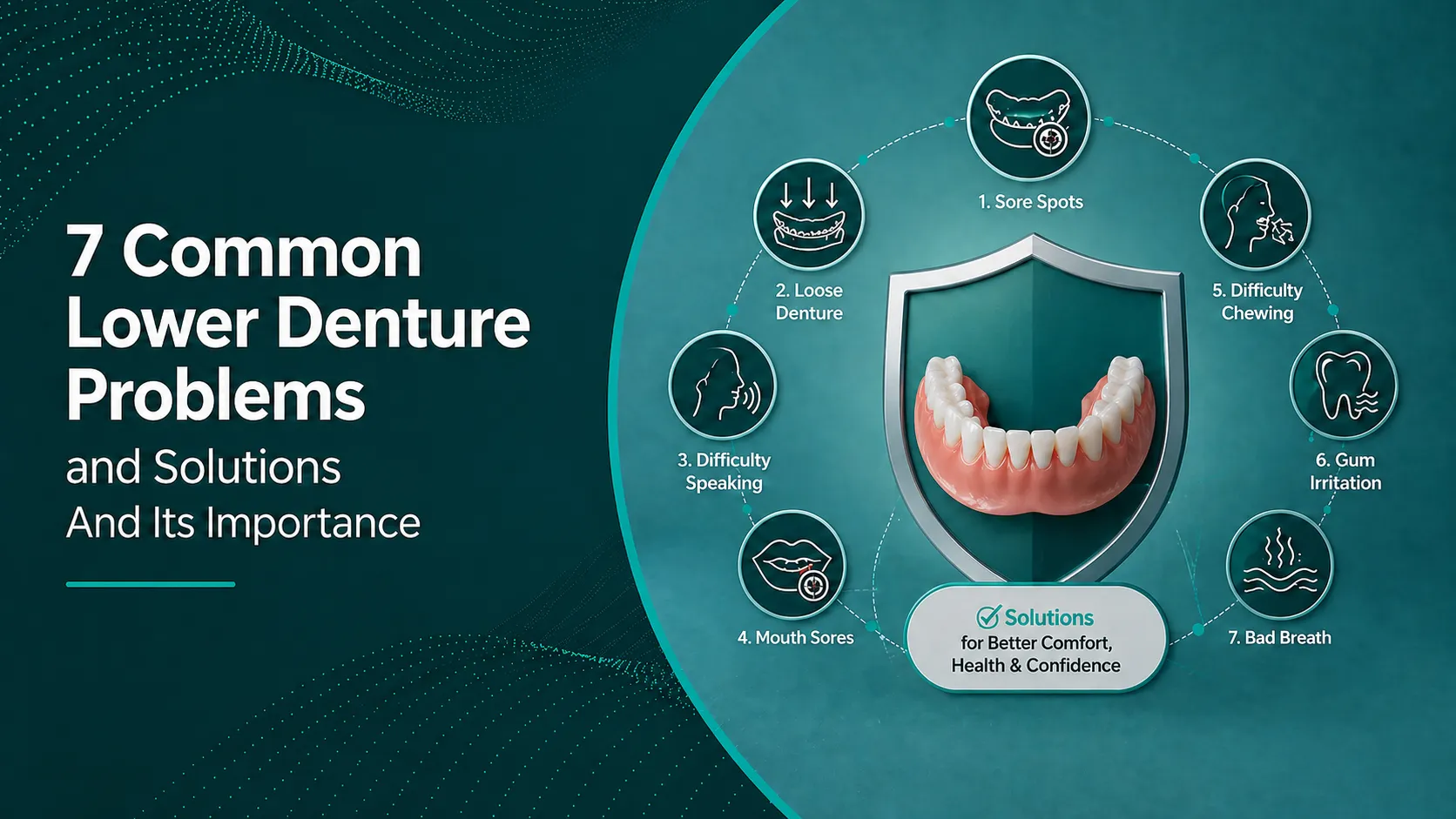
If you ask most dentists which cases keep them on their toes, lower full dentures are usually near the top of the list. Between a resorbed mandibular ridge, a mobile floor of mouth and a tongue with a mind of its own, lower dentures test both clinical skill and lab support. In this article we’ll walk through seven common lower denture problems and solutions from a practical, chairside point of view, with a strong focus on how the lab can make your life easier.
At NovaDent Labs, we see the same patterns every week: similar complaints, similar adjustment visits, and similar opportunities where a small change in impression technique, design, or material could have prevented a remake. This guide pulls those lessons together so your next mandibular complete denture feels more predictable for you and for your patient.
TL;DR:
- Lower dentures struggle because of limited surface area, mobile soft tissue and tongue activity.
- The “big seven” issues: poor retention, instability, sore spots, speech concerns, chewing difficulty, aesthetics/support, and fractures.
- Many problems trace back to border extension, occlusion, and neutral zone capture areas where the lab can give strong support.
