For many patients, the day they lose their teeth is the same day they receive their new immediate denture. Clinically, you are juggling extraction complexity, healing and occlusion; emotionally, they are juggling fear about pain, eating and their appearance. When those expectations are not lined up, the next review visit can feel long for everyone in the room.
This guide is written for dentists and teams who want to give clear, realistic pre‑op conversations and practical take home instructions. We will walk through what patients typically feel at each stage, how full and immediate partial denture cases differ, and how your lab partnership can smooth a stressful week into a manageable treatment journey.
TL;DR
- Explain that an immediate prosthesis is a temporary solution over a changing ridge, not the “final denture”.
- Prepare patients for normal post extraction symptoms: pressure, speech changes and sore spots.
- Use simple written immediate denture instructions that cover wearing time, cleaning and red flag symptoms.
- Plan ahead for soft liners, relines and, in many cases, a future definitive denture.
- Work with a lab that supports you on design, occlusion and turnaround for immediate and removable prosthetics.
What is an immediate denture?
In simple terms, an immediate prosthesis is placed on the same day teeth are removed. Impressions, jaw relations and shade selection are completed while teeth are still present. The lab sets teeth on the anticipated ridge form, then the prosthesis goes in once extractions and any alveoplasty are complete.
Compared with a conventional denture fabricated on a healed ridge, you are working with more guesswork around tissue changes and less chance to trial the setup with the patient. A clear story about “temporary” versus “definitive” makes a big difference. Linking this to written materials from trusted groups such as the Australian Dental Association or the Oral Health Foundation can reinforce your message. For clinicians who want more technical background, a clinical report on immediate dentures illustrates one protocol step by step.
For clinicians using digital impressions, a lab with CAD/CAM workflows for digital dentures and partials can streamline this process and reduce surprises on the day of surgery.
Why patient expectations matter so much
Think of the patient who walks in convinced they will “walk out with perfect teeth and chew steak tonight”. Even if the surgery and prosthesis are textbooks, that mismatch between expectation and reality sets you up for stress, remakes, and a shaky relationship.
On the other hand, when patients know in advance that speech will sound strange, that chewing will be limited at first, and that follow up visits are part of the plan, they read normal side effects as “expected” instead of “something has gone wrong”. A short, well structured handout or link to a resource on your website or your lab’s site (for example, a patient facing guide like our full mouth dentures overview) reinforces what you say in the chair.
Step by step: what patients feel after extraction
Every case is different, but a simple timeline helps patients anchor what they are experiencing. Here is a pattern you can adapt to your own protocols.

Clear written instructions help patients navigate the first days and weeks after extractions.
Day 0–3: Surgery and early healing
- Immediate full or immediate partial denture is placed at the end of surgery.
- Patients feel firm pressure from the prosthesis over the extraction sites.
- Swelling, bruising and blood tinged saliva are common messages to the practice.
- Speech sounds thick, with extra saliva and gag reflex for some.
- Chewing is usually limited to soft, cool foods on the non surgical side.
Week 1–2: Sore spots and adjustments
- Swelling begins to settle; the denture starts to feel slightly looser.
- Sore spots appear along flanges, frenal areas and load bearing ridges.
- You may relieve pressure points, adjust occlusion and consider a tissue conditioner.
- Patients start to test more foods and speak more in social settings.
Month 1–3: Ridge remodelling
- Bone and soft tissue shrink, particularly in the first three months.
- Retention and stability drop, especially in full immediate dentures.
- Reline or remake planning becomes a focus of visits.
- For an immediate partial denture, clasps and rests may need review as teeth and contacts settle.
Beyond 3 months: Toward a definitive solution
- Tissue changes slow and a long term prosthetic plan comes into view.
- Many patients move to a definitive complete or partial prosthesis, or to an implant supported option.
- A lab that understands your implant systems and restorative preferences, such as NovaDent’s implant restorations service, can help you map this with the patient.
“An immediate prosthesis is a phase of treatment, not the final word on a patient’s smile.”
