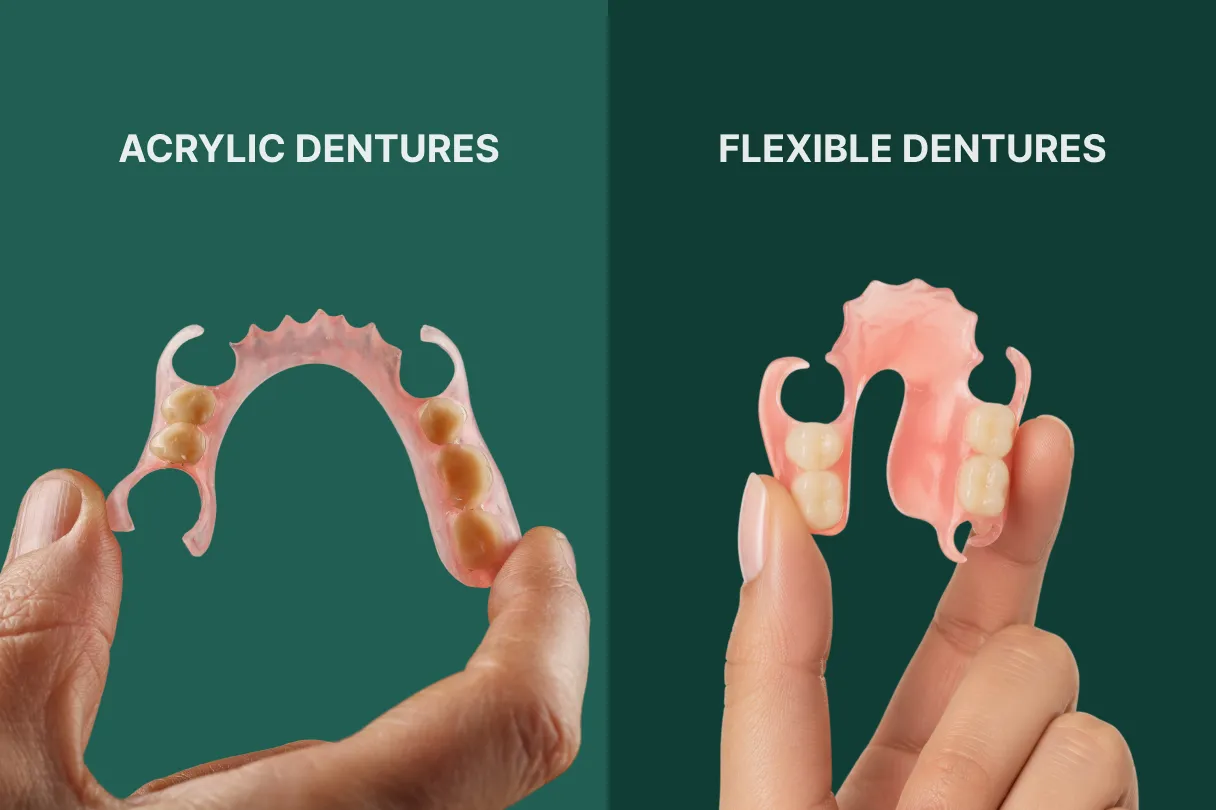
If you restore removable dentures regularly, you already field the “acrylic vs flexible dentures” question from patients who want comfort, a natural look, and something that lasts. At the same time, you have to consider occlusion, ridge changes, hygiene, future adjustments, and how your lab will deliver the design.

This guide compares flexible dentures vs acrylic from a clinician lab perspective, focusing on the first 12–24 months after delivery when most remakes, relines, and adjustments occur. We’ll use a simple R-O-P framework (Ridge, Occlusion, Patient priorities) so you can match each base material to the ridge, occlusion, and expectations in front of you, and integrate it with your broader denture types and treatment options.
TL;DR:
- Acrylic dentures (PMMA bases) are rigid, adjustable, repairable, and better for significant occlusal changes, immediate dentures, and most complete dentures.
- Flexible dentures (nylon or polyamide bases) are thin and comfortable, with great aesthetics around clasps, but they are harder to reline, modify, or repair.
- Flexible partial dentures vs acrylic: flexible works well for small free end or bounded saddles, undercut rich ridges, and patients who reject metal show; acrylic is usually preferable for extensive tooth loss and when you anticipate multiple adjustments.
For most cases, the question isn’t “Which material is best overall?” but “Which material is best for this ridge, occlusion, and patience?”
What do we mean by “acrylic dentures”?
