follows your functional plan.
- Standardised photos, scans, and prescriptions reduce remakes and bring crown/onlay fits much closer on first try in.
What do we mean by teeth restoration?
In a clinical sense, tooth restoration is any intervention that rebuilds lost hard tissue to restore function, anatomy, and, ideally, aesthetics. That spans a wide spectrum:
- Small direct composite for Class I and II lesions
- Adhesive onlays/overlays replacing one or more cusps
- Full coverage crowns on endodontically treated posterior teeth
- Veneers and partial coverage restorations in the aesthetic zone
- Implant crowns and bridges when a tooth is no longer restorable
The unifying idea is simple:
Replace what’s lost while preserving what is sound.
With modern materials and adhesive luting, that balance has shifted away from “retention by removal” toward bonding to enamel and dentine where possible, so you can protect cusps without automatically jumping to full crowns.
For patient facing information on restorative dentistry, many clinicians lean on resources like the Australian Dental Association and share clear summaries of the main types of tooth restoration, while keeping the nuanced case by case decisions for the surgery.
When is tooth restoration actually needed?
It’s tempting to think every lesion demands a restorative solution. In reality, early lesions, non cavitated white spot lesions, and some smooth surface caries may be better managed with prevention and remineralisation protocols.
1. Caries and structural loss
Once a lesion is cavitated and plaque retentive, or there is clear undermining of marginal ridges, it moves into restorative territory. Key triggers for intervention include:
- Cavitated lesions not cleansable by the patient
- Radiographic evidence of dentinal involvement with clinical cavitation
- Existing restorations with secondary caries or open margins
2. Fractures and cracks
We all know the story: heavily restored molar, patient chewing on something “not that hard”, and suddenly a buccal or lingual cusp shears off. Here, the decision is less about whether to restore and more about how far to extend:
- Small chip with intact occlusion: direct bonded build up may suffice.
- Fractured functional cusp or split tooth: indirect onlay or full coverage is usually more predictable.
3. Endodontically treated teeth
Post endo teeth often arrive at the lab with significant loss of coronal structure. The guiding thought here is ferrule and cuspal protection, not just “plugging the access”.
- Minimal structural loss: bonded onlay may be adequate.
- Moderate severe loss: full coverage crown with 360° ferrule, often on a post/core foundation.
4. Wear, erosion and parafunction
Erosive wear, bruxism, and attrition present differently, but the restorative question is similar: can you safely restore anatomy and vertical dimension while managing the aetiology?
In these cases, staged tooth restoration using blended direct and indirect restorations, plus occlusal appliances, often gives better long-term stability than isolated “patch” fillings, especially when splints are integrated into a broader functional plan.
5. Non carious cervical lesions and abfraction
Non carious cervical lesions (NCCLs) including those attributed to abfraction present as wedge shaped or saucer shaped defects at the cemento enamel junction. Their aetiology is multifactorial, with abrasion, erosion, and occlusal stress all implicated to varying degrees. Crucially, restoring the defect does not in itself treat the underlying cause or reliably stop progression.
A pragmatic approach is to restore NCCLs when there are clear clinical consequences or risks, such as:
- Persistent dentine hypersensitivity not controlled with non invasive therapies
- Extensive tissue loss compromising structural integrity or approaching the pulp
- Subgingival or plaque retentive margins that the patient cannot clean
- Aesthetic concerns in the smile zone that matter to the patient
- Caries associated with the lesion, or when the tooth will act as a prosthetic abutment
Shallow, non sensitive lesions (<1 mm deep) that are not trapping plaque can often be monitored with regular photographs and models while you address risk factors: adjust toothbrushing technique, manage dietary acids, and, where occlusal stress is suspected, consider night time splints or other occlusal therapy rather than “chasing” every notch with composite.
Direct and indirect tooth restoration options
Once you’ve decided intervention is indicated, the next choice is whether a direct or indirect approach makes most sense for that tooth and that patient.

Clear conversations about direct versus indirect teeth restoration options help align treatment with each patient’s needs.
Direct restorations
Direct restorations are placed in a single visit, shaped intraorally. Typical options:
- Resin composite (nanohybrid, bulk fill, etc.)
- Glass ionomer and resin modified glass ionomer
- Compomers in selected situations
Directs are ideal for:
- Small to moderate Class I/II, III and V lesions
- Situations where access and moisture control are predictable
- Interim restorations prior to definitive indirect work
Indirect restorations
Indirect restorations are fabricated outside the mouth and bonded or cemented later. These include:
- Inlays and onlays (ceramic, composite, hybrid ceramics)
- Partial coverage overlays and endo crowns
- Full coverage crowns in metal ceramic, zirconia, or lithium disilicate
In a digital lab setting, these restorations are typically designed via CAD and milled or printed before finishing. Labs like NovaDent’s fixed prosthetics service then become an extension of your clinical planning: occlusion, proximal contacts, and emergence all flow from your prep and prescription.
Well designed ceramic onlays and partial crowns can perform at least comparably to full crowns over the medium term. One systematic review reported survival of about 96% for ceramic onlays/partial crowns and 80% for full crowns at a mean 6.6 year follow up in one cohort, with overall survival broadly similar between designs when case selection and preparation were appropriate.