Full immediate dentures vs immediate partial denture after extraction
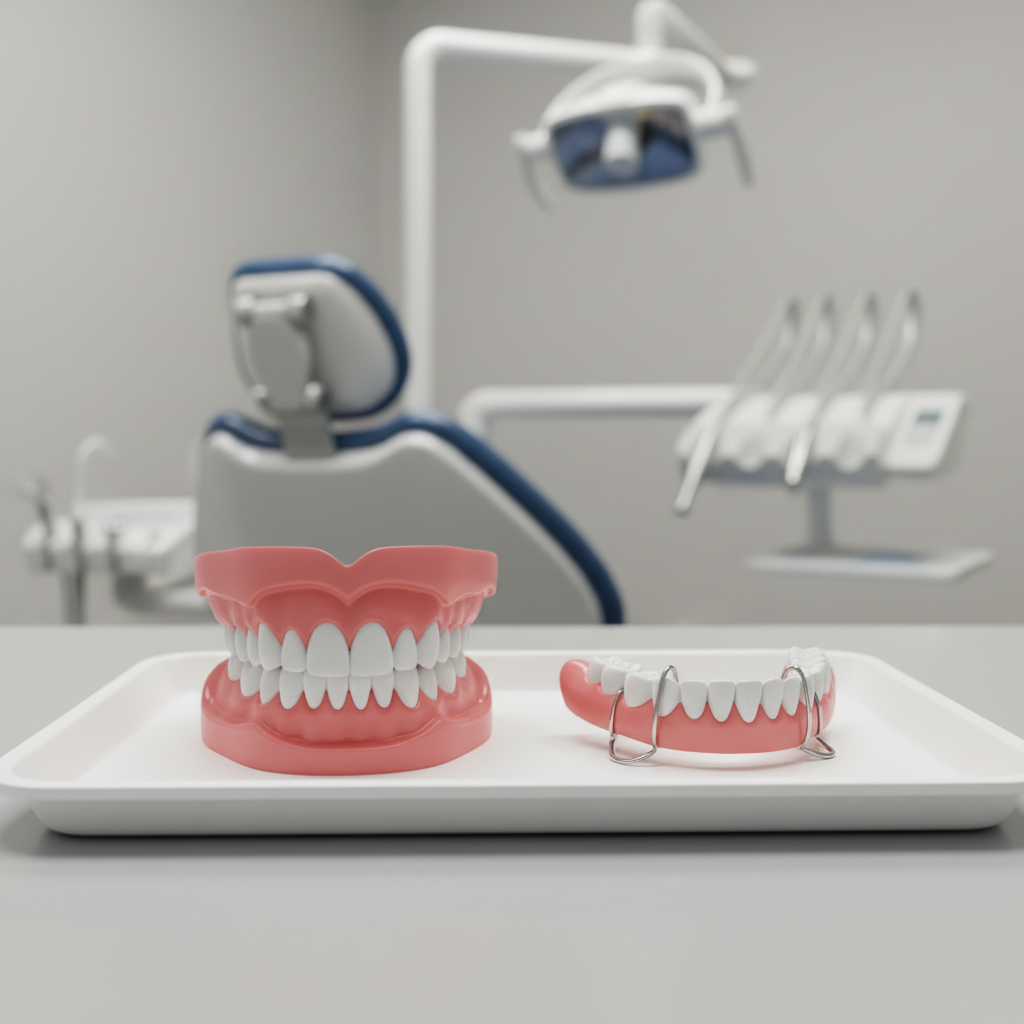
Full immediate dentures and immediate partial dentures each bring different design and patient expectations.
A full immediate prosthesis replaces an entire arch the day teeth are removed. Esthetics are often the patient’s main worry here, especially if anterior teeth are involved. You balance lip support, phonetics and vertical dimension with surgical access and healing.
An immediate partial denture after extraction comes with a slightly different story. Remaining teeth can support the prosthesis, but they also bring questions about caries risk, periodontal status and clasp design. Talk through how those remaining teeth may feel under new occlusal contacts, and how future extractions could change the design. Sharing visual examples from your own cases or from your lab’s removable prosthetics case gallery can help patients picture the plan realistically.
Immediate denture instructions you can share
Many patients remember only fragments of verbal post‑op explanations. A short, plain English sheet of immediate denture instructions, paired with your consent form, often pays for itself in fewer emergency calls.