In this article, “acrylic dentures” refers mainly to PMMA (polymethyl methacrylate) bases used for:
- Conventional complete dentures
- Transitional or immediate dentures
- Partial dentures on an acrylic base with wrought-wire or cast clasps
Acrylic bases are rigid, familiar, and relatively easy to adjust, reline, and repair. If a tooth fractures or a clasp needs replacing, your lab can often process changes without remaking the entire prosthesis, which is why acrylic remains the workhorse for many removable prosthetics and denture cases.
PMMA remains the reference denture‑base material, with well‑characterised stability and biocompatibility compared with newer resins (see this review), and digital workflows now let us mill acrylic bases with consistent thickness and fit for easier relines and occlusal adjustments over the first 12–24 months.
What do we mean by “flexible dentures”?
“Flexible dentures” generally means partials made from nylon‑based or polyamide resins. These materials are:
- Flexible at intraoral temperature
- Fracture resistant in thin section
- Available in gingival shades, with tooth coloured or gingival coloured clasps
Flexible dentures are used almost exclusively as partials; full flexible dentures rarely deliver the occlusal stability you want. They shine in cases where patients prioritise comfort and metal free aesthetics, and where undercuts can be used for mechanical retention without significant tooth preparation. Common systems such as Valplast partials use tissue coloured nylon to achieve this.
Evidence is still limited but consistent: reviews and small clinical studies report that flexible partials deliver high aesthetic and comfort scores, although surfaces may be rougher and more prone to staining than PMMA and they are best used selectively. In a Nigerian quasi experimental study (n=30), 70% of patients were more satisfied overall with flexible RPDs and about 63% reported better comfort while eating than with acrylic designs, while a recent Maltese cohort (n=14) found no significant short term difference in objective masticatory performance between acrylic and flexible partials.
Acrylic dentures vs flexible dentures: side by side
When you line up acrylic vs flexible dentures on the factors that matter chairside, the trade offs become clearer.
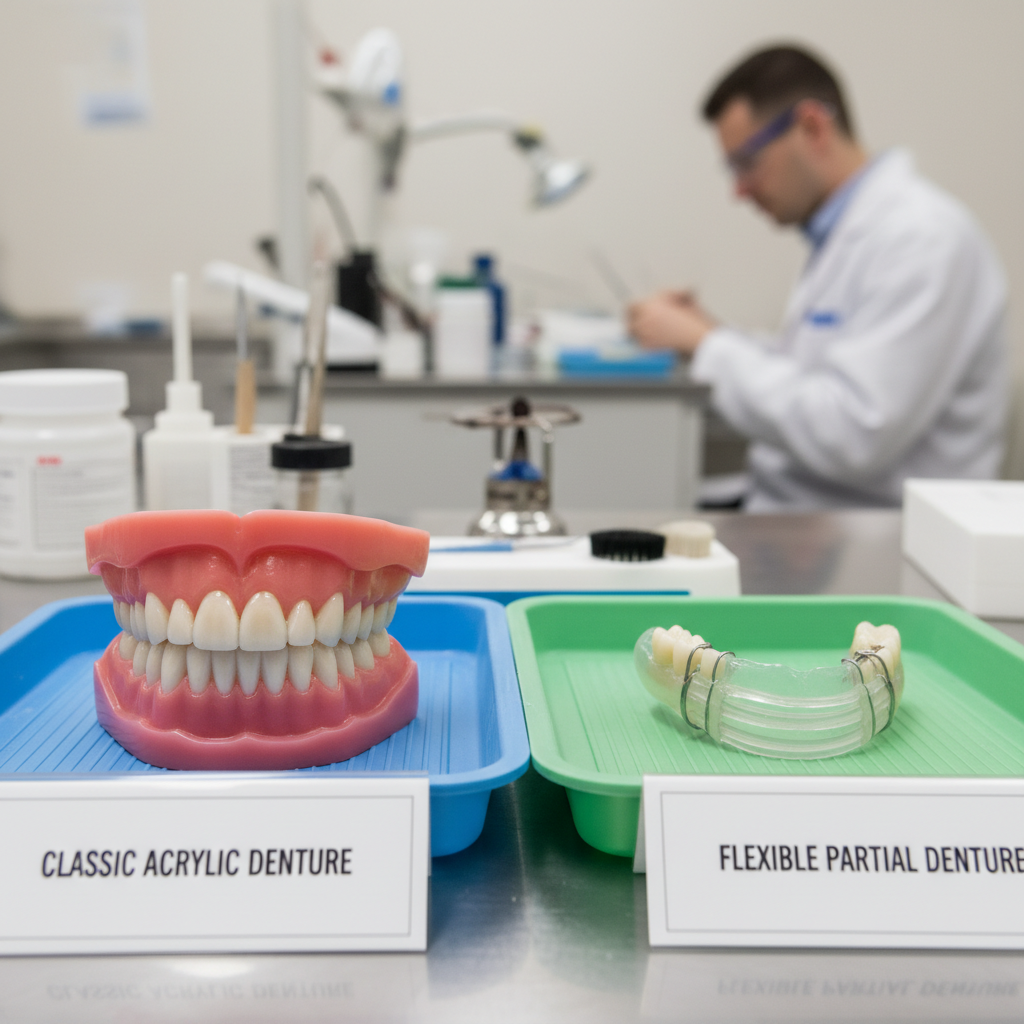
Conceptual lab view of acrylic vs flexible dentures on a workbench, highlighting differences in bulk and design.
