Most days in surgery, crown material choice feels routine. Then the parafunctional molar, metal sensitised patient or high smile line case lands on your list and suddenly pfm crowns vs zirconia crowns is no longer an abstract debate it’s a remake, a fracture or an unhappy review waiting to happen.
This guide steps through the real differences between porcelain fused to metal (PFM) and zirconia crowns in terms of strength, aesthetics, prep design and lab workflow. The goal is simple: give you a clear, chairside framework so you can match the material to the mouth with less second guessing and fewer remakes.
TL;DR:
- Strength & survival: Both PFM and zirconia show 5 year survival rates in the mid 90% range when used within indications.
- Fracture patterns: PFM tends to chip at the porcelain veneer; monolithic zirconia more often fails as rare bulk fractures.
- Aesthetics: Layered zirconia usually outperforms PFM for high smile line cases; PFM can show a grey cervical line over time.
- Posterior workhorses: Monolithic zirconia is usually the first choice for high load molars and bruxers.
- Legacy strengths: PFM still has a role in long‑span bridges, limited clearance with metal occlusals, and cases where decades of data matter.
- Best results: Come from pairing the right material with sound prep, occlusal design and a digitally focused lab, not from the material alone.
PFM and zirconia crowns: quick overview
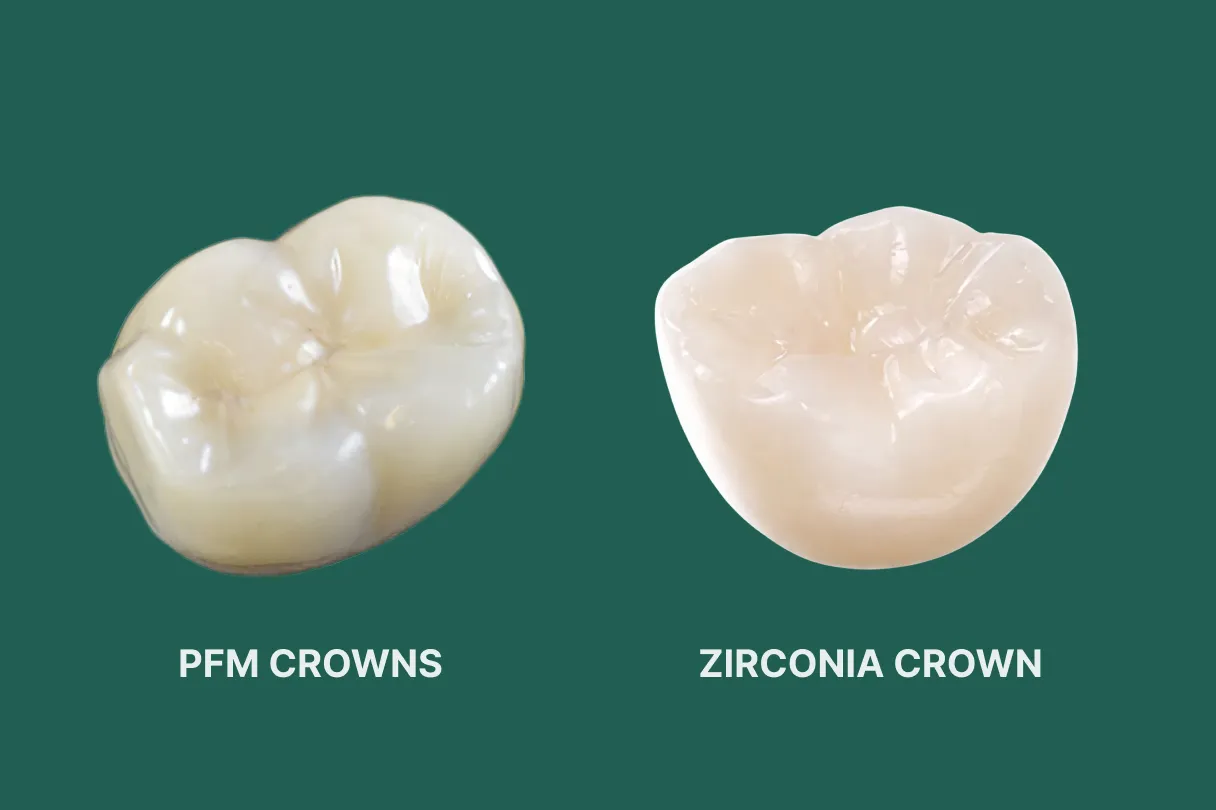
What is a PFM crown?