- Mandibular implant overdentures (often with two implants) can transform function for appropriate patients.
- Consistent communication with a digital focused lab helps reduce remakes and post insertion chair time.
Why lower dentures are more challenging than uppers
Upper dentures enjoy a generous palatal surface and the advantage of atmospheric pressure. The lower arch gives you neither. Instead, you work with:
- A smaller basal seat on the mandibular ridge, often with significant resorption.
- Mobile soft tissue especially the floor of mouth, cheeks and labial frenum.
- A powerful, constantly moving tongue that shares the same real estate as the denture.
- Occlusal forces that tend to dislodge the lower denture rather than seat it.
Understanding mandibular anatomy and denture base extension is central to solving lower denture problems.
Patients, however, rarely distinguish between upper and lower; they just know “my plate doesn’t stay in.” Setting expectations while having a solid technical plan, a consistent impression philosophy and a reliable denture laboratory partner can turn a potentially stressful case into a predictable one.
The 7 most common lower denture problems
Across hundreds of mandibular complete denture cases, we see the same cluster of issues:
- Poor retention and “floating” dentures
- Instability and rocking on function
- Sore spots, ulcers and general discomfort
- Speech problems (especially “s,” “f” and “v” sounds)
- Chewing difficulty and reduced efficiency
- Aesthetic dissatisfaction and loss of lower facial support
- Denture fractures, midline cracks and tooth debonding
Let’s look at each of these lower denture problems and the lower denture solutions that tend to work best from both a clinical and lab perspective.
Problem 1: Poor retention and “floating” lower dentures
What it looks like
The classic complaint: “Doctor, my bottom denture won’t stay in.” The plate lifts during speech, dislodges with tongue movement, or pops up when the patient starts to chew.
Practical solutions
- Border extensions: Under-extended borders reduce the effective seal. A functional impression with proper border moulding, especially in the retromylohyoid space, can transform stability.
- Neutral zone recording: Where muscular forces balance, the denture sits more peacefully. Techniques that record the neutral zone and clear lab instructions help us set up teeth and contours that work with muscles, not against them.
- Tissue adaptation: For digital cases, accurate intraoral scans or well made impression scans, combined with a consistent CAD/CAM denture protocol, can improve fit consistency.
- Adhesives as a short term aid: For some patients, denture adhesive (as per ADA patient guidance on dentures) may help while tissues settle or until a reline is completed.
Problem 2: Instability and rocking during function
What it looks like
The denture pivots around a fulcrum often the premolar region when the patient bites on one side. You might see shiny areas on the base, localised soreness, or repeated complaints of “it feels like it tips.”
Practical solutions
- Base adaptation and occlusion: Even a well fitting base will misbehave if the occlusion drives it off the ridge. Provide clear records and confirm that the vertical dimension and centric relation are stable before sending them to the lab.
- Balanced occlusion: While evidence on occlusal schemes is nuanced, a well executed bilateral balanced scheme for complete dentures tends to minimise tipping forces on the lower plate.
- Major undercuts and bony prominences: Where anatomy causes a rock, consider selective relief or surgical consultation before accepting compromise.
- Digital articulation: When you send accurate interocclusal records with your scans, our team can use virtual articulation to identify and adjust potential interferences before the denture ever reaches the mouth.
Problem 3: Sore spots, ulcers and soft tissue trauma
What it looks like
Post insertion reviews show erythema or ulceration over knife edge ridges, mylohyoid areas, or frenal attachments. Patients report burning, rubbing or difficulty tolerating the denture for more than a few hours.
Practical solutions
- Systematic adjustment protocol: Use pressure indicating paste and methodical reduction rather than “chasing” patient complaints.
- Relines and rebasing: If the denture is fundamentally ill adapted due to tissue changes, a reline or rebase planned with your partner lab is often more effective than endless spot grinding.
- Soft liners for selected cases: For severely resorbed ridges or patients with thin, delicate mucosa, a long term soft liner can improve comfort. Selection of material and thickness is a key lab conversation.
- Systemic factors: Xerostomia, mucosal disease and hygiene issues can amplify minor trauma. Coordinating with the patient’s GP or specialist may be appropriate.
Problem 4: Speech and phonetics complaints
What it looks like
Patients struggle with “s,” “sh,” “f” and “v” sounds, or describe feeling “thick tongued.” Many adapt over time, but persistent speech concerns can drive non wear or social withdrawal.
Practical solutions
- Tooth position: Lower incisor and canine positioning relative to the tongue and upper incisors plays a large role. Neutral zone techniques, phonetic checks at try in, and photos from the previous natural dentition (where available) help.
- Lingual contouring: Overly bulky lingual flanges crowd the tongue. Close collaboration with your lab on lingual contour, particularly in the premolar region, can restore space and improve speech.
- Patient coaching: Simple exercises and reassurance that adaptation often takes weeks, not days, supports compliance. Healthdirect’s overview of dentures can be a handy patient resource.