From a lab perspective, our digital denture workflows for acrylic now let us design and mill PMMA for consistent fit and repeatability across arches. Flexible materials continue to improve but behave very differently at the bench, particularly around surface finishing and clasp design.
This table really summarises your R‑O‑P decision points: how the ridge will remodel under each design, what occlusion you can support with a rigid vs flexible base, and how well each option matches the patient’s priorities for comfort, aesthetics, and maintenance.
When acrylic is usually the better choice
So, in flexible dentures vs acrylic, when does acrylic clearly win? In many practices, these situations still lean strongly toward acrylic bases:
- Complete dentures requiring stable occlusion and future relines.
- Immediate dentures where tissue changes are expected and multiple relines are likely.
- Extensive tooth loss with long span saddles or challenging occlusal schemes.
- Patients with heavy parafunction, where excessive flexure could be an issue.
Acrylic gives you freedom to reestablish OVD, adjust occlusion, and reline as the ridge remodels, and it remains the most familiar, guideline consistent material for most practices, including Australian settings.
In full denture cases in particular, the ability to reline and reestablish occlusal contacts as the ridge resorbs over time is usually more important than having a very thin, flexible base. A well contoured acrylic flange can also support soft tissues and lip profile in a way that most flexible bases cannot reliably duplicate.
In borderline cases, quickly run through R‑O‑P (Ridge, Occlusion, Patient priorities): is the ridge likely to change significantly, do you need a rigid base to control the occlusion, and how much does the patient value future adjustability over initial comfort?
When flexible partial dentures shine
On the other side of the acrylic dentures vs flexible dentures question, there are very clear wins for flexible partials:

Chairside discussion about when flexible partial dentures may be preferable for comfort and aesthetics.
- Small to moderate bounded saddles where you can use natural undercuts.
- Pronounced undercuts or tori where rigid acrylic would require significant block‑out or surgery.
- Patients strongly opposed to metal shows but not suited to cast frameworks.
- Interim partials before implant placement or more definitive rehabilitation.
For these cases, flexible partial dentures vs acrylic often means trading some long‑term adjustability for immediate comfort and improved aesthetics. Many patients with previous rigid partials describe flexible as “less intrusive”, and small comparative studies commonly report higher short term satisfaction scores for flexible designs when anterior aesthetics are involved.
Flexible partials are also useful where you want to avoid additional tooth preparation, such as rests on heavily restored abutments. Tissue borne, flexible clasps can gently engage existing undercuts and provide acceptable short to medium term function, provided you monitor tissue response and occlusal changes closely.
The main caution is span length and occlusal loading. Long free end saddles or patients with significant parafunction can deform flexible bases enough to create sore spots, occlusal discrepancies, or accelerated ridge resorption. In those scenarios, you will often get a safer, more maintainable result from an acrylic or cast metal base.
Micro case example. A 68 year old with a short bounded Kennedy Class III saddle and high aesthetic expectations was restored with a nylon‑based flexible partial using existing undercuts for clasping and light occlusal contacts. At the 12 month review, the patient reported wearing the prosthesis for all meals with no sore spots and only a minor clasp adjustment, a pattern we commonly see when flexible partials are reserved for short spans on favourable ridges with a stable occlusion.
Lab and workflow factors: flexible dentures vs acrylic
Impressions and design information
For flexible dentures, accurate undercut capture drives retention. Clear instructions on:
- Preferred clasp positions and undercut depths
- Avoidance of tissue areas prone to trauma
- Any planned future extractions or implants
help your lab design a base that grips securely without overloading tissues. For larger cases, it is helpful to indicate which teeth are “sacrificial” over the next 12–24 months so the lab can advise whether a flexible design is realistic or whether an acrylic base or cast framework will be easier to modify. A well recorded functional wash impression remains a predictable starting point for many acrylic and flexible cases.