Wearing time
- First 24 hours: in many protocols, the prosthesis stays in place until you remove it at the review visit.
- After the first review: usually worn most of the day and night at first, with planned breaks for cleaning.
- Later phases: once healing stabilises, many clinicians suggest removing it for sleep, guided by individual risk factors.
Cleaning and care
- Rinse the mouth gently with prescribed mouthwash or salt water after the initial period, as your surgical instructions state.
- Clean the prosthesis over a sink partly filled with water or a towel, to reduce the chance of fracture if it slips.
- Use a soft brush and non‑abrasive cleaner, not regular toothpaste, which can scratch acrylic.
- Soak in a recommended denture cleaning solution according to the manufacturer’s directions.
Eating and speaking
- Start with soft, cool foods cut into small pieces.
- Chew slowly and evenly on both sides where possible.
- Expect extra saliva and speech changes; reading aloud at home often helps patients regain control.
When to contact the practice
- Persistent pain that does not ease with your recommended analgesics.
- Ulcers or sore spots that prevent wearing the prosthesis.
- Prosthesis that feels suddenly much looser or cannot be seated fully.
- Signs of infection such as increasing swelling, heat or systemic symptoms.
You can build these points into your own branded handout or patient information sheet, so patients hear a consistent message from your practice and your lab partners.
Fit changes, relines and long‑term planning
Because post extraction bone resorption is fastest in the first months, movement and loss of retention are not a sign of lab error; they are a normal part of biology. Textbook data from sources such as a ridge resorption overview suggest that within the first year after full extractions, the alveolar ridge can lose roughly 25–50% of its width (around 5–7 mm) and about 4 mm of height, with much of that change occurring in the first 3–6 months. Framing soft liners, temporary relines and eventual definitive work as planned stages, not “repairs”, helps patients understand the full treatment arc.
Discuss early how long you expect this prosthesis to serve, and when a reline or remake is likely. Clinical case reports suggest that extraction sockets typically take around 4–5 months to regain their contour, with interim immediate dentures often needing repeated relining over 4–6 months before a definitive prosthesis is stable. A quick line on your consent form about a later definitive prosthesis, plus a note about expected timelines, gives you something to refer back to if funding discussions become tense. Your lab can help with case planning, material choices and turnaround times for each stage.
How NovaDent Labs supports your immediate cases

Your lab partner’s planning and communication can smooth immediate denture cases for both clinician and patient.
At NovaDent Labs we see immediate full and immediate partial denture cases from clinics across Australia every week. Our team combines clinical and laboratory backgrounds, which means we think about how your patient feels in the chair as well as how the case looks on a model or screen.
From digital or traditional impressions, we help with tooth selection, occlusal schemes and design for immediate and conventional dentures. We can work directly from intraoral scanner files, support you with implant transition plans, and keep you updated on each case so you can give patients confident timelines.
FAQs
How long should patients expect to feel “strange” with an immediate denture?
Many report that the first 48–72 hours feel very foreign. Most adapt to basic speech and smiling over one to two weeks, while chewing and social confidence often build over several weeks. Linking this to your review schedule helps them see a path forward.
What is different about immediate partial denture care?
An immediate partial denture introduces new forces to remaining teeth and gingiva. Stress good home care for those teeth, flossing patterns around clasps, and the need for regular checks of periodontal and caries status. A brief mention of how this links into their usual recall visits keeps hygiene on the agenda.
Can patients sleep with their immediate prosthesis?
Many clinicians keep it in place overnight at first for haemostasis and adaptation, then transition to removing it for sleep once healing allows. The key is consistent, written instructions that match what staff say over the phone.
How should dentists frame costs around immediate and definitive work?
One practical approach is to present the immediate prosthesis, planned relines and the future definitive solution as a single phased plan. A clear estimate for each stage, along with options such as implant supported prostheses where indicated, reduces surprise and builds trust.
When patients understand that their immediate prosthesis is the first step in a longer restorative plan, they read normal post extraction experiences as part of healing instead of as treatment failure. Clear explanation, simple written instructions and a lab partner who supports your protocols go a long way toward calmer review visits and happier patients.
If you would like support with your next full or immediate partial denture case, you can request our price list or contact the NovaDent team for a case discussion.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website