Quick comparison: direct vs indirect
- Direct: More conservative, chairside control, lower lab cost; technique sensitive, limited for large load bearing defects.
- Indirect: Better control of contacts and occlusion, stronger materials, longevity; requires lab coordination, more steps.
Adhesive restoration teeth: how bonding changed the rules
The phrase adhesive restoration teeth gets thrown around so often that it can start to lose meaning. At its core, adhesive dentistry is about micromechanical and chemical bonding to enamel and dentine rather than retention by macro mechanical features alone.
How modern adhesive systems work
Contemporary systems typically involve:
- Enamel etching (selective or total etch) to create a high energy, micro rough surface
- Controlled interaction with dentine to form a hybrid layer and resin tags
- Low viscosity bonding resins that penetrate and polymerise within this conditioned surface
The result, when done well, is a bonded unit where the restoration and remaining tooth behave more like a single structure. This is why onlays and overlays can often replace traditional full crowns for moderately compromised cusps.
Clinical advantages and limitations
Adhesive restorations bring clear benefits:
- Preservation of sound tooth tissue (no need for excessive taper or height loss)
- Improved distribution of occlusal forces across bonded surfaces
- Better aesthetics, especially with ceramic or composite systems
But there are trade offs your treatment plan has to respect:
- Moisture control is non negotiable for predictable bonding.
- Heavily cracked roots or vertical fractures won’t be “held together” by adhesive materials.
- Parafunction and limited posterior support may call for stronger materials and designs.
For a concise refresher on how adhesive techniques have reduced the need for full coverage crowns in many aesthetic situations.
How much to restore, and when to involve the lab
One of the trickiest chairside moments is deciding how far to go. Do you leave a slightly undermined cusp and “watch it”, or include it in an onlay? Do you restore a worn anterior segment at the existing vertical dimension, or open it with a full occlusal scheme?
A simple three question framework
Many clinicians use a mental checklist like this:
- Can the remaining tooth reliably withstand occlusal load?
- Can the patient clean the margins long term?
- Does this design give me a clear path if or when it fails?
If the answer to any of these is “not really”, that tooth is probably a candidate for a more protective indirect tooth restoration, often planned with your lab’s input.
Treat your lab as a planning partner, not just a supplier.
Key details to share with your lab
A lab can only design as well as the information it receives. On your lab sheet or digital prescription for onlays, crowns, or implant restorations, include:
- Clear material request (e.g. lithium disilicate vs monolithic zirconia)
- Shade plus characterisation expectations (especially in the anterior)
- Occlusal scheme notes (canine guidance vs group function, known parafunction)
- Any planned vertical dimension changes or transitional splint therapy
Labs with a strong clinical background, such as the NovaDent Labs team in Sydney, are often happy to review pre-op photos, scans, and notes to suggest material and design options before you prep.
How a digital lab supports predictable restorations
In a digital workflow, the handoff between your chair and the lab bench is no longer a padded box and a handwritten slip. Instead, it’s a data set and a set of expectations.
Digital CAD/CAM design allows the lab to visualise your preparation and plan the teeth restoration in detail before fabrication.
Intraoral scanning and CAD/CAM
When you scan rather than take impressions, you give your lab:
- Clear margin visibility and immediate feedback if data is missing
- Bite registrations that can be rechecked and adjusted on screen
- Efficient transmission for faster start on design and milling
Labs that accept all major intraoral scanner file formats and run CAD/CAM workflows can then design restorations that:
- Respect minimal thickness for ceramics and hybrid materials
- Provide consistent proximal contacts and occlusal schemes
- Reduce the time you spend adjusting in the chair
If you’re moving more of your restorative work to digital, it’s worth looking at how your lab manages digital dentistry workflows, from file intake to quality checks and remake monitoring.
Documenting cases for your lab
Digital tools only help if the supporting records are consistent. A simple documentation protocol for crowns, onlays, and implant restorations might include:
- Photo set: full face and smile views, retracted frontal and lateral views, occlusal views, and at least one properly lit shade tab photo adjacent to the reference tooth.
- Scan set: initial pre-op scan, a separate preparation scan with clear margins, opposing arch, and a dedicated bite registration.
- Prescription notes: occlusal scheme, parafunctional habits, planned changes to length or buccal corridors, and any special emergence profile or contour requests.
Many digital teams standardise around a “three scans, three photo series” model for each case, which makes it easier for technicians to design accurately and has been associated anecdotally with fewer remakes and shorter adjustment times once everyone follows the same protocol.
Turnaround times and consistency
Predictable turnaround typically around 5 to 9 business days for a well organised local lab lets you schedule reviews, endo completions, and restorative visits with more confidence.
At NovaDent, ISO 9001/13485 aligned quality systems, TGA compliant manufacturing, and documented material traceability underpin those timeframes, so your crowns, onlays, splints, and implant restorations arrive with consistent contacts, occlusion, and shading rather than last minute surprises. You can review the lab’s certifications and compliance to see how these standards are implemented.
Over months, that consistency fundamentally changes how you feel about large restorative days. Instead of wondering how much you’ll be trimming a crown, you can focus on the clinical conversation with the patient.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website