Digital vs conventional workflows
We accept both conventional impressions and digital files from major intraoral scanners. For acrylic, CAD/CAM design and milled PMMA bases can reduce chairside adjustment time and standardise outcomes, while flexible dentures still rely largely on injection moulding workflows, with digital scans mainly used for design and occlusal planning rather than direct milling. Digital records also make it easier to evolve a case over time, for example from an acrylic immediate denture to an implant retained overdenture supported by custom abutments or zirconia bridges.
Repairs, relines, and adjustments
Repairs and modifications are where flexible dentures vs acrylic differ most:
- Acrylic – Relines, border extensions, and tooth additions are generally manageable. Fractures can usually be mended.
- Flexible – Local grinding is possible but generates heat; deep adjustments can mark the surface. Many relines require specialised techniques or remakes.
If you expect multiple post‑delivery adjustments, acrylic gives you much more room to move without a full remake. Flexible bases can perform well, but are more susceptible to surface roughening and staining, so emphasise plaque control, cleanser choice, and regular reviews in your instructions.
Explaining options to patients
Patients don’t ask for PMMA or polyamide; they ask, “Which denture will feel better?” or “Will people see the metal?” Framing acrylic and flexible options around simple, everyday ideas usually works best:
- Comfort: explain that flexibility feels softer on tissues, while acrylic feels firmer and more stable.
- Aesthetics: flexible clasps can blend with teeth and gums; acrylic partials may show more metal, depending on design.
- Future changes: acrylic is easier to adjust if teeth move, are extracted, or if the ridge remodels.
- Maintenance: flexible often needs more careful cleaning around clasps to limit plaque buildup.
After you cover these points, you can explain that your recommendation reflects how their gums and bone are likely to change, how the bite will work, and how easy each option will be to maintain and that it is consistent with contemporary denture care guidelines from specialist prosthodontic organisations.
How NovaDent Labs can support your denture cases
At NovaDent Labs in Sydney, our technicians work closely with clinicians across Australia on acrylic, flexible, and implant‑related denture cases, focusing on function, patient comfort, and predictable follow up.
We can assist with:
- Case selection for acrylic vs flexible dentures
- Framework and clasp design suggestions based on your impressions and scans
- Digital design options for acrylic dentures, including milled PMMA bases
Quick clinical checklist: acrylic vs flexible dentures
In busy sessions, a simple R‑O‑P framework (Ridge, Occlusion, Patient priorities) can quickly move you from “either could work” to a clear recommendation. Use this checklist before prescribing acrylic vs flexible.
- Confirm whether the case is complete, extensive, partial, or small bounded saddle.
- Note parafunction, occlusal scheme, and expected ridge changes over the next 12–24 months.
- Identify undercuts and soft tissue constraints that favour rigid vs flexible bases.
- Decide how many relines/adjustments you realistically anticipate.
- Match patient expectations (comfort, metal show, budget) against those findings.
If most answers point toward long spans, changing ridges, and multiple planned adjustments, acrylic usually makes more sense. If they point toward short saddles, favourable undercuts, and a patient who strongly prefers metal‑free comfort, a flexible partial can be a very reasonable choice.
FAQs
Which is better overall: acrylic dentures or flexible dentures?
There isn’t a single winner. For extensive tooth loss, complete dentures, and cases where ongoing adjustments are expected, acrylic is generally the more predictable choice. For small to moderate span partials in patients who dislike metal and value comfort, flexible dentures can perform very well when case selection and occlusion are favourable.
Are acrylic dentures stronger than flexible dentures?
Acrylic is rigid and handles compressive loads well but can fracture if thin or dropped. Flexible bases resist fracture and are forgiving if dropped, but under heavy functional load they can distort slightly, which may not suit every occlusal scheme. Strength is therefore a combination of material, design, and how the denture is loaded.
Can flexible dentures be relined or have teeth added later?
Some flexible systems allow relining and additions, but the process is more technique‑sensitive and less predictable than with acrylic. When you expect staged extractions or major ridge changes, an acrylic base usually gives you more reliable options for relines, border extensions, and tooth additions.
How do flexible partial dentures vs acrylic affect hygiene?
Flexible clasps that hug the gingival third can trap plaque if the surface finish is rough or patients struggle with interdental cleaning. Acrylic partials may be slightly bulkier but are often easier for patients to brush and soak effectively. Whichever material you choose, give clear denture hygiene instructions and review patients regularly.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website