Problem 5: Chewing inefficiency and frustration
What it looks like
Even if the denture looks textbook-perfect, patients may still say they “can’t chew properly.” They may gravitate to soft diets, cut food finely, or simply stop wearing the lower denture altogether.
Practical solutions
- Occlusal scheme and tooth morphology: Shallow cusps and carefully controlled contacts help keep forces centred over the ridge. Clear instructions about your preferred scheme at the lab slip are invaluable.
- Opposing arch status: A single lower denture opposing natural maxillary teeth or fixed prostheses often faces tougher functional demands than a full denture set.
- Case selection for conventional dentures: For some severely resorbed mandibles, best chewing performance may only be achieved with an implant retained overdenture. Multiple trials have shown improved function and quality of life when two implant overdentures replace conventional mandibular dentures.
Problem 6: Aesthetics and lower facial support
What it looks like
Patients mention “sunken” appearance, inadequate lip support, or dissatisfaction with tooth display at rest and on smiling. Vertical dimension errors, tooth position and ridge resorption all contribute.
Practical solutions
- Vertical dimension: Insufficient vertical dimension can exaggerate folds at the commissures and deepen the nasolabial angle. Thorough records and facebow (where used) give the lab a solid starting point.
- Lower incisor position: Overly lingual placement sacrifices lip support and aesthetics. Again, neutral zone and try in feedback are key.
- Tooth mould and shade: A realistic tooth mould and shade selection, documented with photos and shade tabs, help the lab deliver a result that matches the patient’s expectations.
Problem 7: Fractures, wear and material failure
What it looks like
Midline fractures across the lower denture, chipped or worn posterior teeth, or recurrent tooth debonding. These issues lead to emergency visits and frustrated patients.
Practical solutions
- Reinforcement: For high risk cases (parafunction, very thin ridges, limited vertical space), consider metal reinforcement or high impact acrylic, and specify this when you prescribe the case.
- Material selection: CAD/CAM milled dentures from pre-polymerised PMMA blanks can show better strength and wear resistance compared with conventionally processed acrylics, when used appropriately.
- Occlusal adjustments: Heavy posterior contacts or off axis forces accelerate wear and fractures; early review and occlusal refinement help extend prosthesis life.
When to consider implant-supported lower dentures
At some point, no amount of re-adjusting or relining will meet the patient’s functional expectations with a conventional lower denture. In these cases, discussing an implant retained mandibular overdenture becomes reasonable.

Implant supported lower dentures can significantly improve everyday comfort, chewing and confidence for suitable patients.
The well known McGill consensus statement on overdentures and the York consensus statement on overdentures support mandibular two implant overdentures as a standard option for edentulous patients, with evidence for improved comfort and satisfaction compared with traditional lower dentures. For suitable patients, even two well placed fixtures with locator or bar attachments can dramatically change day to day function.
From a lab perspective, implant overdentures introduce extra variables: attachment type, space, bar design, insertion path but also offer far better prospects for stability. Working with a lab experienced in implant prosthetics lets you plan attachment selection, hygiene access and future maintenance from the outset.
Lab collaboration checklist for smoother lower denture cases
A predictable mandibular denture is rarely an accident. Here is a quick checklist you can use with any lab, and especially with digital labs like NovaDent:
- Clear written prescription: Occlusal scheme, preferred tooth moulds, shade, vertical dimension and any previous issues with the patient’s old prosthesis.
- High quality impressions or scans: Border moulded functional impressions or accurate intraoral scans, with special attention to the retromylohyoid areas.
- Accurate records: Centric relation, vertical dimension, facebow (if used), and opposing arch status (natural, partial, or complete denture).
- Photos: Pre-extraction photos, smile line, rest position, frontal and profile shots help with aesthetics and tooth positioning.
- Try in feedback: Detailed notes at wax try in ( for digital dentures) regarding phonetics, aesthetics and vertical dimension.
- Post insertion communication: Let your lab know about recurring problems so future cases can be refined. A quick email or call can save multiple review appointments down the track.
For clinicians transitioning to digital dentures, structured communication with a digital ready lab partner is especially helpful during the learning curve.
How NovaDent Labs supports your lower denture solutions
As a Sydney based, digitally focused lab, NovaDent works with dentists across Australia on everything from conventional mandibular dentures to two implant overdentures and full arch solutions.

Digital workflows and close lab clinician collaboration help reduce lower denture problems and remakes.
With CAD/CAM workflows, AI assisted design and compatibility with all major intraoral scanner files, we can help you:
- Standardise your lower denture protocols for impressions, records.
- Reduce chairside adjustment time through better base adaptation and occlusal planning.
- Plan implant retained with appropriate attachment systems and space analysis.
- Manage remakes and relines efficiently while keeping communication straightforward.
If you’d like to compare turnaround times, materials and pricing, you can request a price list or contact our lab team to talk through a specific lower denture case.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website