A porcelain fused to metal crown has a cast metal coping with a fired porcelain veneer. The metal substructure delivers strength and can be very thin, while porcelain provides contour and shade. PFM has decades of clinical data with high long‑term survival on both anterior and posterior teeth, including a 5 year evaluation of complications and survival in porcelain fused to metal crowns.
Typical indications include full coverage crowns and bridges where you want reliable support under high occlusal load, especially when using metal occlusal surfaces or when connector dimensions are tight.
What is a zirconia crown?
Zirconia crowns use yttria stabilised tetragonal zirconia polycrystal (Y‑TZP). Monolithic zirconia (full contour) is milled from a solid block and then sintered, giving flexural strength often in the 900–1200 MPa range roughly two to three times that of many veneering porcelains, as shown in vitro fracture load testing of translucent zirconia crowns.
Modern zirconias come in multiple translucency levels and multilayer discs, so you can choose between high strength posterior options and more aesthetic anterior formulations. At NovaDent’s fixed prosthetics service, zirconia, PFM, PFZ and e.max are all available on the same digital workflow, which lets you switch materials without redesigning the entire case.
PFM vs zirconia crowns: key differences at a glance
For a more ceramic focused comparison, you can cross reference this with NovaDent’s Emax vs zirconia crowns guide, which looks at glass ceramics versus zirconia in similar detail.
Strength, longevity and complications
Posterior examinations help identify which crown material will best handle occlusal load over time.
What does the evidence say about survival?
Systematic reviews and cohort studies report 5 year survival rates for tooth supported PFM crowns and all ceramic crowns (including zirconia) typically in the 90–97% range when cases are well selected, as summarised in an NCBI review of porcelain fused to metal versus all ceramic crowns. More recent clinical work comparing monolithic zirconia with PFM in posterior teeth has found survival around 95–98% for zirconia and similarly high rates for PFM, particularly in well designed single crowns and short span bridges.
How do they fail?
- PFM crowns: The classic complication is porcelain chipping or fracture, with the metal coping still intact. Marginal discoloration and exposure of the metal collar are also common findings over time.
- Zirconia crowns: Monolithic zirconia largely removes the veneer chipping issue. When failures occur, they tend to be bulk fractures or problems related to design (connector size, sharp internal angles, inadequate thickness) rather than slow chipping.
For everyday practice, this means that zirconia vs PFM crowns is less about “which one breaks” and more about where and how they are likely to fail if pushed beyond their comfort zone.
In treatment planning, it is often more productive to ask “Is this a good crown case?” before “Is this a zirconia or PFM case?” Large cores with uncertain ferrule, uncontrolled parafunction, poor moisture control or compromised periodontal support tend to fail regardless of material choice. When these risk factors are addressed for example by improving ferrule, controlling bruxism with a guard, or staging periodontal treatment first survival rates for both zirconia and PFM rise, and the material decision becomes more about aesthetics and workflow.
For a deeper literature scan between sessions, the NCBI Bookshelf summary on metal ceramic versus all ceramic crowns and a retrospective survey on long‑term survival of posterior zirconia and PFM crowns provide good starting points.
Aesthetics and patient expectations

Conversations about zirconia vs PFM crowns often centre on how the final smile will look.
Anterior zone: where appearance rules
In the smile line, the main limitation of PFM is optical: the metal coping can make it harder to reproduce natural translucency, and a dark line may appear at the gingival margin if tissue recedes or the collar becomes exposed.
Multilayer zirconia offers a more forgiving cervical zone and lets you bring incisal translucency closer to adjacent enamel. When the patient’s first question is “Will anyone see the crown?”, zirconia usually has the edge over classic PFM, especially when your lab controls thickness and shade digitally, as with NovaDent’s zirconia crown range.
Posterior zone: aesthetics vs function
In posterior zones, aesthetics matter but rarely override function. A monolithic zirconia crown with careful staining and glazing is usually more than acceptable cosmetically and brings a high safety margin against fracture. Many clinicians in Australia now use zirconia as their default posterior crown and reserve PFM for specific structural reasons, such as very limited occlusal clearance with metal occlusals or long span bridges where they like the behaviour of a metal framework.
Prep design, occlusion and indications
Preparation: how much reduction?
While exact numbers depend on the system you use, PFM crowns generally need space for both metal and porcelain. That often means around 1.5–2.0 mm occlusal reduction and roughly 1.2 mm axial, with either a heavy chamfer or shoulder to support the porcelain, in line with fixed prosthodontic preparation guidelines.
Monolithic zirconia can often work at slightly lower thickness in low risk zones, thanks to its higher flexural strength, though aesthetic zirconias in the anterior still benefit from generous reduction. NovaDent’s team regularly reviews intraoral scans and helps clinicians confirm minimal thicknesses before you commit to a prep, similar to the scanner‑first approach described in their crown prep workflow guide.
Occlusion, parafunction and contact design
For bruxers, heavy clenchers and short clinical crowns, zirconia’s strength and the ability to keep copings thinner make it a logical choice, provided the occlusion is thoughtfully adjusted and polished. Well‑polished zirconia is kinder to opposing enamel than rough, glazed surfaces, which is worth remembering when you are refining contacts chairside.
PFM still earns its place where metal occlusals or long span frameworks are preferred, and where you want the forgiving behaviour of a ductile metal framework under stress.
Cost, turnaround and lab workflow

Digital workflows streamline planning and fabrication for both PFM and zirconia crowns.
Many Australian labs now price monolithic zirconia and PFM along with other dental crown cost crowns in a similar band, with variations for alloy type and translucency. In a digital lab like NovaDent, zirconia integrates neatly with CAD/CAM design, nesting and milling, which helps keep remake rates low and contacts repeatable across cases.
For your own scheduling, NovaDent’s turnaround time guide lists typical lab days for zirconia, PFM and implant crowns. When you combine that with digital case submission via the Submit a Case portal, you can set clearer expectations with patients and reduce the “is my crown back yet?” calls.
If you are moving into a scanner first model, NovaDent’s intraoral scanner connection guide walks through how to connect Trios, Medit, Primescan, iTero and others, so PFM vs zirconia decisions sit on top of a reliable digital foundation.
Decision checklist: zirconia vs PFM in daily practice
When you are mid prep and time is tight, a quick mental checklist helps more than a textbook chapter. Here is a simple framework many NovaDent clinicians use when weighing zirconia vs PFM crowns:
- Zone: High smile line anterior? Favour multilayer zirconia. Low smile line molar? Monolithic zirconia or PFM with metal occlusal both work.
- Load & parafunction: Heavy grinder or history of fractures? Lean toward monolithic zirconia plus an occlusal guard.
- Span length: Long bridge with minimal connector bulk? PFM framework may still be the safer option.
- Clearance: Very limited space? Metal occlusal PFM or conservative zirconia (confirmed with your lab) are candidates.
- Tissue and smile line: High risk of recession in a high smile line case? Metal collar exposure becomes a real aesthetic issue; zirconia helps here.
- Workflow: Working digitally with NovaDent? Sending photos and scans lets the lab suggest material and thickness before you finalise prep.
In practice, many dentists settle on a hybrid protocol: zirconia for most posterior units, PFM where metal frameworks still shine, and glass ceramics where bonding and translucency matter most.
FAQs
Are zirconia crowns more durable than PFM crowns?
In terms of flexural strength, yes: monolithic zirconia is significantly stronger than typical feldspathic porcelains used over PFM copings. Clinically, both materials show excellent survival when correctly indicated. Zirconia tends to have fewer veneer chipping events because there is no separate porcelain layer in full contour designs, while PFM has an exceptionally long evidence base with proven performance over decades.
Can I mix zirconia and PFM crowns in the same arch?
Yes. Many full mouth rehabilitations combine materials: for example, PFM for long span bridges and zirconia for single posterior crowns. The main considerations are occlusion, connector design, opposing materials and aesthetic consistency. Working with one lab for the whole case helps harmonise shade and contour irrespective of material.
What do I tell patients when they ask which material is “better”?
A simple script that works well is: “Both options are strong and long lasting. This one is slightly stronger, this one can look a little more like a natural tooth in your smile. Together we’ll choose the option that best fits your bite, your smile line and how hard you are on your teeth.” That keeps the focus on matching the material to their mouth rather than trying to crown a single “winner”.

NovaDent Has Arrived.
Previously VTS Dental Labs.
Same team
Same standards
New identity
Visit our new website